Optics and Refraction — MCQs

On this page
A person came to the eye OPD for a routine eye check. On the Snellen's chart, they were found to read 6/6 in both eyes. What is the largest approximate distance at which they would be able to read the first topmost letter?
What is the most important refractive surface of the eye?
Landolt's broken ring test is used for testing:
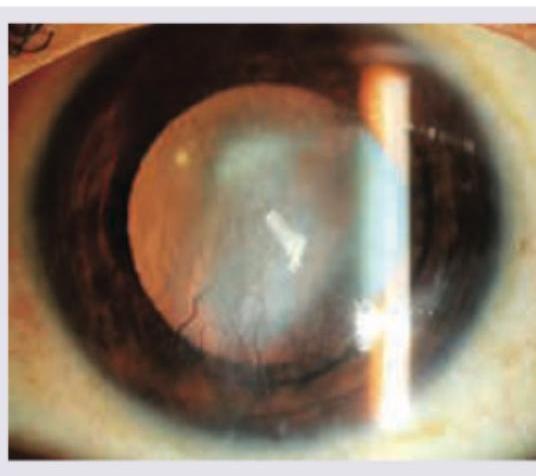
A 59-year-old male presents with dimness of near vision. On examination, the media was clear in both eyes. What is the next appropriate step?
In the given condition, what is the cause of defective vision?
True stereopsis is perceived due to which of the following?
If the length of the eyeball increases by 1 mm, what is the net effect on refractive error?
LASIK is used in which of the following refractive errors?
Astigmatism is due to which of the following?
What is true about the amplitude of accommodation?
Practice by Chapter
Physical Optics
Practice Questions
Geometric Optics
Practice Questions
Optical System of Eye
Practice Questions
Visual Acuity and Contrast Sensitivity
Practice Questions
Refractive Errors
Practice Questions
Accommodation and Presbyopia
Practice Questions
Optical Instruments
Practice Questions
Lenses and Prisms
Practice Questions
Retinoscopy
Practice Questions
Subjective Refraction
Practice Questions
Contact Lens Optics
Practice Questions
Wavefront Technology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
