Basic Science in Orthopaedics — MCQs

On this page
Wolff's law states that:
Who coined the term orthopaedics?
What is the difference between neuropraxia and axonotmesis?
All are true regarding bone remodeling, EXCEPT:
Myositis ossificans is differentiated from other reactive fibroblastic proliferations by the presence of?
Which of the following changes occurs during bone growth?
All of the following cause osteonecrosis except?
What type of joint is the inferior tibiofibular joint?
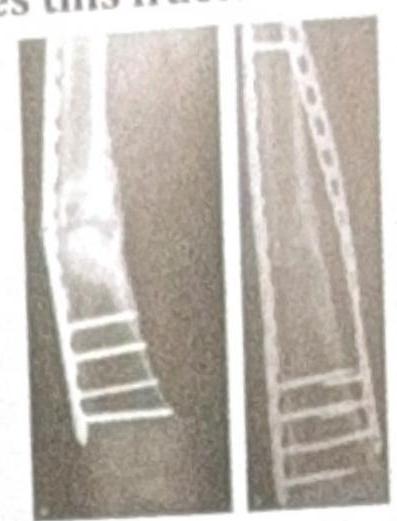
The X-ray shows plating done for a fracture. How does this fracture heal?
If the outer sheath and nerve fibres are intact and the inner axon is damaged, it is known as
Practice by Chapter
Bone Structure and Function
Practice Questions
Cartilage Biology and Physiology
Practice Questions
Muscle and Tendon Physiology
Practice Questions
Joint Biomechanics
Practice Questions
Fracture Healing Process
Practice Questions
Bone Metabolism and Turnover
Practice Questions
Orthopaedic Biomaterials
Practice Questions
Tribology in Orthopaedics
Practice Questions
Gait Analysis
Practice Questions
Biomechanics of Spine
Practice Questions
Applied Surgical Anatomy
Practice Questions
Bone Banking and Grafting
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
