Optics and Refraction — MCQs

On this page
What is the refractive condition of the eye?
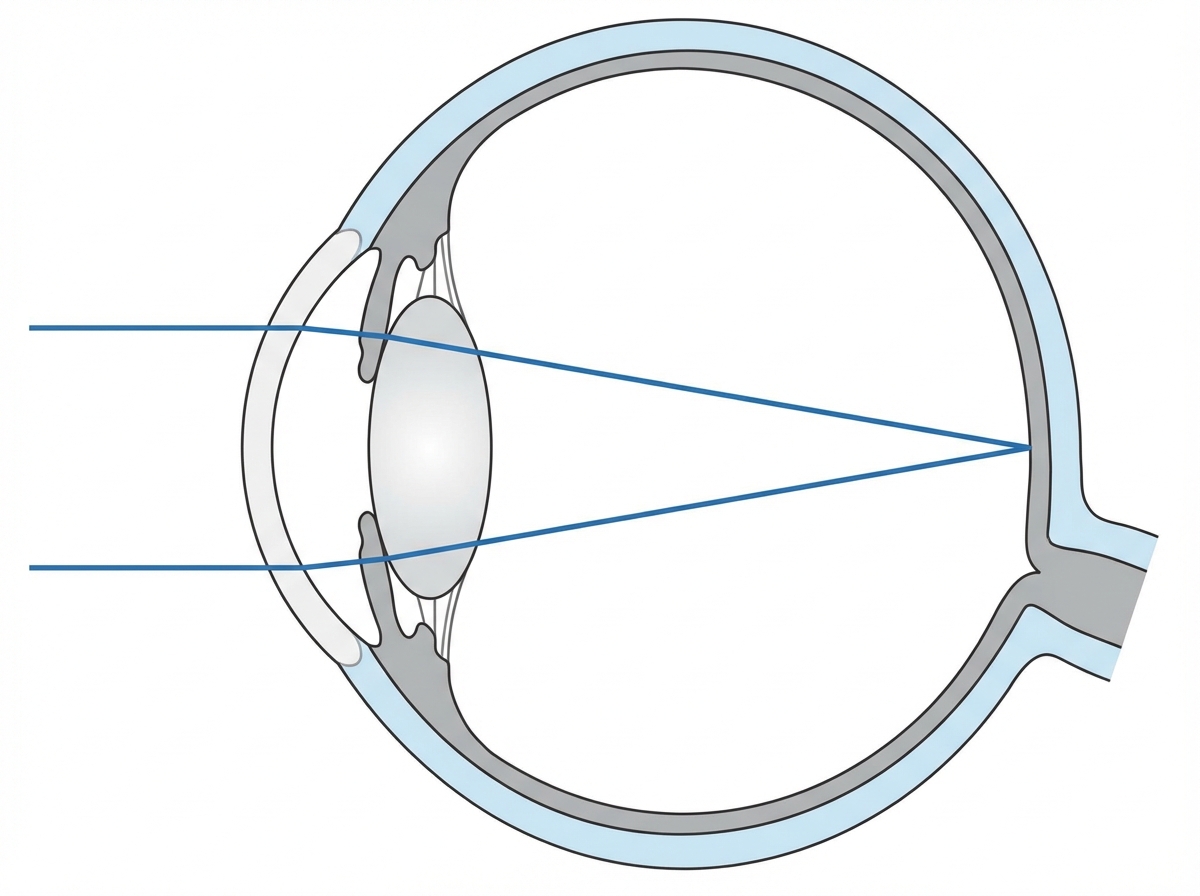
In myopia, what occurs?
What is the most accepted method for treating myopia with a refractive error of 2 diopters?
Which type of cataract is commonly induced by prolonged steroid use?
In indirect ophthalmoscopy, what refractive state is the examining eye intentionally made to achieve?
Practice by Chapter
Physical Optics
Practice Questions
Geometric Optics
Practice Questions
Optical System of Eye
Practice Questions
Visual Acuity and Contrast Sensitivity
Practice Questions
Refractive Errors
Practice Questions
Accommodation and Presbyopia
Practice Questions
Optical Instruments
Practice Questions
Lenses and Prisms
Practice Questions
Retinoscopy
Practice Questions
Subjective Refraction
Practice Questions
Contact Lens Optics
Practice Questions
Wavefront Technology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
