Ocular Manifestations of Systemic Disorders — MCQs

On this page
Epidemic dropsy is characterised by all EXCEPT:
Which of the following is the most common cause of anterior uveitis?
What is the most common benign tumor of the eyelids?
What is the cause of acute vision loss in a patient with alcoholic pancreatitis?
Heterochromia iridis is a feature of:
Which syndrome is characterized by the following ocular finding?
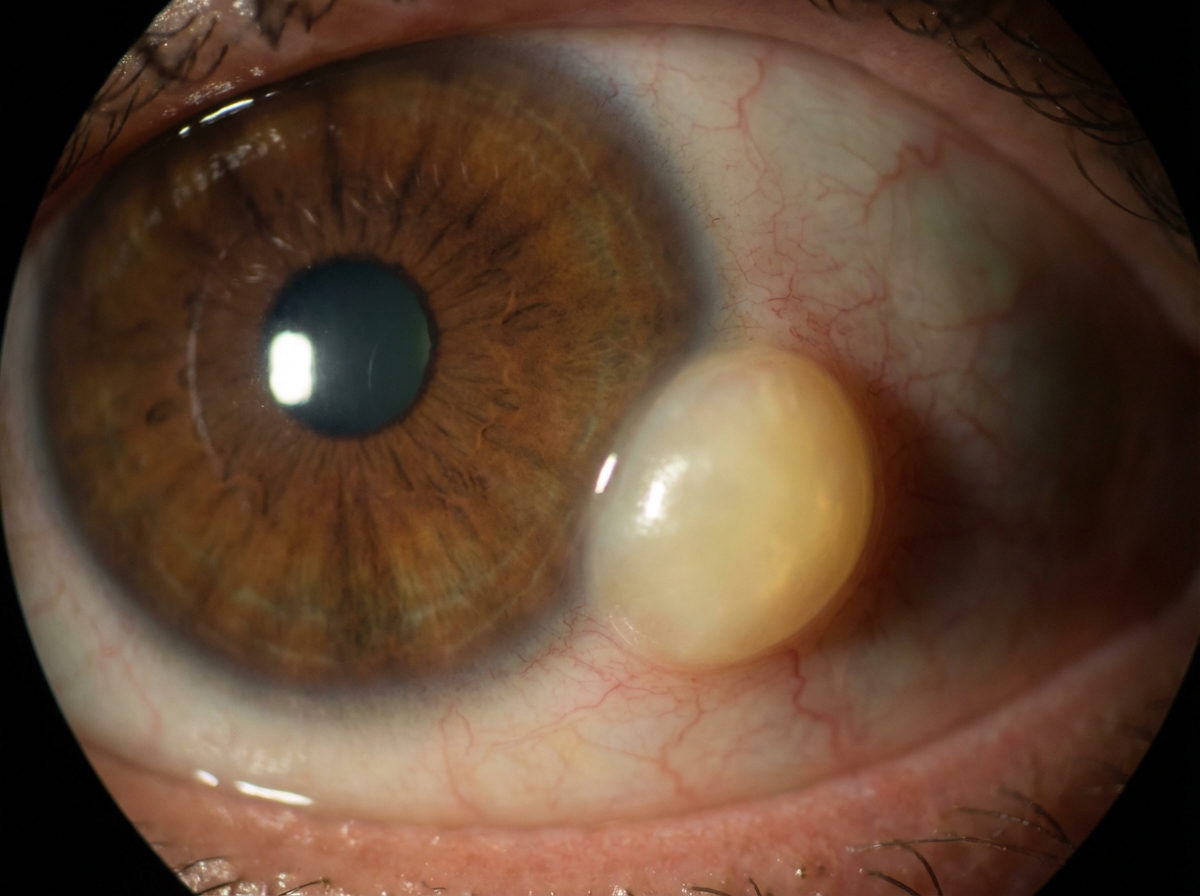
All are causes of chronic granulomatous uveitis EXCEPT:
Which of the following statements is not true regarding uveitis?
Which of the following can cause lid retraction?
Vascular invasion is commonly seen in which of the following ocular tumors?
Practice by Chapter
Diabetes Mellitus
Practice Questions
Hypertension
Practice Questions
Autoimmune Disorders
Practice Questions
Thyroid Disease
Practice Questions
HIV and AIDS
Practice Questions
Hematological Disorders
Practice Questions
Neurological Disorders
Practice Questions
Dermatological Conditions
Practice Questions
Pregnancy-Related Eye Changes
Practice Questions
Metabolic Disorders
Practice Questions
Ocular Toxicity of Systemic Medications
Practice Questions
Infectious Systemic Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
