Blue Sclera Syndromes — MCQs

Most common cause of posterior staphyloma?
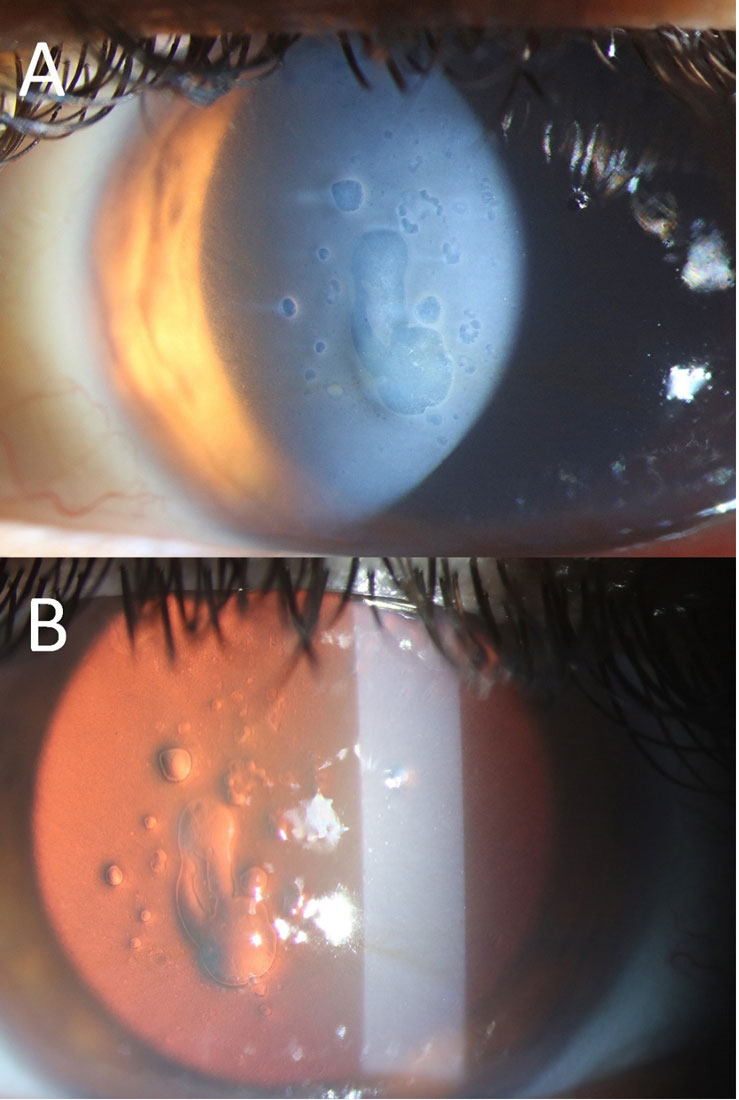
A patient, three years post-surgery, presents with the condition shown in the image and complains of decreased vision. What is the most likely diagnosis?
Which of the following is NOT a connective tissue disorder?
A 10-year-old boy presents with frequent fractures and blue sclerae. This patient most likely carries a mutation in a gene that encodes which of the following proteins?
Osteogenesis imperfecta is due to a defect in what?
Blue sclera is associated with:
Blue sclera is seen in-
Blue sclera is seen in all of the following conditions except:
An intrauterine scan at the 13th week of pregnancy showed a fetus with multiple long bone fractures. What is commonly associated with this finding?
A 22-year-old Air-force test pilot presents after flying a sortie. He reports no pain or vision changes. Eye examination reveals a localized red patch on the sclera. What is the most likely diagnosis?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
