Ophthalmic Surgery — MCQs

On this page
What is phacoanaphylactic uveitis?
Plication of inferior lid retractors is indicated in which of the following conditions?
A patient with fixed dilated pupil, iris atrophy, and secondary glaucoma after penetrating keratoplasty is suggestive of which syndrome?
What is the percentage of endothelial cell loss during Descemet's stripping automated endothelial keratoplasty?
Which of the following is NOT true regarding suprachoroidal hemorrhage?
Following cataract surgery, a patient comes with complaints of decreased visual acuity. On examination, posterior capsular opacification is seen. What type of laser can be used to treat this condition?
Following a fungal corneal ulcer, a farmer underwent corneal transplant surgery. What is the preservative used for storing the donor corneal graft and the suture material used in the procedure?
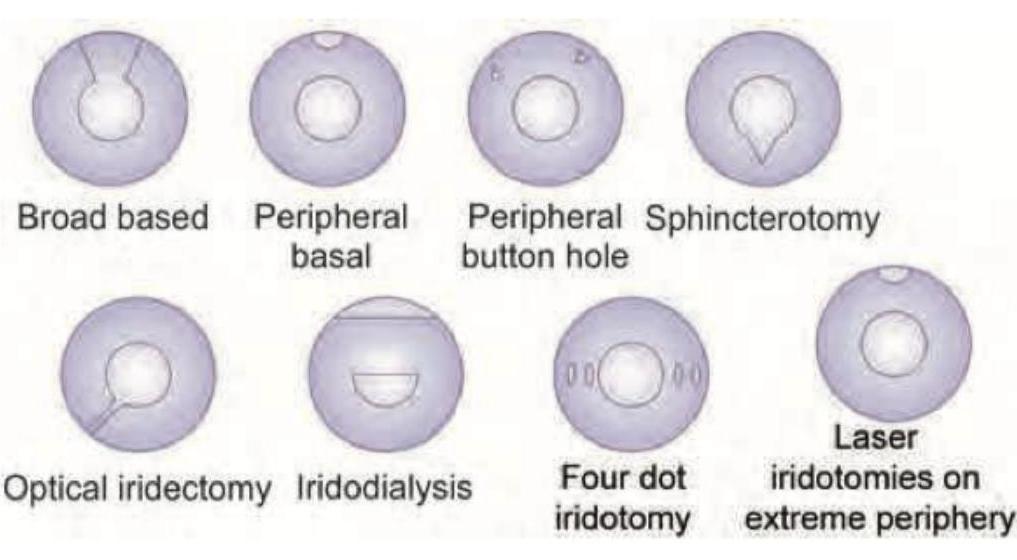
The type of iridectomy shown in the image is:
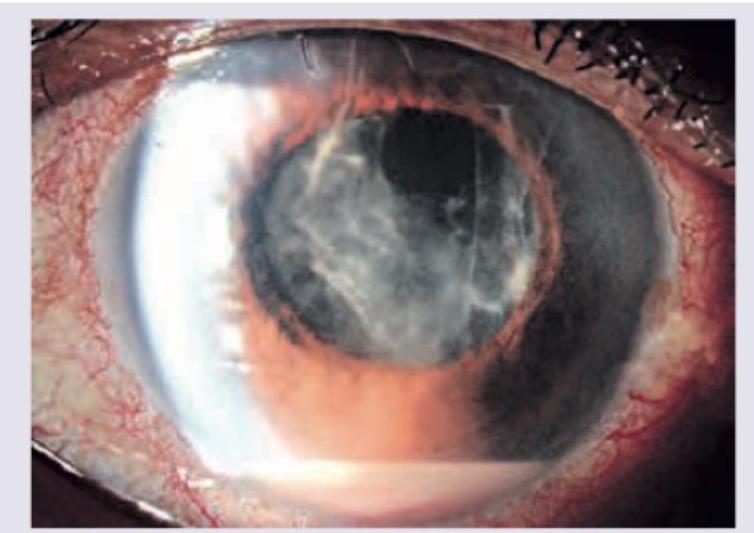
A patient on day 2 after cataract surgery has developed the following findings which are diagnostic of:
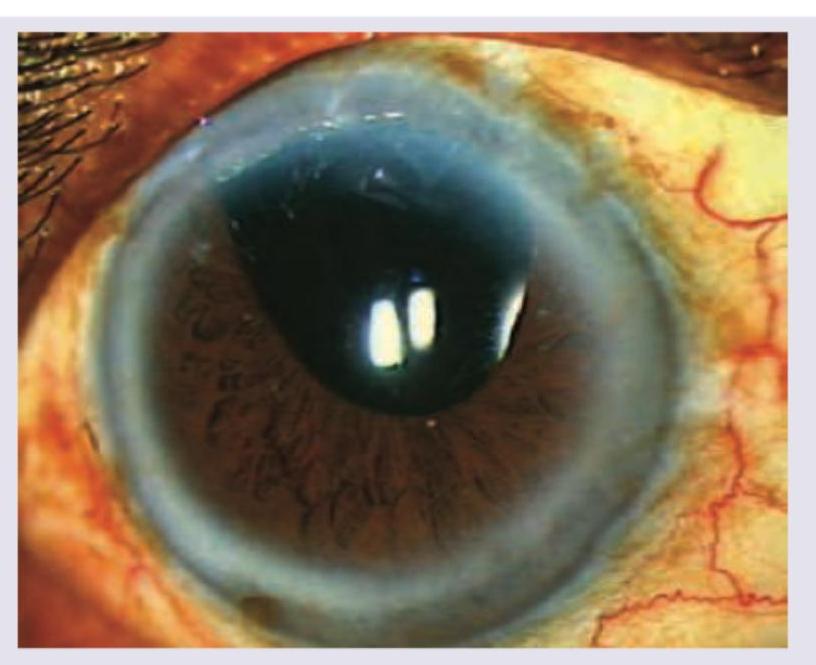
The patient underwent complete iridectomy in aphakia. Comment on the diagnosis:
Practice by Chapter
Surgical Anatomy of Eye
Practice Questions
Asepsis and Sterilization in Eye Surgery
Practice Questions
Anesthesia in Ophthalmic Surgery
Practice Questions
Cataract Surgery Techniques
Practice Questions
Corneal Surgeries
Practice Questions
Glaucoma Surgeries
Practice Questions
Oculoplastic Surgeries
Practice Questions
Vitreoretinal Surgeries
Practice Questions
Strabismus Surgery
Practice Questions
Refractive Surgery
Practice Questions
Ocular Oncology Surgeries
Practice Questions
Management of Surgical Complications
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
