Bone Metabolism and Turnover — MCQs

Osteoclasts have all of the following functions except -
Estrogen administration in a menopausal woman increases the:
What is the primary organic component of bone?
The most important regulator of serum 1,25(OH)2 vitamin D concentration is:
A patient is on a low calcium diet for 8 weeks. Which of the following increases to maintain serum calcium levels?
Most metabolically active part in bone is
The success of estrogen and estrogen-like drugs in combating osteoporosis in postmenopausal women may indicate that estrogen:
The X-ray shows plating done for a fracture. How does this fracture heal?
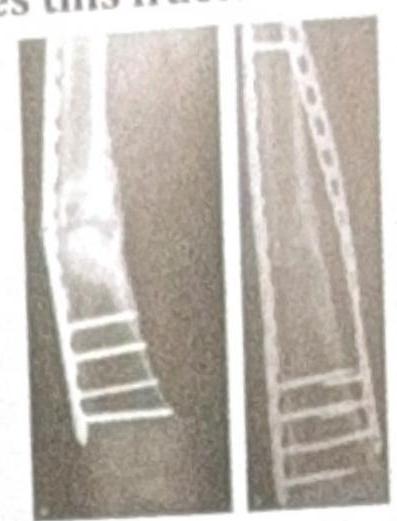
The compression fracture is commonest in
Fracture at which site affects the longitudinal growth of a bone?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
