Optics and Refraction — MCQs

On this page
Which type of lens is used to correct astigmatism?
A patient is diagnosed with simple myopia with regular astigmatism. Which of the following glasses should be prescribed?
The Rosenbaum chart is used to test for visual acuity at a distance of?
Presbyopia is due to which of the following?
Which of the following does not affect the refraction of the eye?
Pseudopapilitis is seen in which of the following conditions?
What is the maximum refractive error that can be neutralized by a pinhole?
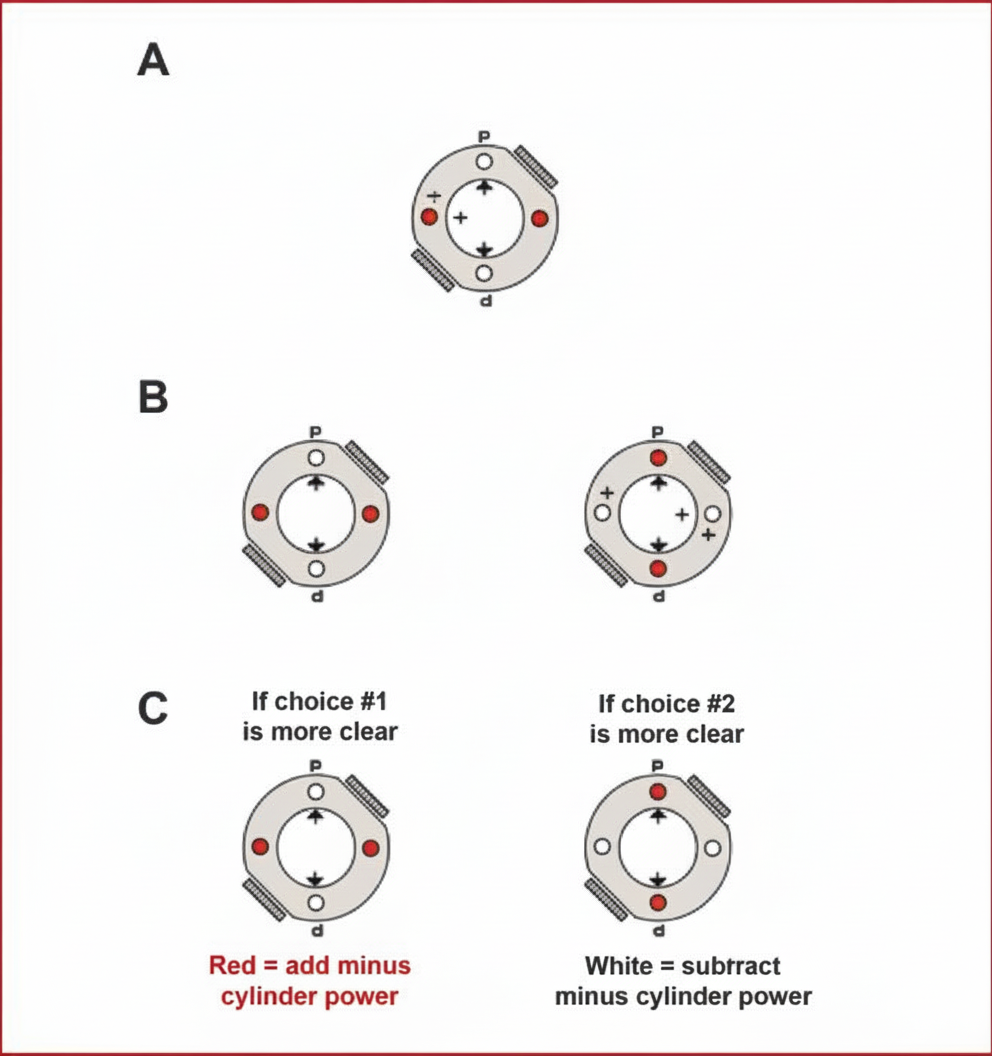
The optical procedure being done is used for:
When water enters the eyes, blurring of vision is due to which of the following?
What is the normal value of the Arden index?
Practice by Chapter
Physical Optics
Practice Questions
Geometric Optics
Practice Questions
Optical System of Eye
Practice Questions
Visual Acuity and Contrast Sensitivity
Practice Questions
Refractive Errors
Practice Questions
Accommodation and Presbyopia
Practice Questions
Optical Instruments
Practice Questions
Lenses and Prisms
Practice Questions
Retinoscopy
Practice Questions
Subjective Refraction
Practice Questions
Contact Lens Optics
Practice Questions
Wavefront Technology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
