Ophthalmic Pharmacology — MCQs

On this page
Pilocarpine is an:
Which of the following is a recently approved drug for the treatment of neovascular age-related macular degeneration?
What concentration of alcaftadine was used in its trial?
A 29-year-old female diagnosed with AIDS presents with progressive blurring of vision in her right eye. Funduscopic examination reveals a small, white, opaque lesion on the retina of her right eye. What is the most appropriate therapy for this patient?
In a patient predisposed to glaucoma, which drug is contraindicated?
A patient with glaucoma develops blepharoconjunctivitis after instilling an anti-glaucoma medication. Which of the following drugs is most likely responsible for this side effect?
Which drug is used during a trabeculectomy procedure?
What is the drug of choice for the treatment of intermediate uveitis?
Which of the following topical local anesthetics is commonly used in cataract surgery?
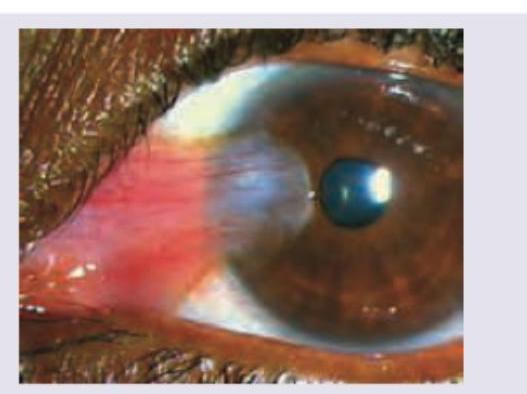
A patient has the following presentation. After administration of an intravenous drug to the patient, in 6 minutes his symptoms have resolved. The diagnosis of the patient is:
Practice by Chapter
Ocular Pharmacokinetics
Practice Questions
Anti-infective Agents
Practice Questions
Anti-inflammatory Drugs
Practice Questions
Antiglaucoma Medications
Practice Questions
Mydriatics and Cycloplegics
Practice Questions
Ocular Lubricants
Practice Questions
Anti-VEGF Agents
Practice Questions
Ocular Diagnostic Agents
Practice Questions
Anesthetics in Ophthalmology
Practice Questions
Preservatives and Their Effects
Practice Questions
Ocular Toxicology
Practice Questions
Novel Drug Delivery Systems
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
