Bone Tumors — MCQs

On this page
In the treatment of osteosarcoma, all of the following chemotherapy agents are used EXCEPT:
Which of the following statements is true regarding hemangioma of the bone?
What is the most common bone involved in hemangioma?
Which of the following is NOT an epiphyseal tumor?
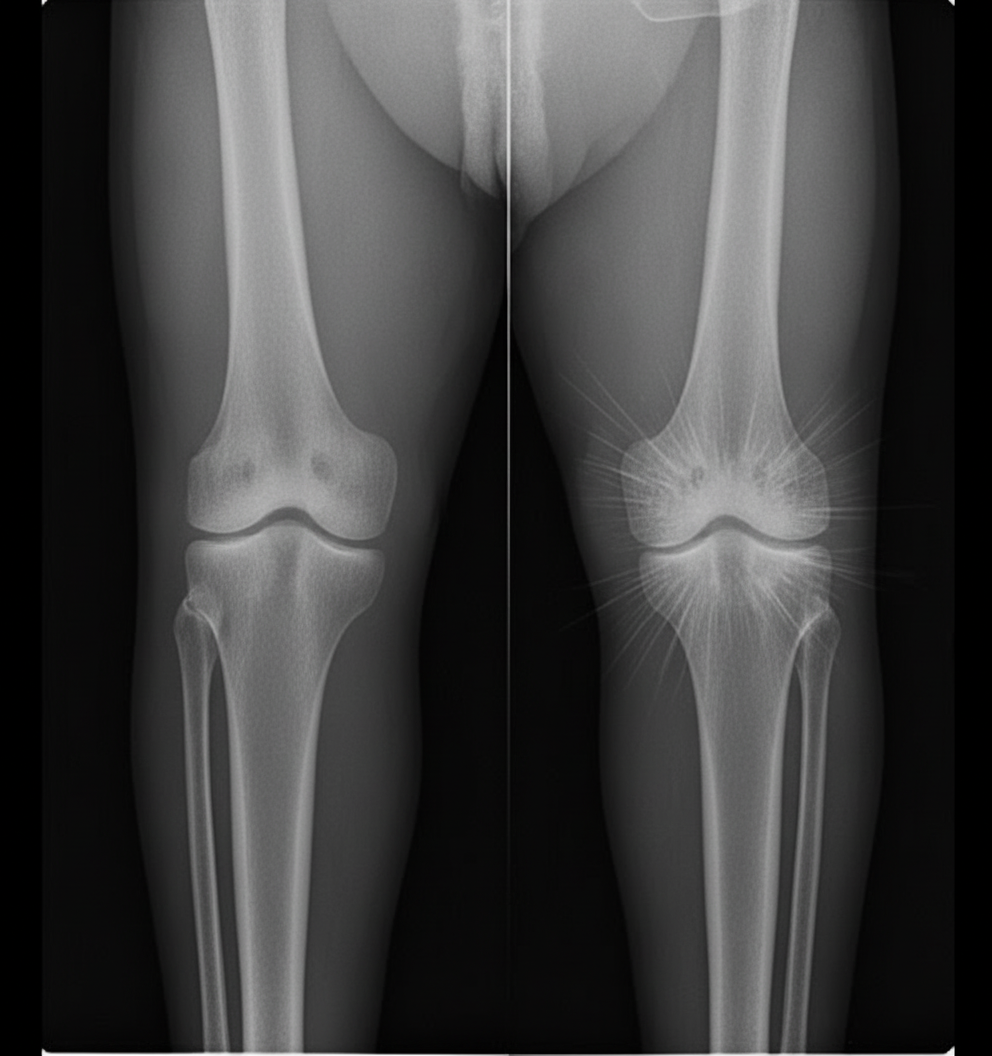
A 25-year-old male presents with right knee swelling of one month duration. A radiograph is provided. Which of the following statements is true regarding this condition?
Which of the following bones is not a common site for metastasis?
Which of the following bone tumors is radiosensitive?
Which of the following organs is usually the first site of metastasis in a case of osteosarcoma in a young female?
A 12-year-old girl complains of leg pain persisting for several weeks with a low-grade fever. A radiograph reveals a mass in the diaphyseal region of the left femur with overlying cortical erosion and soft tissue extension. A biopsy of the lesion shows numerous small round cells, rich in PAS-positive diastase-sensitive granules. What is the most likely histological diagnosis?
What is the most common site of a March fracture?
Practice by Chapter
Classification of Bone Tumors
Practice Questions
Benign Bone Tumors
Practice Questions
Malignant Primary Bone Tumors
Practice Questions
Metastatic Bone Disease
Practice Questions
Tumor-Like Lesions of Bone
Practice Questions
Soft Tissue Tumors
Practice Questions
Evaluation and Staging of Bone Tumors
Practice Questions
Biopsy Principles
Practice Questions
Limb Salvage Surgery
Practice Questions
Amputation for Bone Tumors
Practice Questions
Adjuvant Therapies
Practice Questions
Surveillance and Follow-up
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
