Ocular Trauma — MCQs

On this page
Which of the following is NOT a sign of blunt ocular trauma?
Which of the following conditions does NOT occur due to blunt trauma of the eye?
Clinically, in the non-injured eye, sympathetic ophthalmitis may manifest as?
Which of the following is seen in iridodialysis?
All are clinical features of chalcosis except?
What is the most serious complication seen in the other eye after a traumatic injury to one eye?
A patient has a history of a flying metallic foreign body injury to the eye. On examination, there is evidence of intraocular metallic foreign body with progressive visual deterioration. Which of the following substances is most likely causing the toxic deposition in ocular tissues?
A patient sustained blunt trauma to the eye 6 months ago and now presents with blurring of vision. What is the most likely condition?
A patient presents to you with pain and redness in the right eye following an injury during welding. On examination, the following is observed. Which of the following is the appropriate next step in managing this patient? 
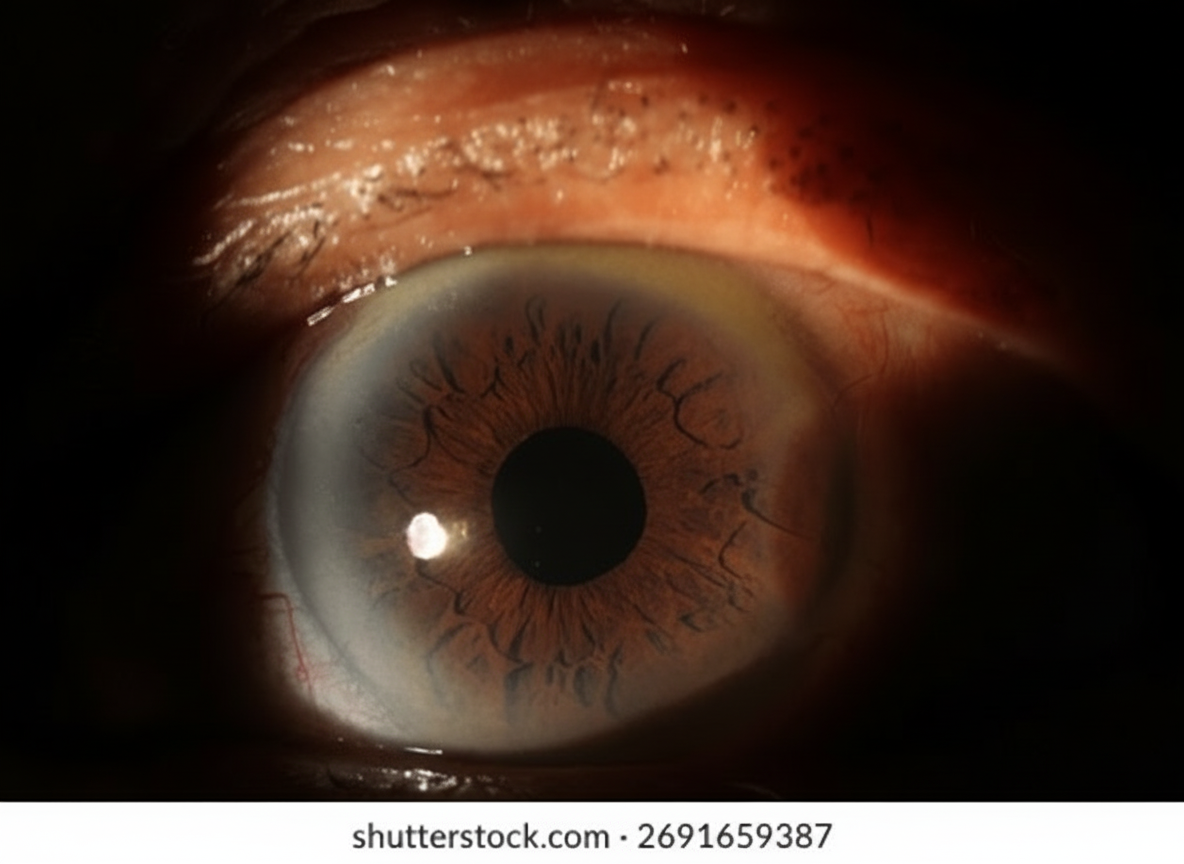
The following appearance of eye is seen in:
Practice by Chapter
Classification of Ocular Trauma
Practice Questions
Blunt Trauma
Practice Questions
Penetrating and Perforating Injuries
Practice Questions
Intraocular Foreign Bodies
Practice Questions
Chemical Injuries
Practice Questions
Thermal and Radiation Injuries
Practice Questions
Orbital Trauma
Practice Questions
Traumatic Optic Neuropathy
Practice Questions
Ocular Manifestations of Child Abuse
Practice Questions
Sports-Related Eye Injuries
Practice Questions
Ocular Trauma Management Principles
Practice Questions
Rehabilitation After Ocular Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
