Osteoarthritis of Shoulder — MCQs

Which of the following is the most common cause of secondary osteoarthritis?
A 30-year-old woman complains of bilateral pain and stiffness in the small joints of her hands, worse in the morning and improving throughout the day. What is the most likely diagnosis?
Treatment of choice in a 65-year-old female with impacted fracture of the neck of the humerus is:
A 40-year-old presents with chronic shoulder pain and restricted ROM. X-ray shows decreased joint space. Most likely diagnosis?
Which of the following statements about osteoarthritis is false?
Osteoarthritis not seen in ?
A 55-year-old woman presents with widespread pain, fatigue, and sleep disturbances. Physical examination reveals multiple tender points. What is the most likely diagnosis?
Which of the following joints are commonly affected in osteoarthritis? I. First metatarsophalangeal joint II. Proximal interphalangeal joint III. Ankle joint IV. 5th and 6th cervical vertebrae joint Select the correct answer using the code given below :
79 yrs old lady had fall, the following X-ray was taken. Which of the following is treatment?
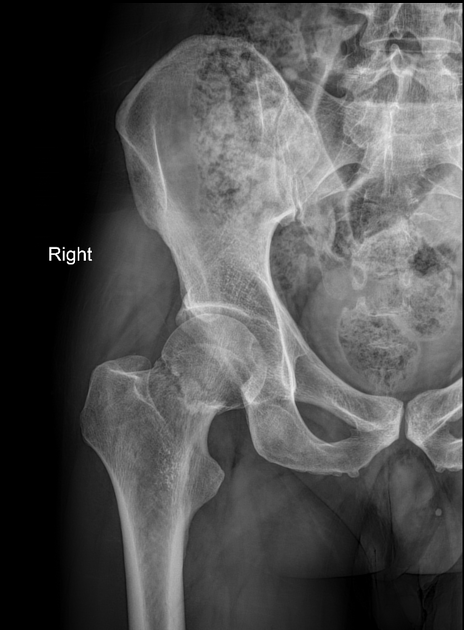
What is the best treatment for a 60-year-old man with intracapsular femoral neck fracture?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
