Arthroplasty — MCQs

On this page
Metal on metal articulation in arthroplasty should be avoided in which of the following scenarios?
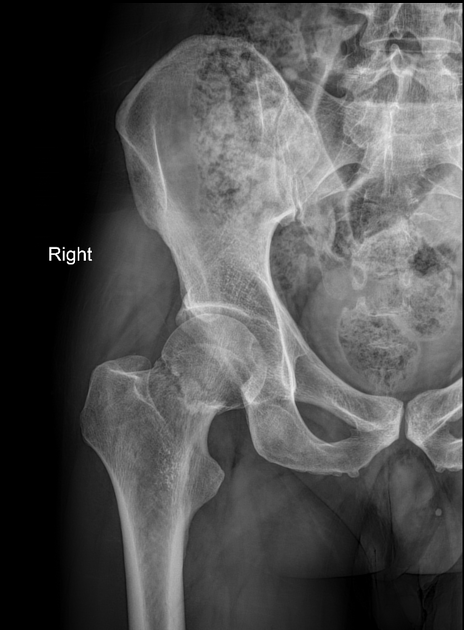
79 yrs old lady had fall, the following X-ray was taken. Which of the following is treatment?
The most common approach for total hip arthroplasty is
All of the following factors affect osseointegration EXCEPT:
Severe disability in primary osteoarthritis of hip is best managed by -
Watson Jones Operation is the procedure for which of the following conditions?
A 65-year-old lady presented with a swollen and painful knee. On examination, she was found to have grade III osteoarthritic changes. What is the best course of action?
What is the most common complication after total hip replacement?
A 65-year-old presents with chronic knee pain, varus deformity, and medial joint space narrowing. BMI is 32. Best treatment option?
Why is early mobilization important after hip arthroplasty?
Practice by Chapter
Principles of Joint Replacement
Practice Questions
Total Hip Arthroplasty
Practice Questions
Total Knee Arthroplasty
Practice Questions
Shoulder Arthroplasty
Practice Questions
Elbow Arthroplasty
Practice Questions
Ankle Arthroplasty
Practice Questions
Revision Arthroplasty
Practice Questions
Implant Materials and Design
Practice Questions
Complications of Arthroplasty
Practice Questions
Infected Arthroplasty Management
Practice Questions
Rehabilitation After Arthroplasty
Practice Questions
Long-term Outcomes and Surveillance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
