Glaucoma — MCQs

On this page
What is the value of diurnal variation of intraocular pressure (IOP) above which a diagnosis of glaucoma can be made?
Cupping of optic disc is seen in:
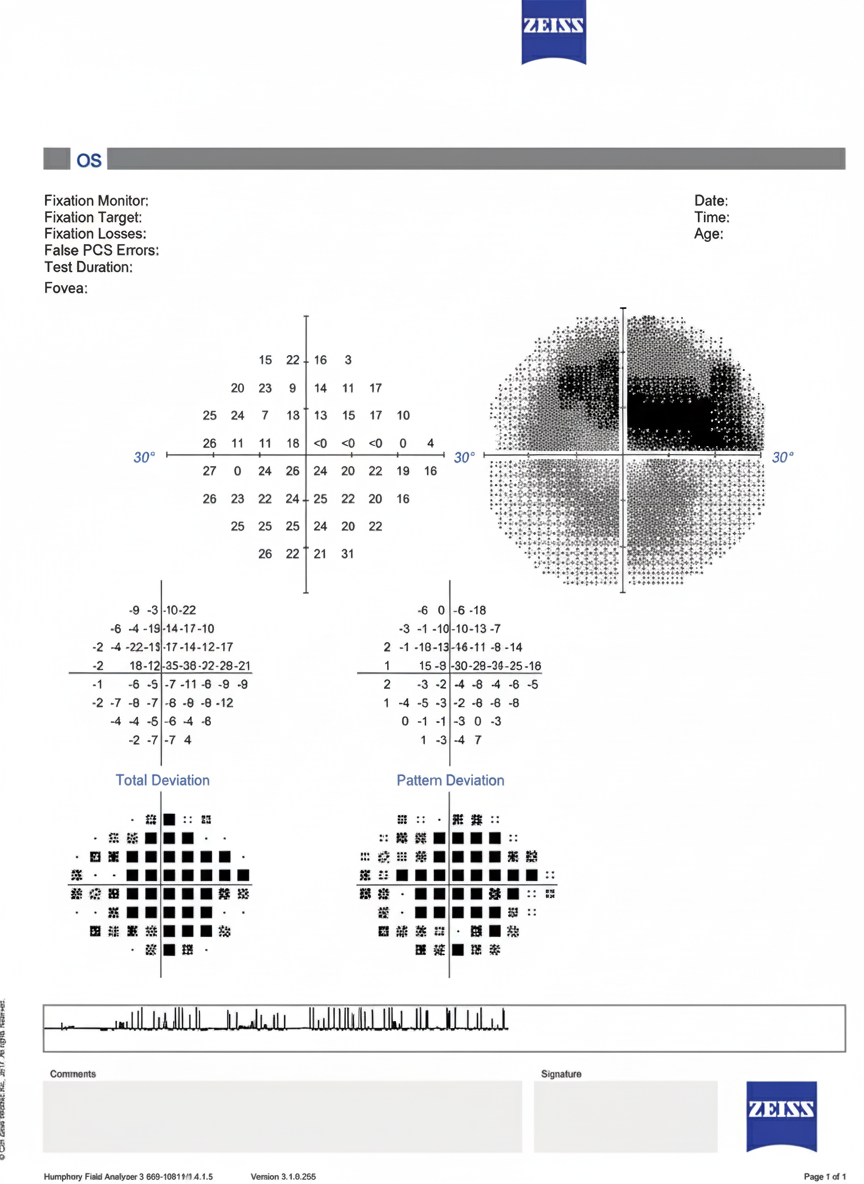
Which of the following statements is true regarding the given investigation?
All of the following conditions are contraindicated or likely to cause issues in a patient treated with Timolol maleate 0.5% eye drops for Primary Open Angle glaucoma, EXCEPT:
Schwalbe's line is:
A young male presents with painless loss of vision and an intraocular pressure of 60mm Hg. Which of the following is the most likely diagnosis?
All of the following can be seen in Axenfeld-Rieger syndrome, except?
Which of the following tonometers can be used in a diseased cornea?
What is the mechanism of steroid-induced glaucoma?
Haab's striae is seen in which of the following conditions?
Practice by Chapter
Aqueous Humor Dynamics
Practice Questions
Primary Open-Angle Glaucoma
Practice Questions
Primary Angle-Closure Glaucoma
Practice Questions
Secondary Open-Angle Glaucomas
Practice Questions
Secondary Angle-Closure Glaucomas
Practice Questions
Developmental and Congenital Glaucomas
Practice Questions
Medical Management of Glaucoma
Practice Questions
Laser Therapy in Glaucoma
Practice Questions
Glaucoma Filtration Surgery
Practice Questions
Glaucoma Drainage Devices
Practice Questions
Angle Assessment Techniques
Practice Questions
Visual Field Testing in Glaucoma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
