Diseases of the Retina — MCQs

On this page
The most typical clinical presentation of a retinoblastoma is
While working in a primary health centre, an elderly patient presents with a history of sudden loss of vision and curtain falling sensation in one eye. This symptom is highly suggestive that the patient has the following condition:
In diabetes mellitus the following findings are seen in ophthalmoscopy except:
A patient presents with sudden painful diminution of vision, difficulty looking in light (photophobia), and circumcorneal congestion with hypopyon. What is the most likely diagnosis?
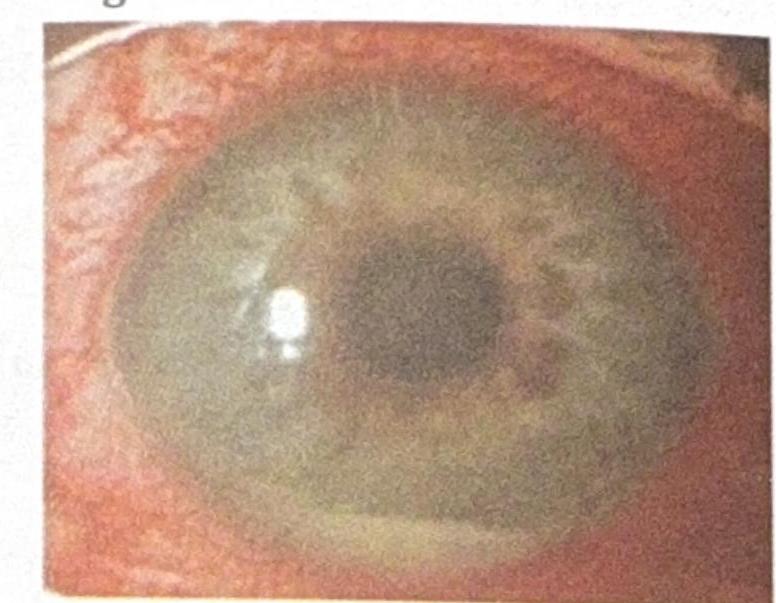
A patient presented with gradual loss in night vision and peripheral vision. Based on the fundoscopic image provided, what is the most likely diagnosis?
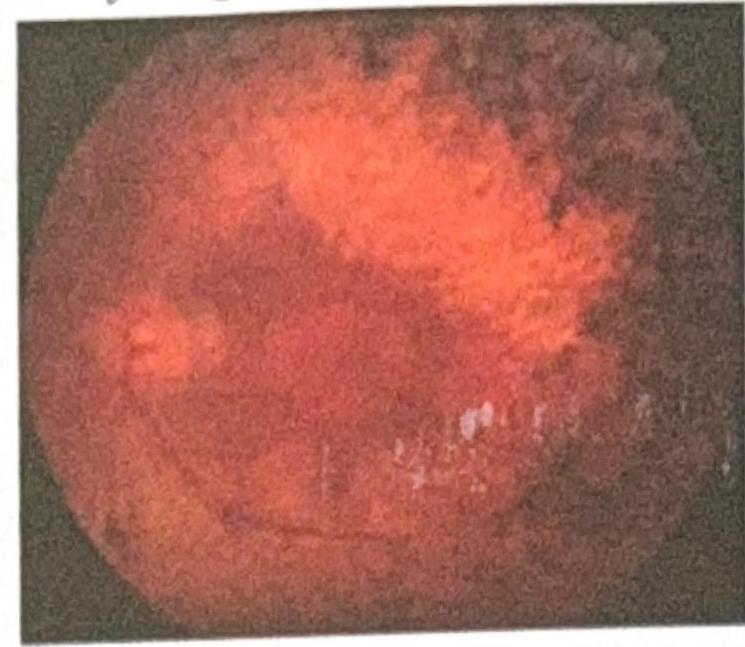
An elderly woman presented with gradual painless diminution of vision. The fundus picture is shown below. What is the most likely diagnosis?
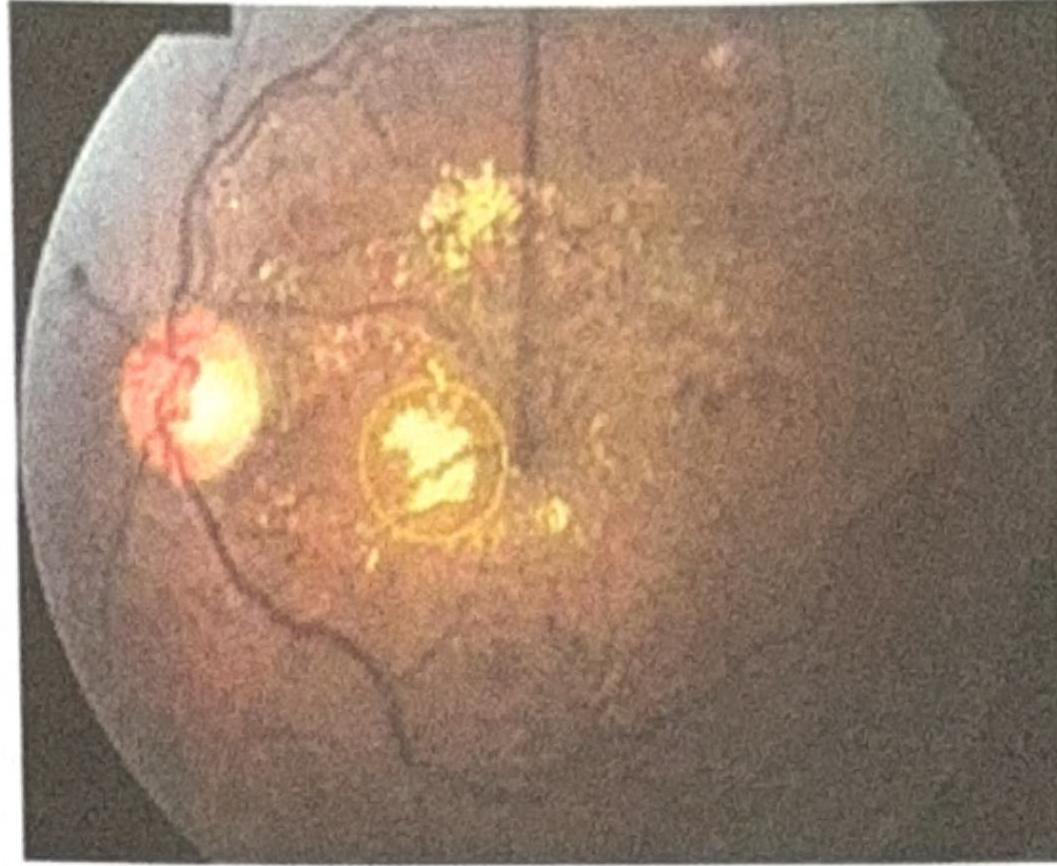
What is the most common route of the spread of retinoblastoma?
A 30-year-old female presents with redness and pain in the eye. Examination revealed 38 mm of Hg on IOP, aqueous flare, and corneal precipitates. Which of the following drugs must be avoided for her?
A 58-year-old woman is brought to the emergency room by her husband complaining, “I can’t see out of my right eye.” She was watching television last night when she covered her left eye due to an itch and discovered that she could not see. The patient denies any precipitating event, pain, swelling, flashes, floaters, or headaches. Her past medical history is significant for uncontrolled hypertension and angina. Her medications include hydrochlorothiazide, lisinopril, atorvastatin, and nitroglycerin as needed. Her physical examination is unremarkable. Fundus examination demonstrates generalized pallor and slight disc edema with no hemorrhages. What is the most likely explanation for this patient’s symptoms?
A fundus examination shows 'sunset glow' appearance. Which fluorescein angiography finding would best support Vogt-Koyanagi-Harada disease?
Practice by Chapter
Retinal Anatomy and Physiology
Practice Questions
Age-Related Macular Degeneration
Practice Questions
Diabetic Retinopathy
Practice Questions
Retinal Vascular Diseases
Practice Questions
Retinal Detachment
Practice Questions
Hereditary Retinal Dystrophies
Practice Questions
Inflammatory Retinal Diseases
Practice Questions
Retinal Tumors
Practice Questions
Retinopathy of Prematurity
Practice Questions
Retinal Imaging Techniques
Practice Questions
Intravitreal Pharmacotherapy
Practice Questions
Vitreoretinal Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
