Ocular Manifestations of Systemic Disorders — MCQs

On this page
Vision loss in HIV is commonly due to infection with?
What is the best management for an immunocompromised patient with the following fundus findings?
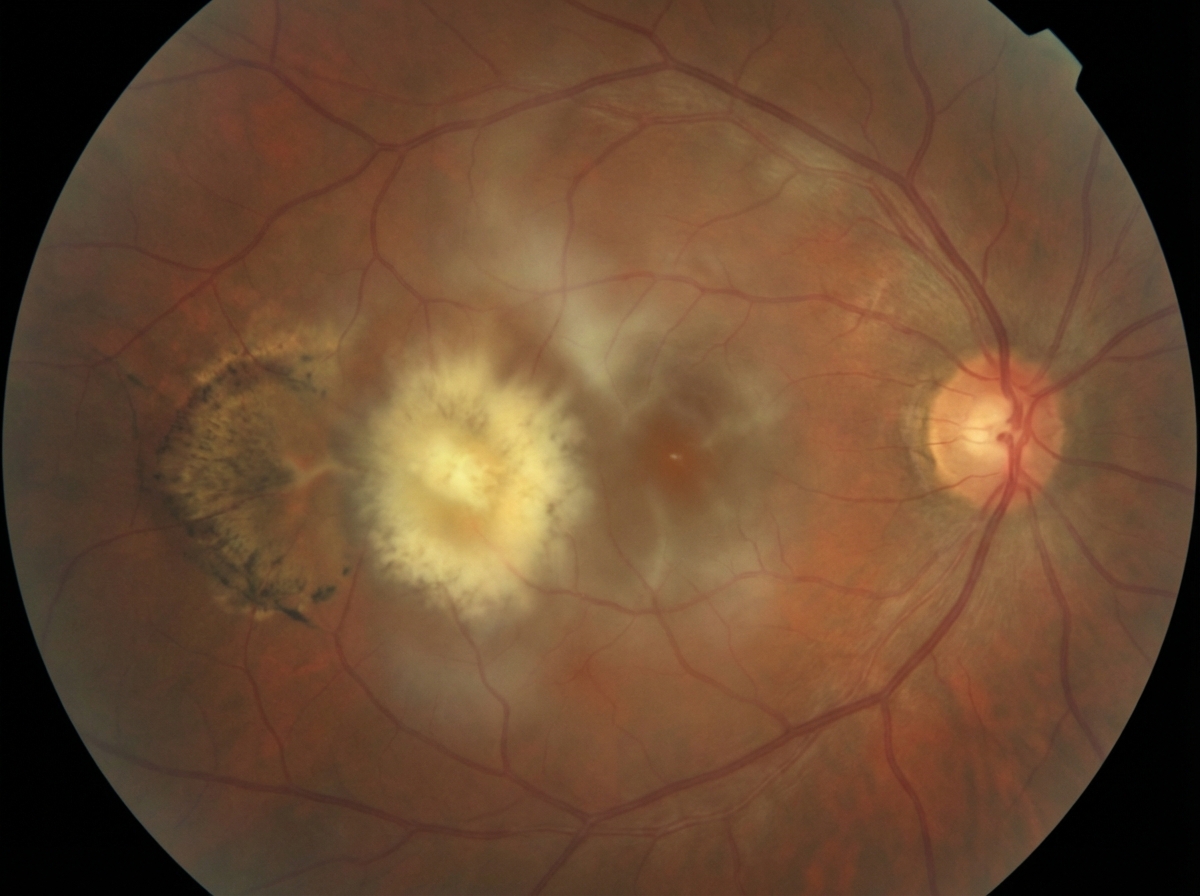
Systemic corticosteroids in herpes zoster ophthalmicus are indicated when associated with which of the following conditions?
Red keratin precipitates are seen in which of the following conditions?
The use of highly active anti-retroviral therapy (HAART) is associated with the development of:
Which one of the following is not an ocular emergency?
What is seen in the fundus of a patient with disseminated tuberculosis?
Which condition is characterized by the "Candle wax dripping sign"?
All the following are causes of bluish sclerae in young children, EXCEPT:
A 12-year-old girl complains of headaches and blurred vision. She has a history of high blood pressure but is not currently taking medication. Her blood pressure is 160/95 mm Hg and pulse is 95 per minute. Funduscopic examination reveals small retinal microaneurysms and cotton-like zones of retinal edema and necrosis. She is hospitalized for further evaluation. Renal arteriography shows segmental stenoses forming multiple ridges that project into the lumen. What is the most likely cause of secondary hypertension in this young patient?
Practice by Chapter
Diabetes Mellitus
Practice Questions
Hypertension
Practice Questions
Autoimmune Disorders
Practice Questions
Thyroid Disease
Practice Questions
HIV and AIDS
Practice Questions
Hematological Disorders
Practice Questions
Neurological Disorders
Practice Questions
Dermatological Conditions
Practice Questions
Pregnancy-Related Eye Changes
Practice Questions
Metabolic Disorders
Practice Questions
Ocular Toxicity of Systemic Medications
Practice Questions
Infectious Systemic Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
