Neuro-Ophthalmology — MCQs

On this page
Typical field defect observed in anterior ischemic optic neuropathy is?
Which of the following is NOT a characteristic of diabetic third nerve palsy?
Incongruous homonymous hemianopia is caused by a lesion in which of the following?
Which of the following statements about Leber's hereditary optic neuropathy is FALSE?
Bergmeister papilla are present on which anatomical structure?
Foster Kennedy syndrome is associated with all of the following, except:
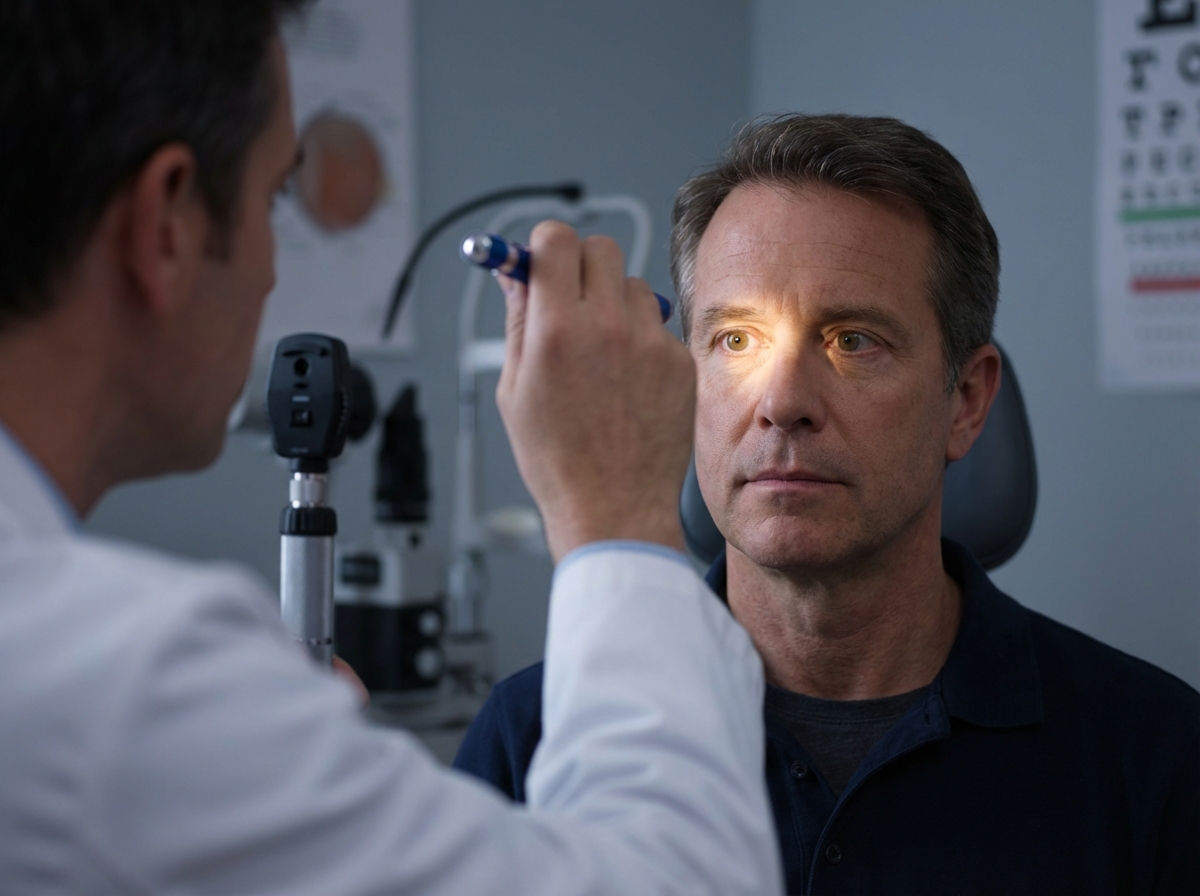
The shown procedure is helpful in diagnosing which condition?
Disc edema is not seen in which of the following conditions?
A patient presents with normal eyesight and absence of direct and consensual light reflexes. Which of the following cranial nerves is suspected to be lesioned?
What is the most common cause of optic neuritis?
Practice by Chapter
Anatomy of Visual Pathways
Practice Questions
Pupillary Disorders
Practice Questions
Optic Neuritis
Practice Questions
Ischemic Optic Neuropathies
Practice Questions
Other Optic Neuropathies
Practice Questions
Papilledema
Practice Questions
Cranial Nerve Palsies
Practice Questions
Nystagmus
Practice Questions
Visual Field Defects
Practice Questions
Neuro-ophthalmic Manifestations of Intracranial Lesions
Practice Questions
Functional Visual Disorders
Practice Questions
Migraine and the Eye
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
