Bone Tumors — MCQs

On this page
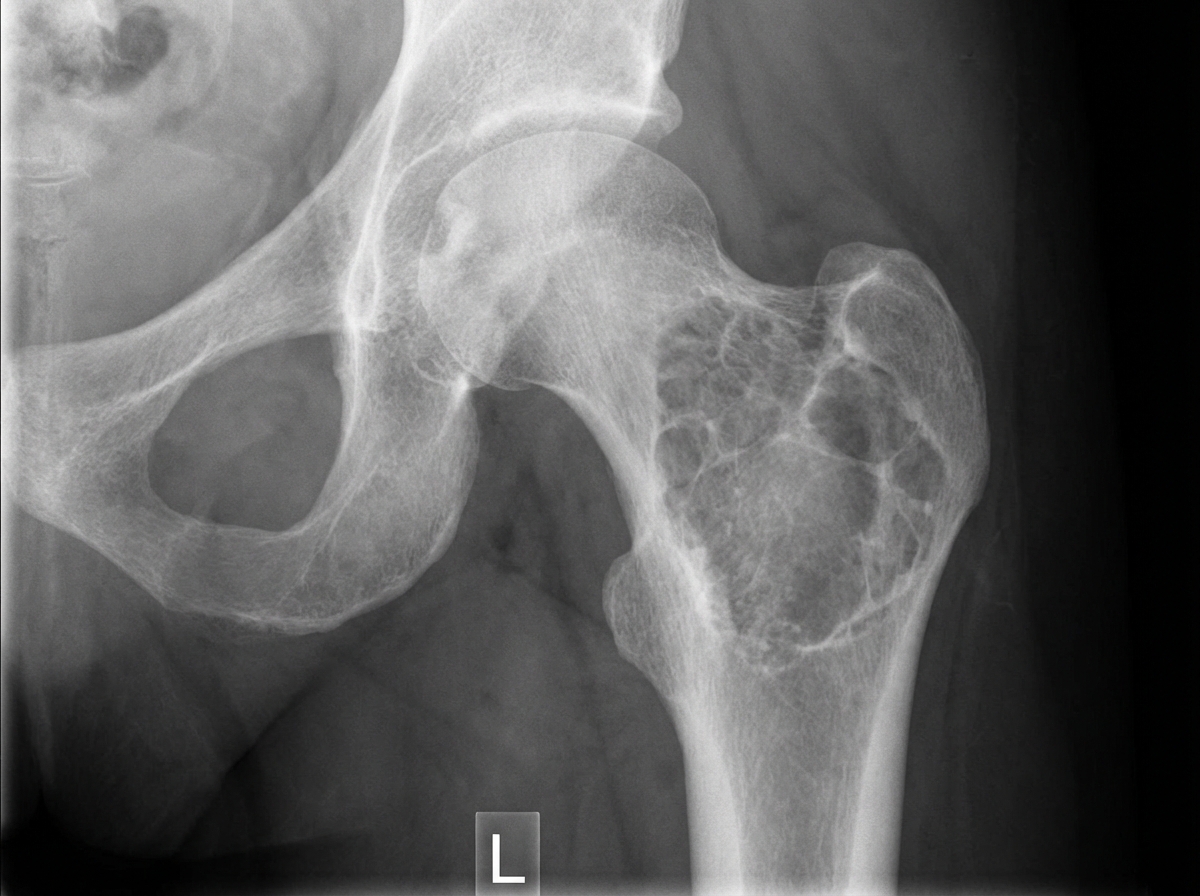
A 30-year-old male presented with hip pain for the last 6 months. A hip X-ray is provided. What is the likely diagnosis?
Which of the following is a pulsatile tumor?
What is the most common primary site of a metastatic bone tumor in males?
Which of the following is not a type I geographic lesion of bone?
Which of the following conditions shows a sun ray appearance on imaging?
What is true about Ameloblastoma?
Which of the following tumors is associated with raised serum alkaline phosphatase levels?
Mazabraud's syndrome is defined as:
What is the standard surgical staging system for bone tumors?
A specimen shows a stalk-like resection of a pedunculated bony swelling. What is the most likely diagnosis?
Practice by Chapter
Classification of Bone Tumors
Practice Questions
Benign Bone Tumors
Practice Questions
Malignant Primary Bone Tumors
Practice Questions
Metastatic Bone Disease
Practice Questions
Tumor-Like Lesions of Bone
Practice Questions
Soft Tissue Tumors
Practice Questions
Evaluation and Staging of Bone Tumors
Practice Questions
Biopsy Principles
Practice Questions
Limb Salvage Surgery
Practice Questions
Amputation for Bone Tumors
Practice Questions
Adjuvant Therapies
Practice Questions
Surveillance and Follow-up
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
