LASIK — MCQs

Which laser is used in the management of posterior capsule opacification (PCO)?
Which of the following is not a relative contraindication for breast conservative surgery?
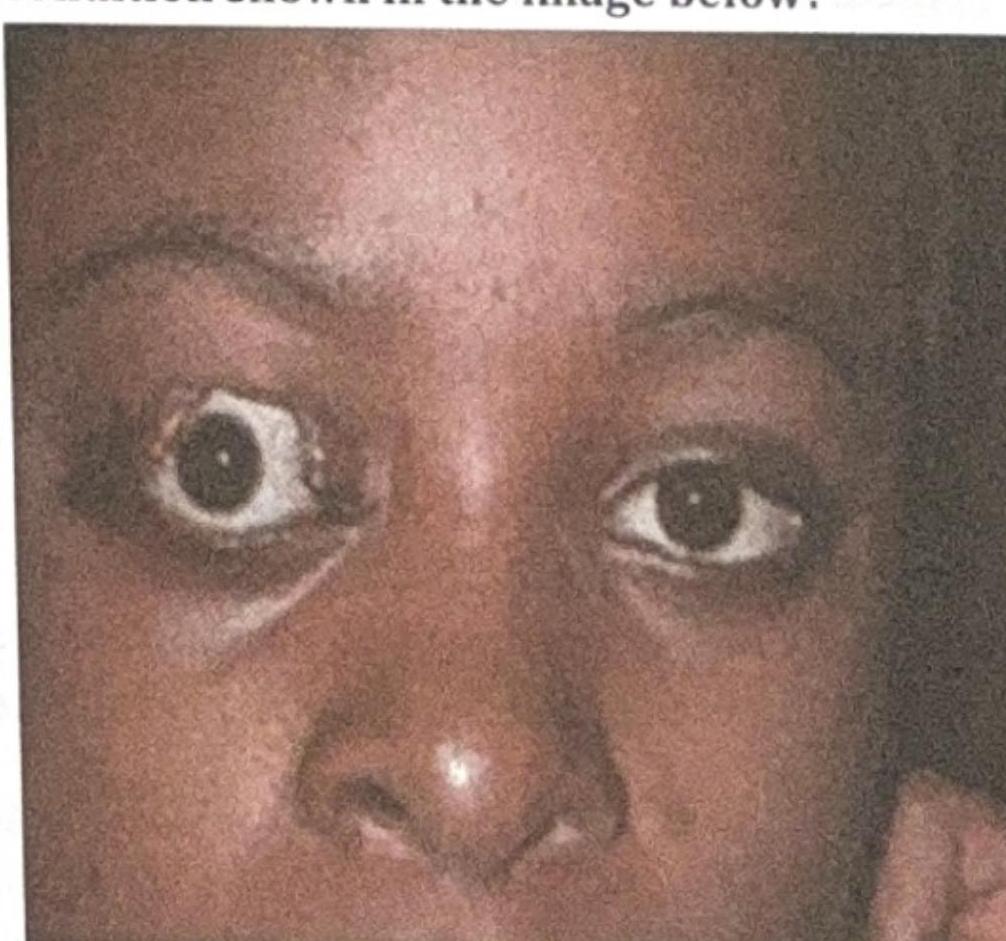
What is the most likely complication of the condition shown in the image below?
Which keratometry reading is most accurate in post-LASIK eyes for IOL power calculation?
Laser used in LASIK is:
The laser procedure, most often used for treating iris neovascularization is
Maximum correction of myopia can be done by?
What does a visual acuity test primarily assess?
Which of the following is a contraindication to topical steroids?
Which of the following is used for the treatment of Myopia?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
