Neuro-Ophthalmology — MCQs

On this page
A 40-year-old female presented with an excruciating headache, ptosis, downward and outward gaze of the eyeball, and a large pupil. She also complained of blurred and double vision. An magnetic resonance angiogram scan showed an aneurysm of the circle of Willis. Which artery gives rise to the offending aneurysm?
Which of the following drugs does NOT cause retinal changes?
Internuclear ophthalmoplegia is caused due to a lesion in which of the following?
Papilledema is caused by tumors arising from all the following structures except:
Anisocoria in dim light is maximally seen in which condition?
All of the following findings are associated with optic neuritis except?
A 23-year-old woman complains of progressive loss of vision and papilledema. Investigations show normal findings on CT scan. A lumbar puncture shows marked elevation of pressure. What is the most likely diagnosis?
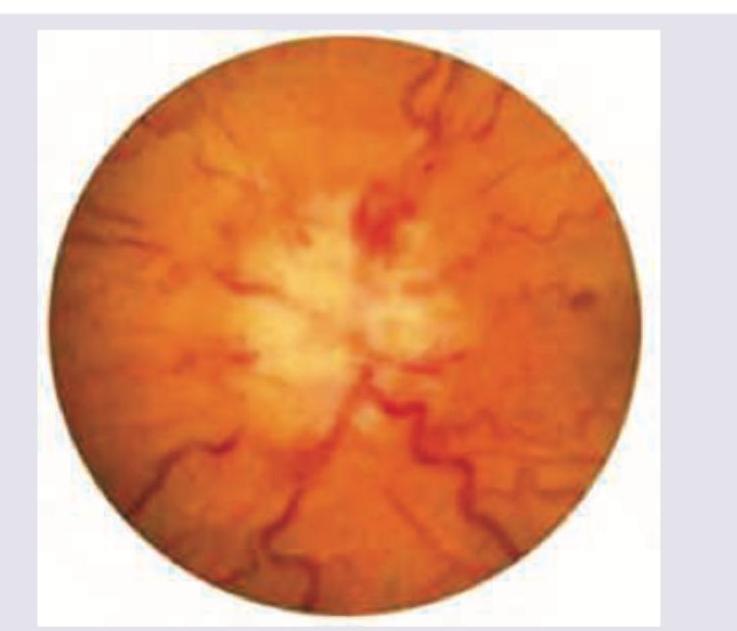
Diagnose the ocular pathology.
Opsoclonus is a feature of which of the following conditions?
Which of the following is NOT a feature of Horner syndrome?
Practice by Chapter
Anatomy of Visual Pathways
Practice Questions
Pupillary Disorders
Practice Questions
Optic Neuritis
Practice Questions
Ischemic Optic Neuropathies
Practice Questions
Other Optic Neuropathies
Practice Questions
Papilledema
Practice Questions
Cranial Nerve Palsies
Practice Questions
Nystagmus
Practice Questions
Visual Field Defects
Practice Questions
Neuro-ophthalmic Manifestations of Intracranial Lesions
Practice Questions
Functional Visual Disorders
Practice Questions
Migraine and the Eye
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
