Pediatric Ophthalmology and Strabismus — MCQs

On this page
What condition presents with a white pupillary reflex?
In concomitant squint, which of the following is true regarding primary and secondary deviations?
A 3-year-old child presents with suspected squint. What is the drug of choice for refraction in this case?
Comment on the diagnosis?
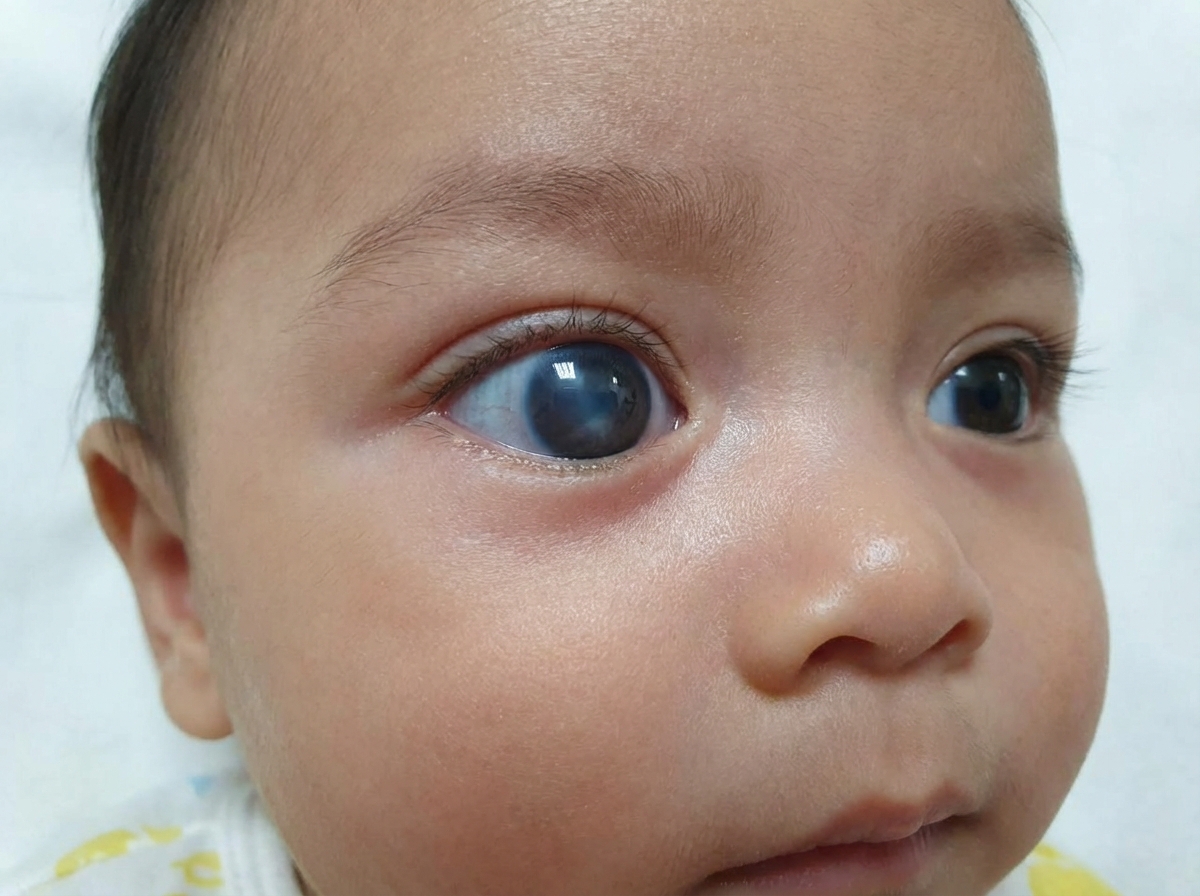
Which of the following drug classes is used in the management of accommodative esotropia?
Increased lactic dehydrogenase (LDH) in aqueous humor suggests which diagnosis?
Which childhood malignancy commonly presents with proptosis?
The Hirschberg test measures which of the following conditions?
Which pair of extraocular muscles is known as the 'yolk muscle pair'?
Blindness in a child is most commonly due to which of the following conditions?
Practice by Chapter
Amblyopia
Practice Questions
Esotropia
Practice Questions
Exotropia
Practice Questions
Vertical Deviations
Practice Questions
Special Forms of Strabismus
Practice Questions
Nystagmus in Children
Practice Questions
Pediatric Cataract
Practice Questions
Retinopathy of Prematurity
Practice Questions
Pediatric Glaucoma
Practice Questions
Pediatric Neuro-ophthalmology
Practice Questions
Genetic Eye Diseases in Children
Practice Questions
Pediatric Ocular Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
