Ocular Manifestations of Systemic Disorders — MCQs

On this page
A 30-year-old patient with a history of recurrent headache presents for fundus evaluation. Funduscopic examination reveals generalized arterial attenuation, multiple cotton wool spots, and flame-shaped hemorrhages in both eyes. What is the most likely cause?
What is the first symptom of vitamin A deficiency?
Which of the following statements regarding chalazion is true?
A 37-year-old woman presented with symptoms consistent with allergic conjunctivitis. What is the diagnosis for this incidental finding?
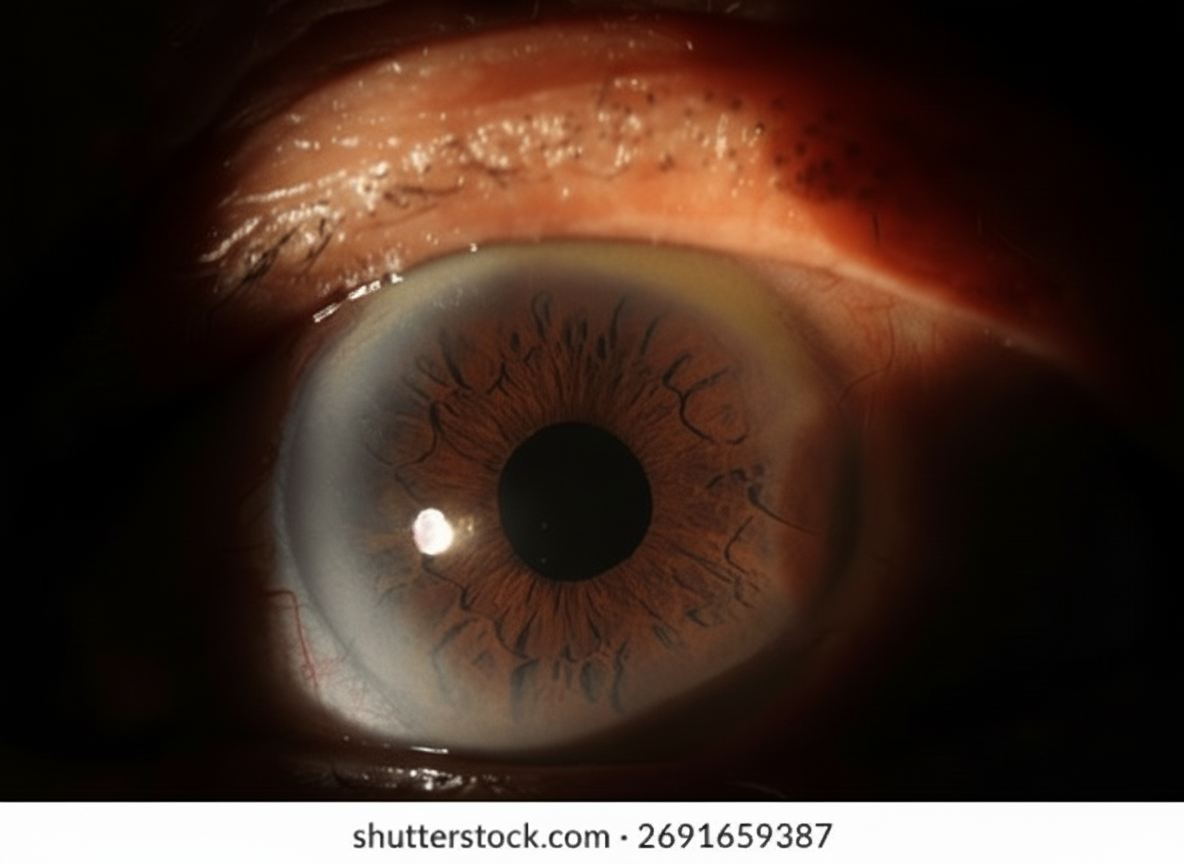
Heerfordt's syndrome is characterized by all of the following EXCEPT:
In Von Hippel-Lindau Syndrome, retinal vascular tumors are often associated with intracranial hemangioblastoma. Which one of the following regions is associated with such vascular abnormalities in this syndrome?
What is the causative agent for Oculoglandular syndrome of Parinaud?
What is a common ocular consequence of a sudden increase in blood sugar in a diabetic patient?
Chronic, sterile inflammation of the meibomian gland is seen in which of the following conditions?
What is true about cavernous sinus thrombosis?
Practice by Chapter
Diabetes Mellitus
Practice Questions
Hypertension
Practice Questions
Autoimmune Disorders
Practice Questions
Thyroid Disease
Practice Questions
HIV and AIDS
Practice Questions
Hematological Disorders
Practice Questions
Neurological Disorders
Practice Questions
Dermatological Conditions
Practice Questions
Pregnancy-Related Eye Changes
Practice Questions
Metabolic Disorders
Practice Questions
Ocular Toxicity of Systemic Medications
Practice Questions
Infectious Systemic Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
