Pediatric Ophthalmology and Strabismus — MCQs

On this page
A patient presents with recent onset paralytic squint. Which of the following statements regarding paralytic squint is true?
Knudson's hypothesis is applied for which of the following conditions?
Amaurotic cat eye reflex is seen in which condition?
What is the preferred cycloplegic drug for a 1-year-old child?
Loss of heterozygosity is associated with which of the following conditions?
Duane syndrome involves dysfunction of which extraocular muscle?
Conjugate fixation reflex is established by the age of:
Extraretinal fibrovascular proliferation at the ridge between normal and avascular retina is characteristic of which grade of Retinopathy of Prematurity (ROP)?
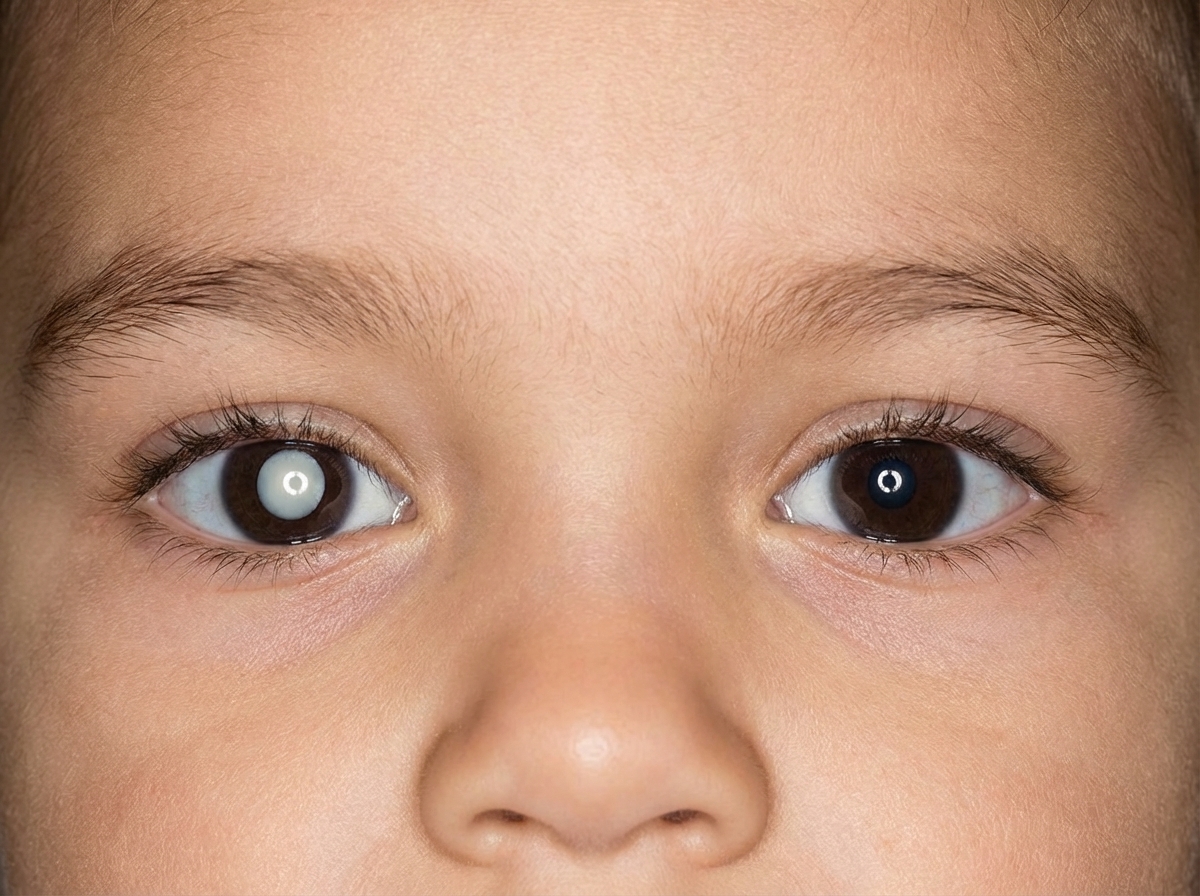
A 2-year-old child presented with a specific abnormality, and there is a history of a similar illness in his father. What is the most likely underlying condition responsible?
Weakness of both adduction and abduction is seen in which condition?
Practice by Chapter
Amblyopia
Practice Questions
Esotropia
Practice Questions
Exotropia
Practice Questions
Vertical Deviations
Practice Questions
Special Forms of Strabismus
Practice Questions
Nystagmus in Children
Practice Questions
Pediatric Cataract
Practice Questions
Retinopathy of Prematurity
Practice Questions
Pediatric Glaucoma
Practice Questions
Pediatric Neuro-ophthalmology
Practice Questions
Genetic Eye Diseases in Children
Practice Questions
Pediatric Ocular Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
