Foot and Ankle Surgery — MCQs

On this page
Watson Jones operation is indicated for which condition?
Triple arthrodesis does not involve which of the following joints?
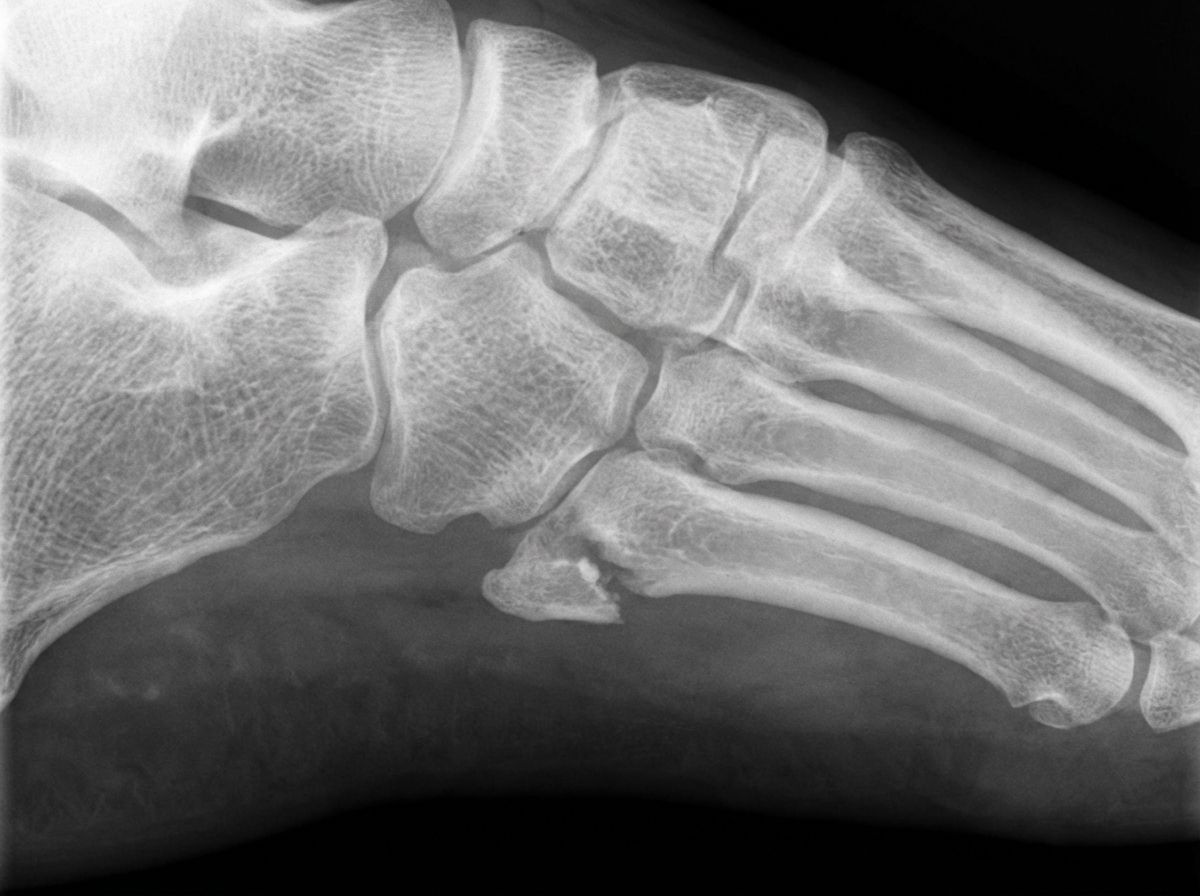
A 45-year-old male presents with foot pain after an injury. What is the mechanism of injury associated with the pathology seen in this X-ray?
Hallux valgus is associated with all of the following except:
A 32-year-old athlete presents with posterior heel pain. Which of the following could be a differential diagnosis?
What happens to Gissane's angle in an intraarticular fracture of the calcaneum?
A patient presents with a hindfoot deformity requiring triple arthrodesis. Which of the following bones are fused in a triple arthrodesis?
Radiographic examination of a woman with foot pain reveals a neuroma. What is the most typical location of this neuroma?
What does equinus deformity refer to?
Triple orthodesis consists of fusion of which three joints of the foot?
Practice by Chapter
Foot and Ankle Anatomy
Practice Questions
Hallux Valgus
Practice Questions
Flatfoot Deformities
Practice Questions
Cavus Foot
Practice Questions
Ankle Instability and Sprains
Practice Questions
Achilles Tendon Disorders
Practice Questions
Diabetic Foot
Practice Questions
Foot and Ankle Arthritis
Practice Questions
Ankle Fractures
Practice Questions
Foot Fractures
Practice Questions
Tendon Disorders of Foot and Ankle
Practice Questions
Reconstructive Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
