Refractive Surgery — MCQs

On this page
What is the typical wavelength of a femtosecond laser used in ophthalmic procedures?
What type of laser is used in LASIK?
What type of laser is used in LASIK surgery?
LASIK (Laser assisted in situ keratomileusis) is useful in the treatment of which of the following refractive errors?
A 35-year-old patient underwent LASIK surgery for myopia correction 2 weeks ago. The patient now complains of glare and halos around lights at night. Visual acuity is 20/25 bilaterally. What is the most appropriate next step in management?
Which of the following lasers is used in refractive surgery?
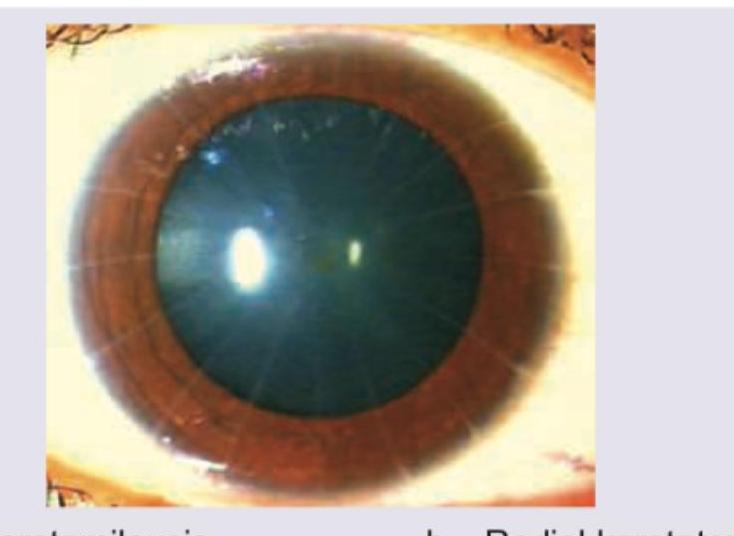
What does the given image show?
A 15-year-old girl with myopic astigmatism does not want to wear glasses. What is the best alternative for her?
Scleral Expansion Bands are used in the management of:
Which keratometry reading is most accurate in post-LASIK eyes for IOL power calculation?
Practice by Chapter
Corneal Topography and Tomography
Practice Questions
Patient Selection for Refractive Surgery
Practice Questions
LASIK
Practice Questions
PRK and LASEK
Practice Questions
Small Incision Lenticule Extraction
Practice Questions
Phakic IOLs
Practice Questions
Refractive Lens Exchange
Practice Questions
Astigmatic Keratotomy
Practice Questions
Intrastromal Corneal Ring Segments
Practice Questions
Corneal Collagen Crosslinking
Practice Questions
Complications of Refractive Surgery
Practice Questions
Future Trends in Refractive Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
