Pediatric Ophthalmology and Strabismus — MCQs

On this page
Which of the following is NOT recommended for gonococcal eye prophylaxis?
What is the most common type of amblyopia?
Phoria is a type of
A 3-year-old male presents with sudden onset of visual loss in the left eye. Ophthalmological examination reveals strabismus and a white pupillary reflex. Fundus findings are as shown below. What is your diagnosis?
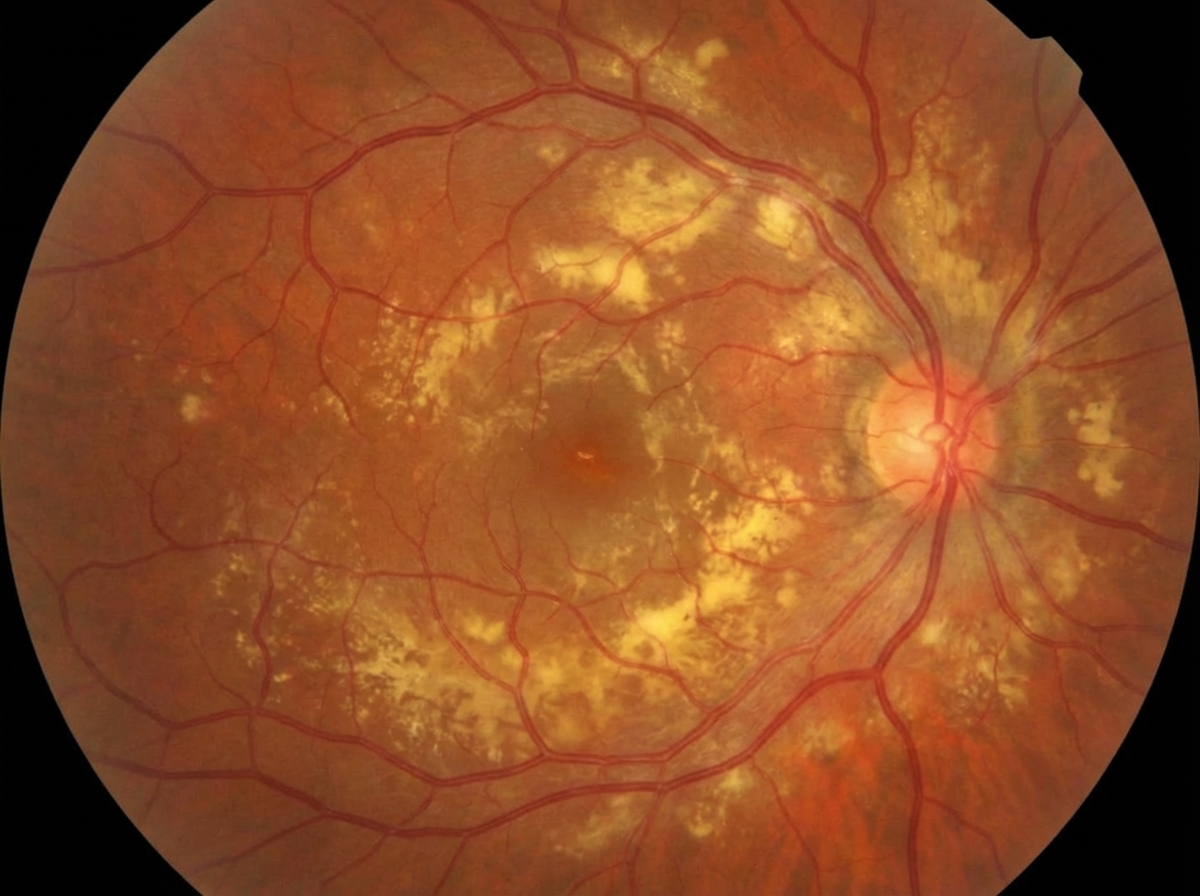
Regarding retinoblastoma, all of the following are true, EXCEPT?
Which of the following is associated with Retinoblastoma?
A patient with Coats' disease presenting with leukocoria needs to be differentiated from which of the following conditions?
What is the most common cause of epiphora in a newborn?
Which two muscles are primarily responsible for the elevation of the eye?
All of the following are true regarding paralytic squint, except:
Practice by Chapter
Amblyopia
Practice Questions
Esotropia
Practice Questions
Exotropia
Practice Questions
Vertical Deviations
Practice Questions
Special Forms of Strabismus
Practice Questions
Nystagmus in Children
Practice Questions
Pediatric Cataract
Practice Questions
Retinopathy of Prematurity
Practice Questions
Pediatric Glaucoma
Practice Questions
Pediatric Neuro-ophthalmology
Practice Questions
Genetic Eye Diseases in Children
Practice Questions
Pediatric Ocular Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
