Ophthalmic Surgery — MCQs

On this page
Dacryocystorhinostomy is contraindicated in all EXCEPT?
What is the treatment for nasolacrimal duct obstruction?
Recovery in cataract surgery is fastest with which of the following procedures?
Inferior oblique muscle is most weakened by which surgical procedure?
What technique of cataract extraction is used in the care of a subluxated lens?
Which method is used to visualize the periphery of the retina?
Inverse hypopyon is seen in which of the following conditions?
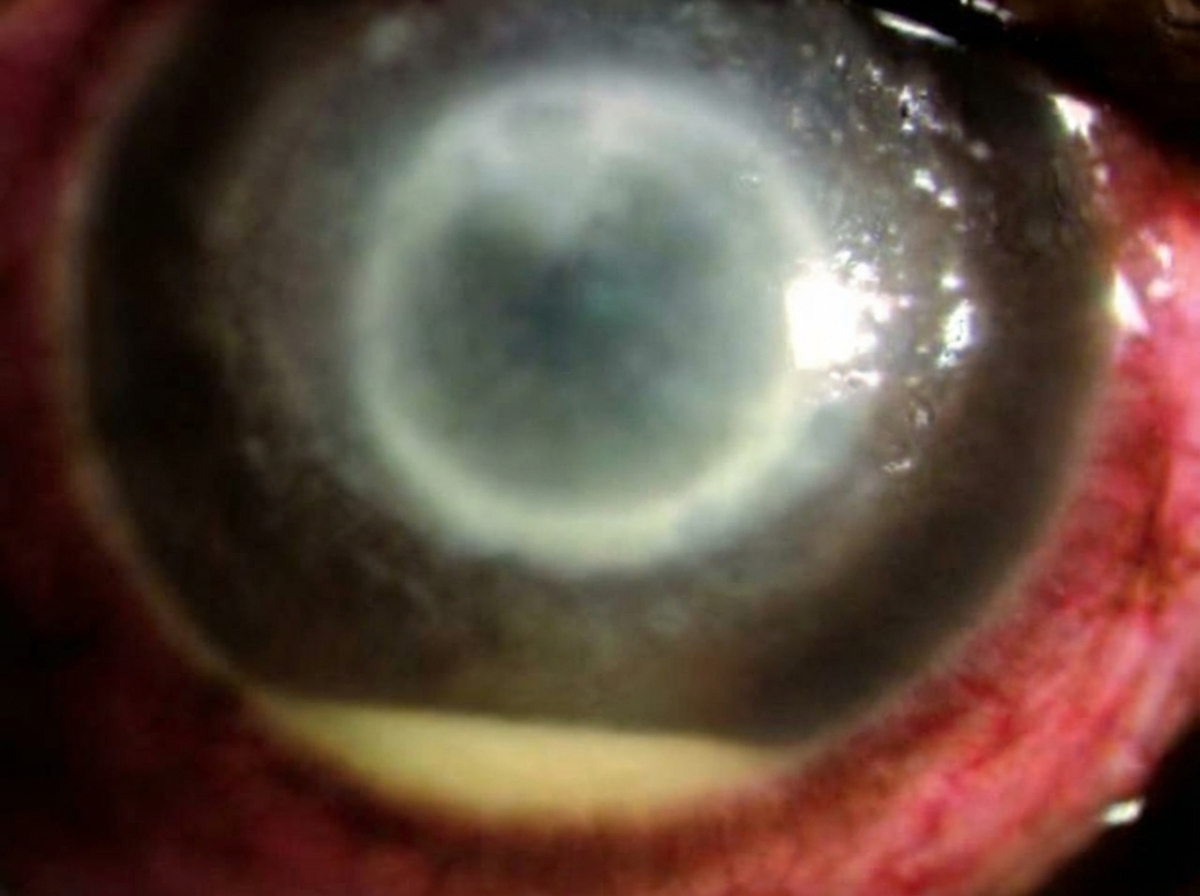
A patient developed pain and severe vision loss 2 days after cataract surgery. On examination, a particular finding was noted. Which of the following statements about the given condition is INCORRECT?
Which of the following is not true regarding the treatment for chalazion?
What is the treatment of choice for acute dacryocystitis?
Practice by Chapter
Surgical Anatomy of Eye
Practice Questions
Asepsis and Sterilization in Eye Surgery
Practice Questions
Anesthesia in Ophthalmic Surgery
Practice Questions
Cataract Surgery Techniques
Practice Questions
Corneal Surgeries
Practice Questions
Glaucoma Surgeries
Practice Questions
Oculoplastic Surgeries
Practice Questions
Vitreoretinal Surgeries
Practice Questions
Strabismus Surgery
Practice Questions
Refractive Surgery
Practice Questions
Ocular Oncology Surgeries
Practice Questions
Management of Surgical Complications
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
