Neuro-Ophthalmology — MCQs

On this page
A patient with pituitary adenoma compressing the optic chiasma now presents with loss of visual field. What visual field defect will be seen in the patient?
A patient presents with right-sided field defects in both eyes, but central vision remains unaffected. What is the most likely diagnosis?
Which of the following is NOT a feature of Horner's Syndrome?
Which of the following is the diagnosis based on the given eye movement abnormality image?
In optic neuritis, which is true?
What is the clinical condition shown in the image?

Which of the following lesions will develop after lesion in the area marked as $X$ ?
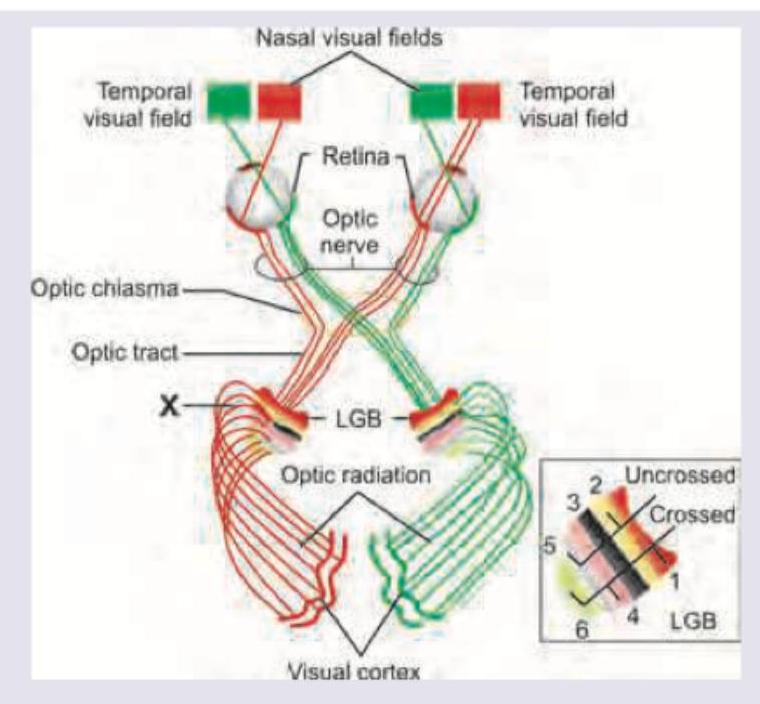
A child has been diagnosed with cavernous sinus meningioma. Which of these is correct?
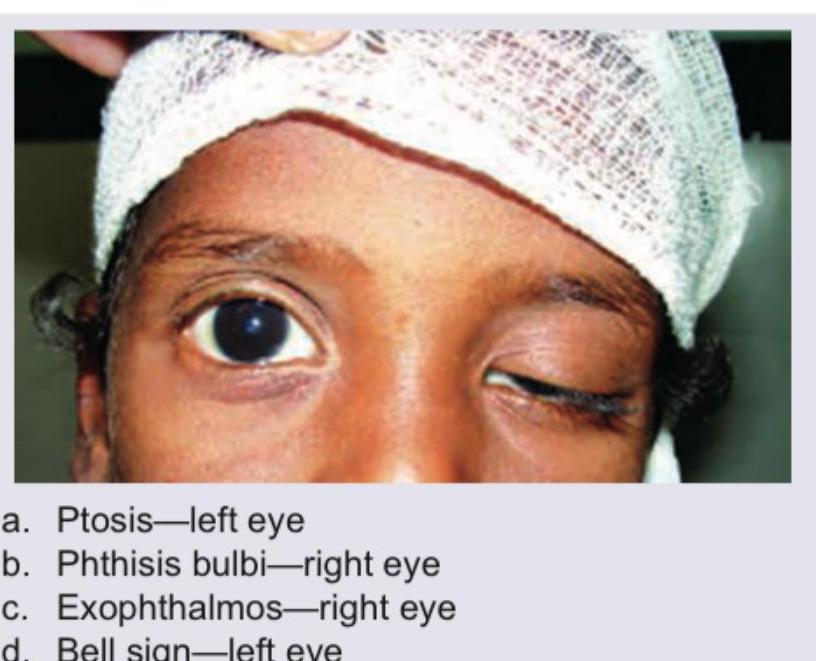
The following image shows:
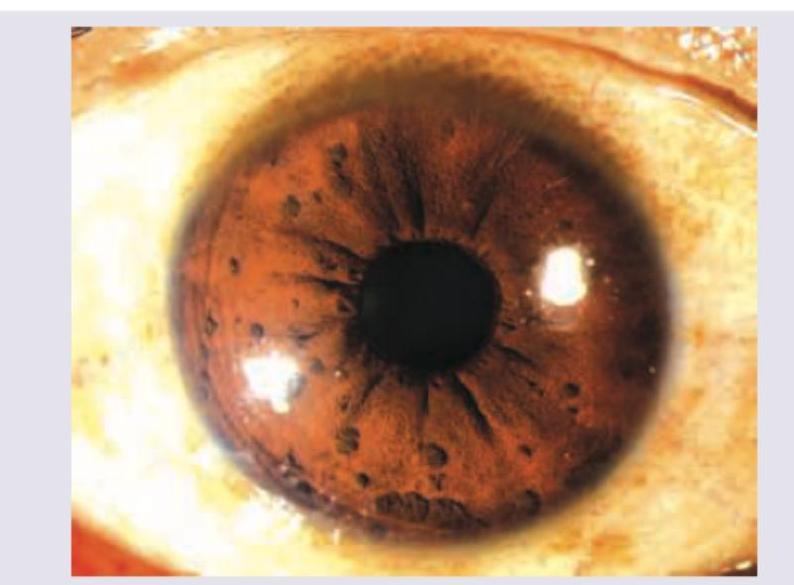
All are causes of the field defect shown below except:

Practice by Chapter
Anatomy of Visual Pathways
Practice Questions
Pupillary Disorders
Practice Questions
Optic Neuritis
Practice Questions
Ischemic Optic Neuropathies
Practice Questions
Other Optic Neuropathies
Practice Questions
Papilledema
Practice Questions
Cranial Nerve Palsies
Practice Questions
Nystagmus
Practice Questions
Visual Field Defects
Practice Questions
Neuro-ophthalmic Manifestations of Intracranial Lesions
Practice Questions
Functional Visual Disorders
Practice Questions
Migraine and the Eye
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
