Anatomy and Physiology of Sclera — MCQs

Type I collagen is present in all EXCEPT:
An example of a scleroprotein is
Normal intraocular pressure is typically in the range of:
Blue sclera is associated with:
A patient presents with a nodular swelling near the limbus, which does not blanch with topical vasoconstrictors and recurs after treatment. Based on the image and clinical presentation, what is the most probable diagnosis?
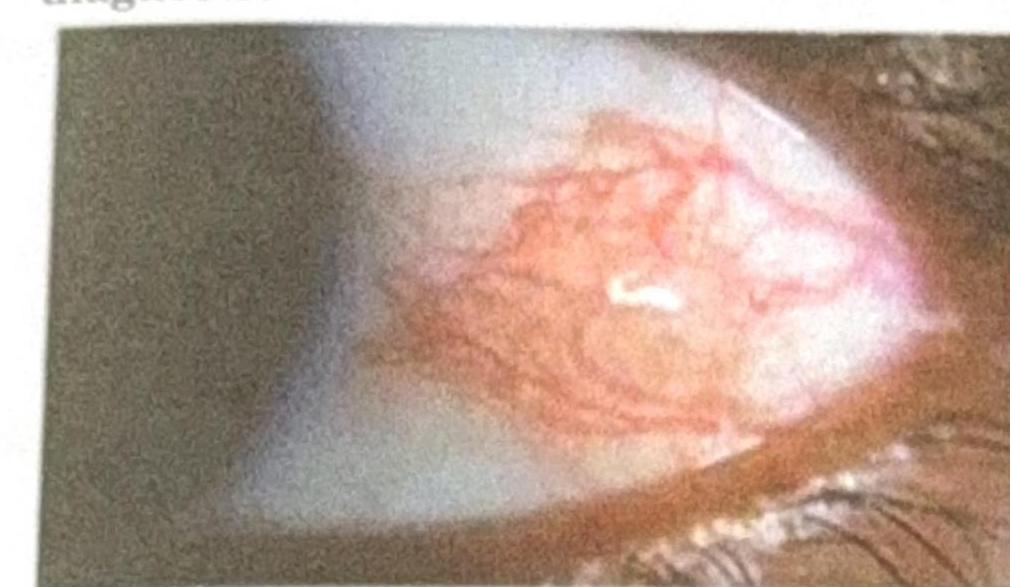
A 22-year-old Air-force test pilot presents after flying a sortie. He reports no pain or vision changes. Eye examination reveals a localized red patch on the sclera. What is the most likely diagnosis?
Blue sclera is seen in all of the following conditions except:
Evisceration is removal of which layer of eyeball?
Shortening of 2 mm of axial length of the eyeball causes?
Ciliary staphyloma is seen in which of the following conditions?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
