Ophthalmic Surgery — MCQs

On this page
The image shows an eye following a surgical procedure. What type of iridectomy is depicted?
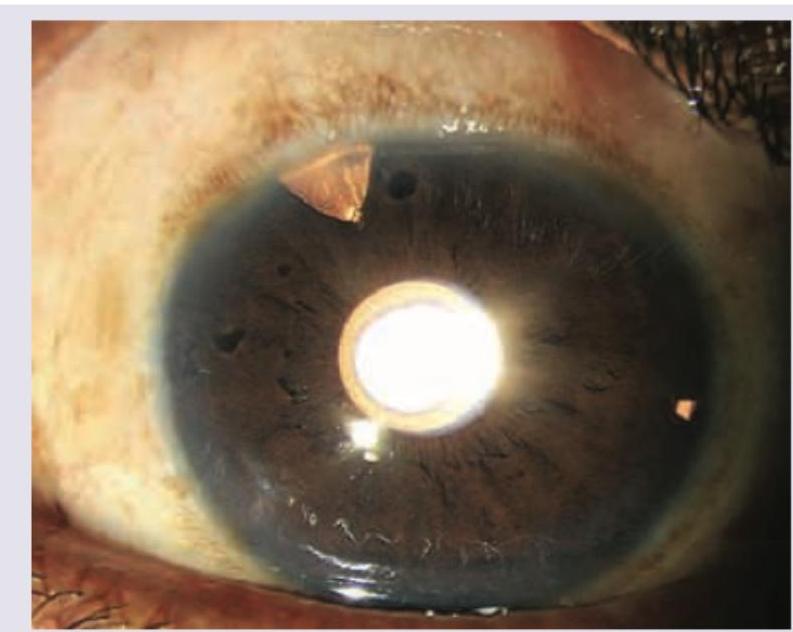
What does the given image show?
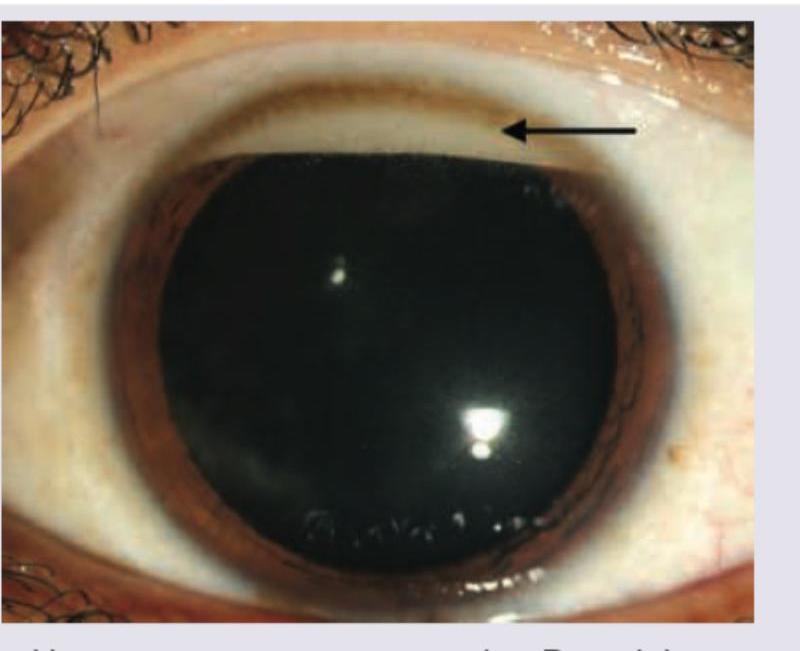
Patient with eye surgery done 2 days ago presents with pain and dimness of vision. Which of the following is not useful for management?
All the following statements regarding the image given are true except: (Recent Neet Pattem 2016-17)
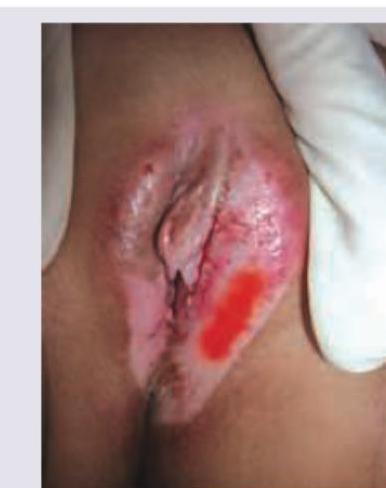
Identify the surgical step shown in the image given below
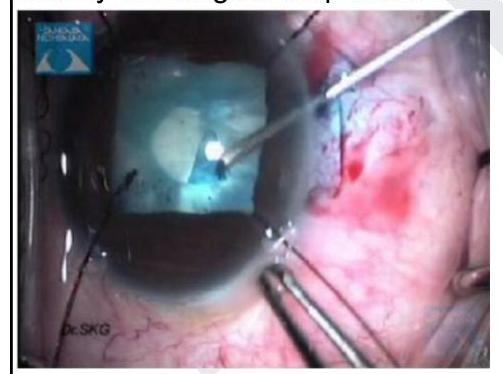
Evisceration is removal of which layer of eyeball?
For laser iridotomy which laser is used?
Site of bleeding after cataract surgery is:
Which laser is used for posterior capsular opacification (PCO)?
Gold standard procedure to reduce recurrence of pterygium after surgical excision is
Practice by Chapter
Surgical Anatomy of Eye
Practice Questions
Asepsis and Sterilization in Eye Surgery
Practice Questions
Anesthesia in Ophthalmic Surgery
Practice Questions
Cataract Surgery Techniques
Practice Questions
Corneal Surgeries
Practice Questions
Glaucoma Surgeries
Practice Questions
Oculoplastic Surgeries
Practice Questions
Vitreoretinal Surgeries
Practice Questions
Strabismus Surgery
Practice Questions
Refractive Surgery
Practice Questions
Ocular Oncology Surgeries
Practice Questions
Management of Surgical Complications
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
