Optics and Refraction — MCQs

On this page
Refraction of the eye is affected by all of the following except:
Which of the following has the maximum field of vision?
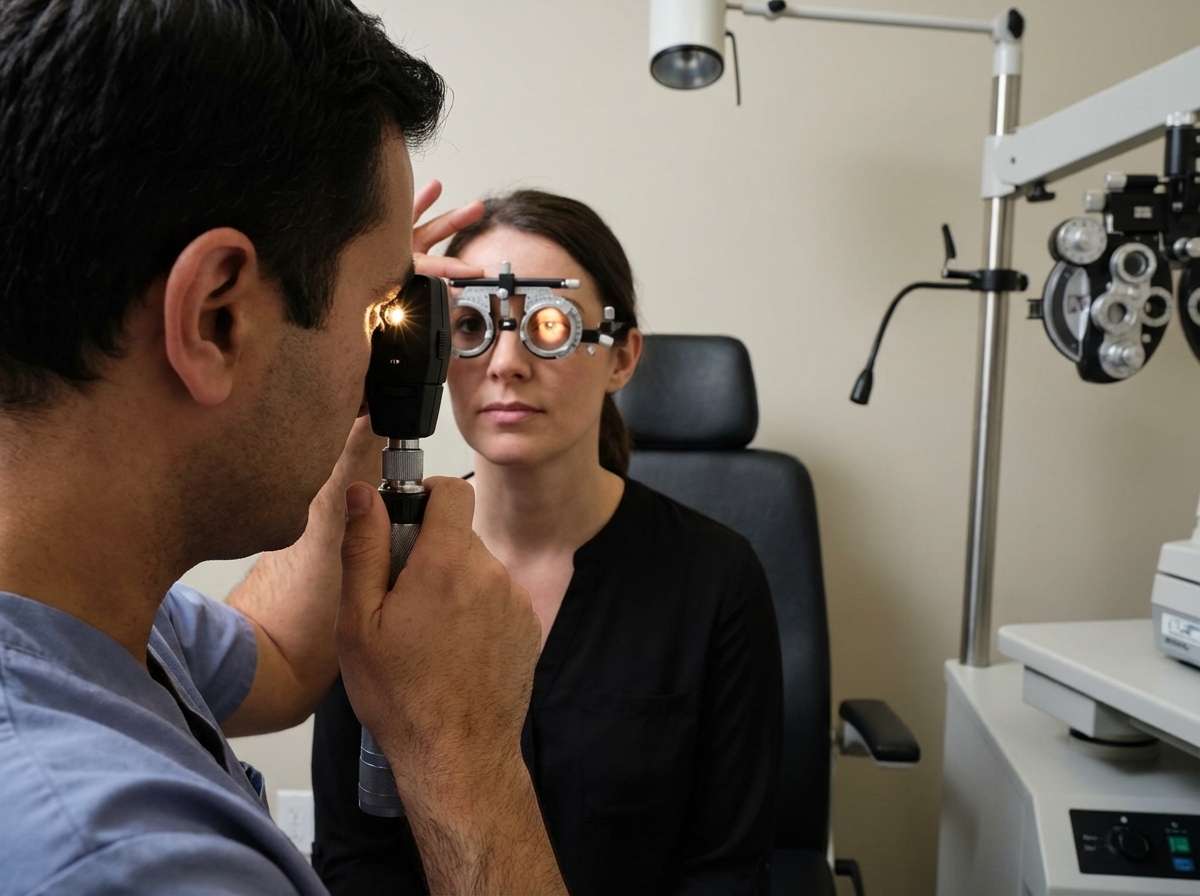
Name the procedure shown in the image?
The near point of the eye varies with which of the following factors?
What is the normal power of a reduced eye in diopters?
Which component of the eye has the maximum refractive index?
Soft contact lenses are primarily made of which material?
Presbyopia occurs as a result of which of the following changes?
Visual acuity test is a test of:
Snellen's chart is based on which visual function?
Practice by Chapter
Physical Optics
Practice Questions
Geometric Optics
Practice Questions
Optical System of Eye
Practice Questions
Visual Acuity and Contrast Sensitivity
Practice Questions
Refractive Errors
Practice Questions
Accommodation and Presbyopia
Practice Questions
Optical Instruments
Practice Questions
Lenses and Prisms
Practice Questions
Retinoscopy
Practice Questions
Subjective Refraction
Practice Questions
Contact Lens Optics
Practice Questions
Wavefront Technology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
