Bone Tumors — MCQs

On this page
Which test is used for posterior dislocation of the glenohumeral joint?
Which solitary bone lesion does not arise from the metaphysis?
Sunray appearance on X-ray may be seen in:
A patient with a history of Road Traffic Accident (RTA) two years ago developed pain and swelling at the same site in the leg. X-ray shows certain features. What is the most likely diagnosis?
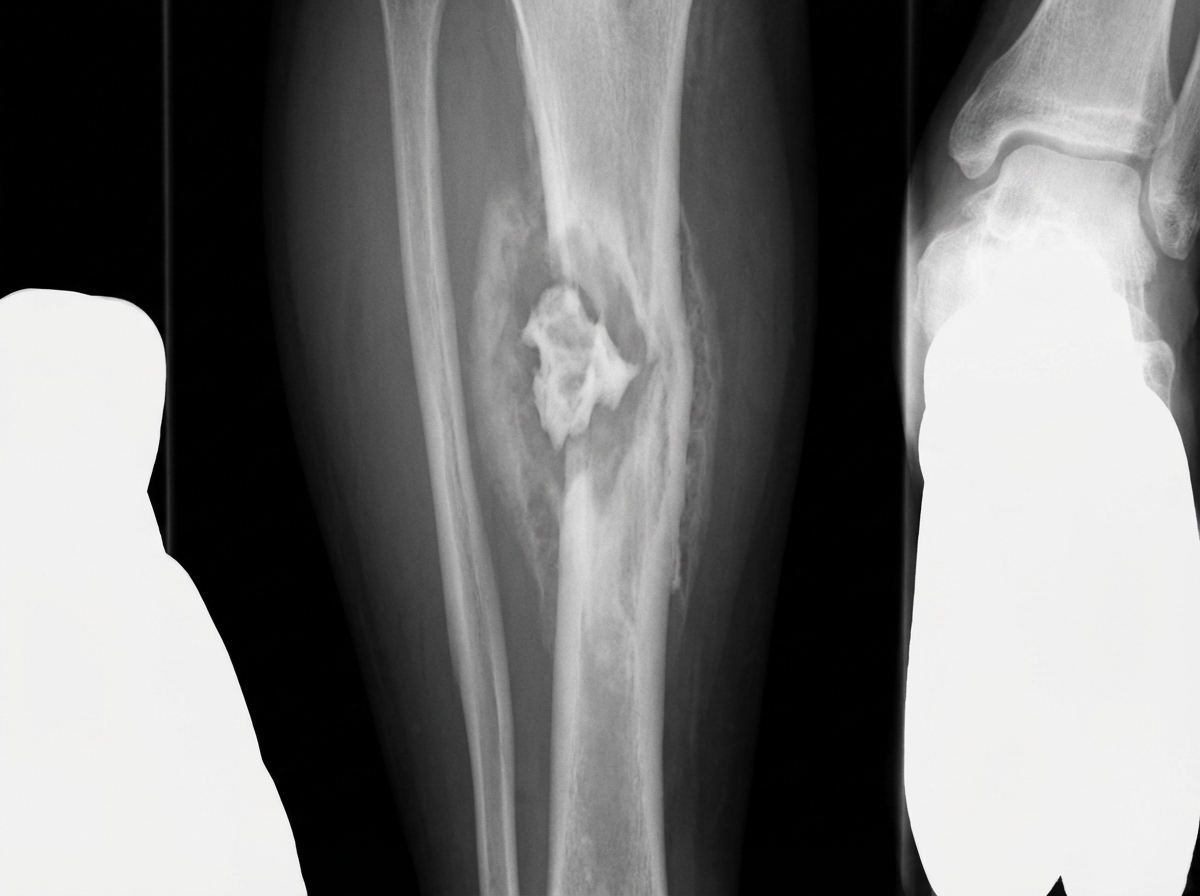
Which of the following conditions is considered a premalignant condition for secondary osteosarcoma?
Which tumors are known to produce expansile bony metastases?
New periosteal bone formation can be seen in which of the following conditions?
Which of the following is NOT a non-neoplastic lesion that simulates a bone tumor?
Which of the following is NOT a diaphyseal tumor?
What is the most serious complication of Paget's disease?
Practice by Chapter
Classification of Bone Tumors
Practice Questions
Benign Bone Tumors
Practice Questions
Malignant Primary Bone Tumors
Practice Questions
Metastatic Bone Disease
Practice Questions
Tumor-Like Lesions of Bone
Practice Questions
Soft Tissue Tumors
Practice Questions
Evaluation and Staging of Bone Tumors
Practice Questions
Biopsy Principles
Practice Questions
Limb Salvage Surgery
Practice Questions
Amputation for Bone Tumors
Practice Questions
Adjuvant Therapies
Practice Questions
Surveillance and Follow-up
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
