Glaucoma — MCQs

On this page
Which procedure is being done in the patient?
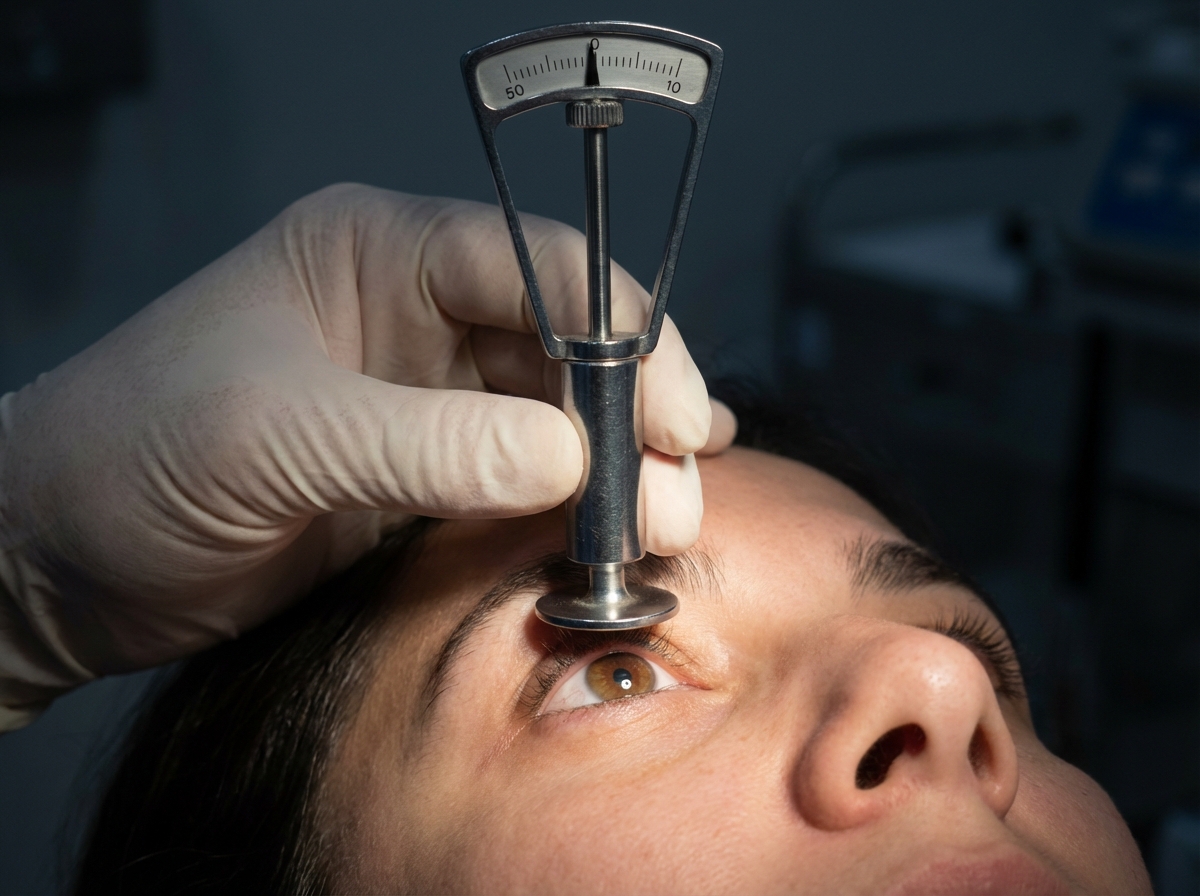
Pilocarpine is not used in young adults as it causes:
What is the main mechanism of action of brimonidine in glaucoma?
What is not true about the ciliary body?
Iridocorneal endothelial syndrome is associated with which of the following?
Laser trabeculoplasty is indicated in which of the following types of glaucoma?
The cause of a coloured halo in narrow angle glaucoma is?
What is the most common cause of neovascular glaucoma?
A patient with open-angle glaucoma and 7 diopters of myopia complains of blurring of vision after administration of pilocarpine. What is the reason for this blurring?
What is the classical sign of neovascular glaucoma?
Practice by Chapter
Aqueous Humor Dynamics
Practice Questions
Primary Open-Angle Glaucoma
Practice Questions
Primary Angle-Closure Glaucoma
Practice Questions
Secondary Open-Angle Glaucomas
Practice Questions
Secondary Angle-Closure Glaucomas
Practice Questions
Developmental and Congenital Glaucomas
Practice Questions
Medical Management of Glaucoma
Practice Questions
Laser Therapy in Glaucoma
Practice Questions
Glaucoma Filtration Surgery
Practice Questions
Glaucoma Drainage Devices
Practice Questions
Angle Assessment Techniques
Practice Questions
Visual Field Testing in Glaucoma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
