Diseases of the Retina — MCQs

On this page
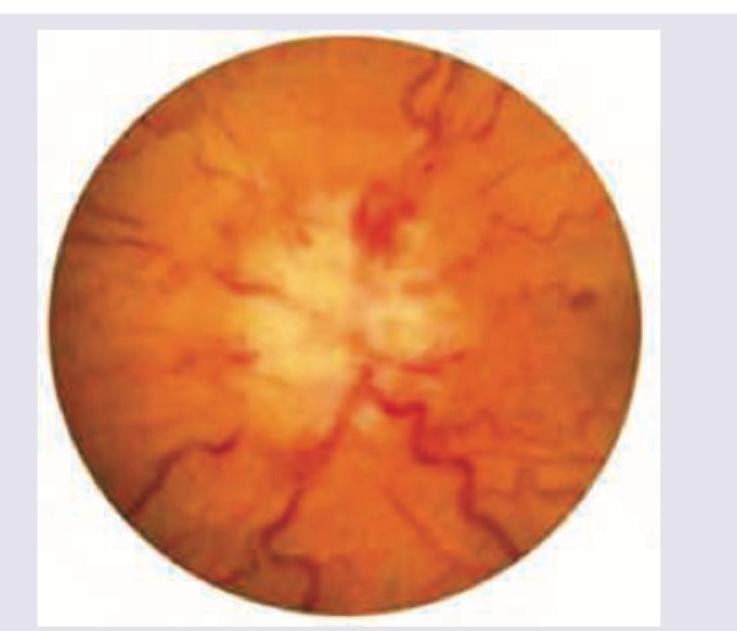
What does the following image show?
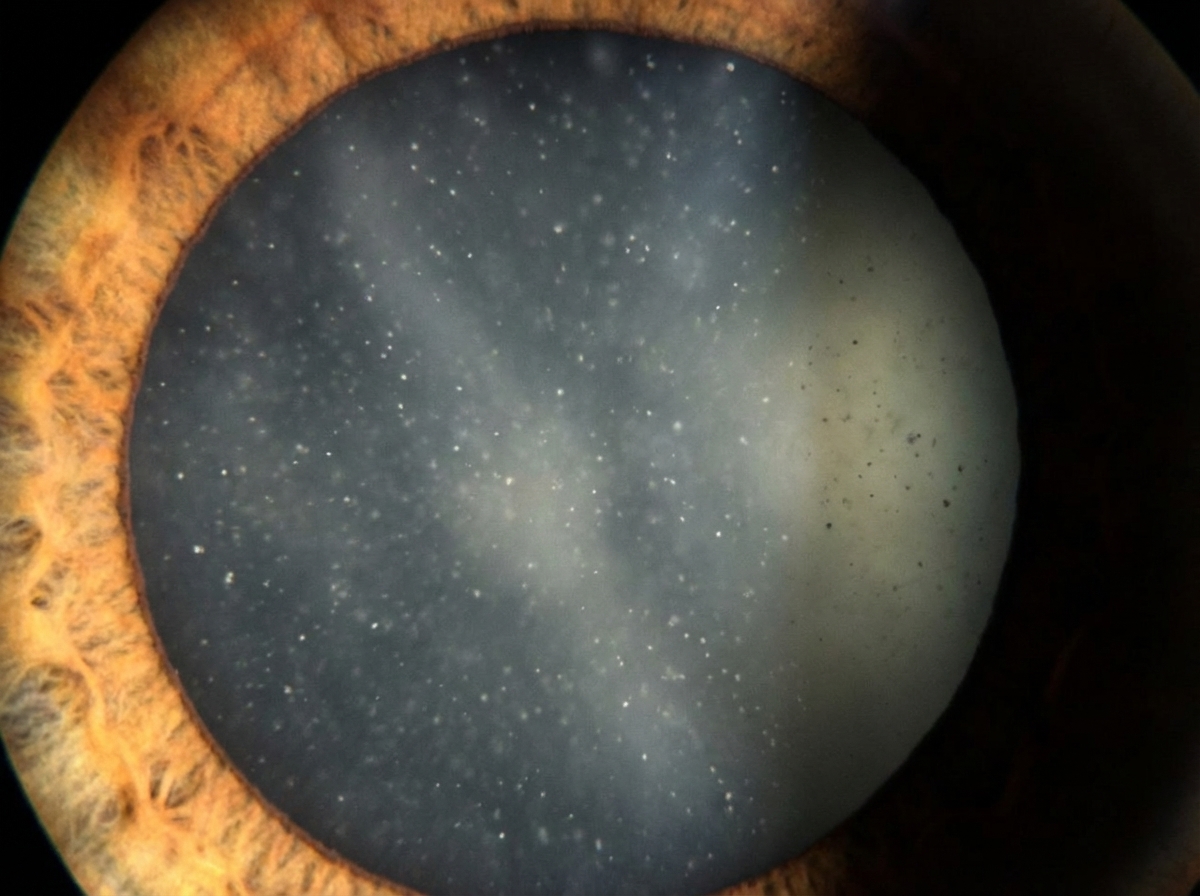
During annual medical check-up, a 55-year-old hypertensive corporate executive is found to have ophthalmoscopic findings as shown in the image given below. What is it composed of?
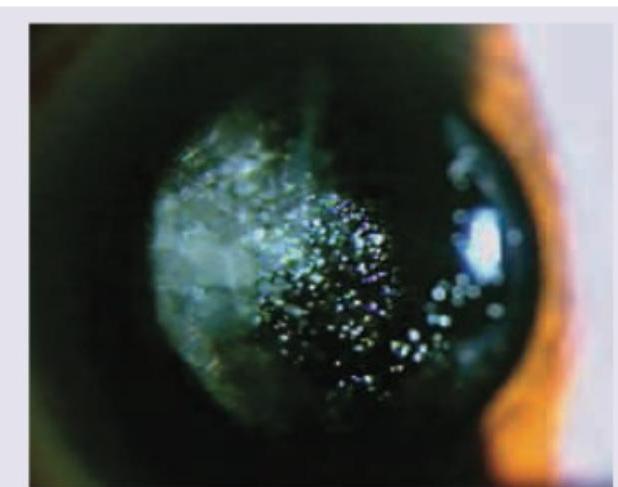
All of the following are responsible for the condition shown in the image except:
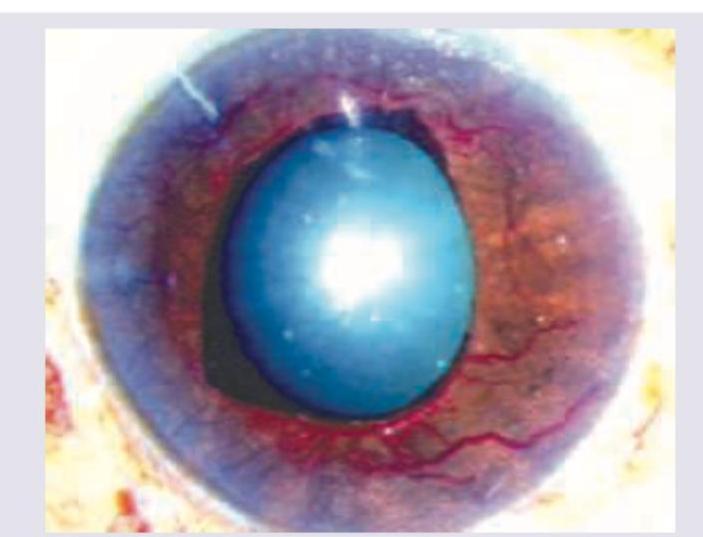
All are true about the recording shown except:
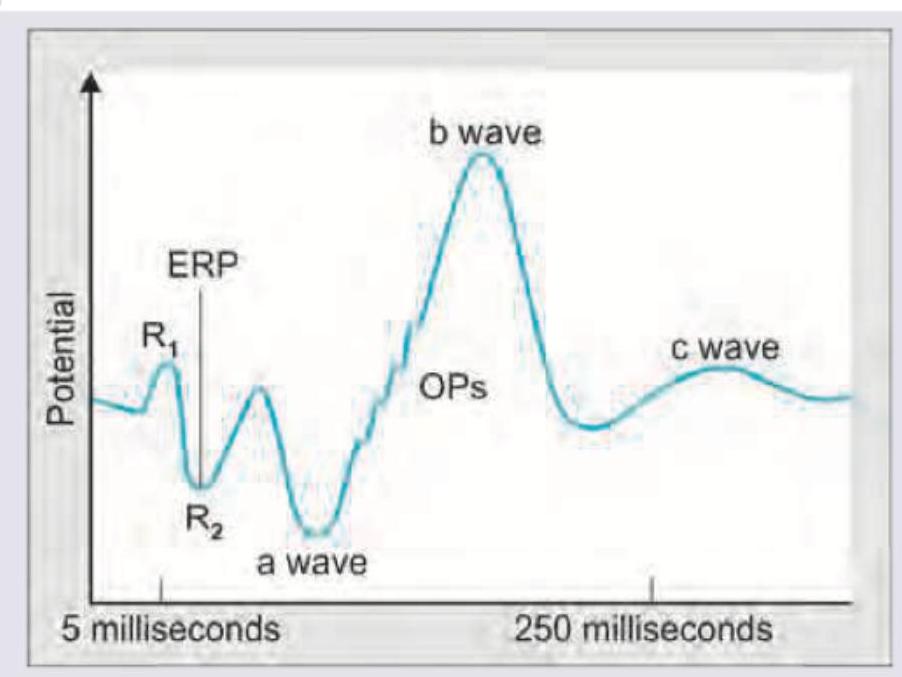
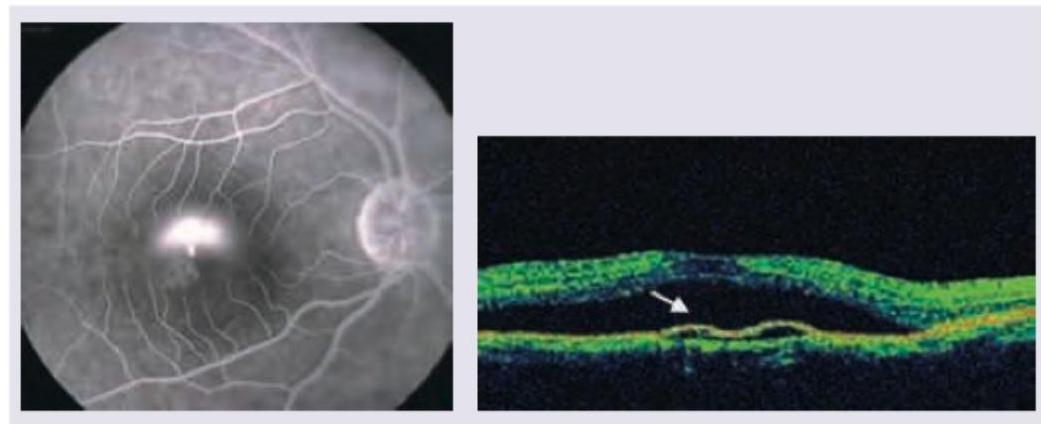
A 25-year-old young male presented with complaints of diminished vision in the right eye. On examination vision in left eye is 6/6 and right eye is 6/18. Shown are the FFA and optical coherence topography of the patient. The pathology lies in which layer of retina?
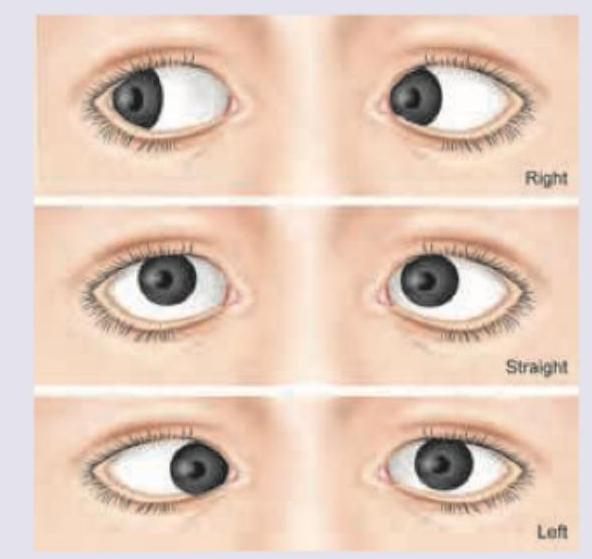
A 60-year-old male underwent a cataract surgery. After 1 year he came with complaints of diminished vision and the finding shown in the image. Diagnosis is?
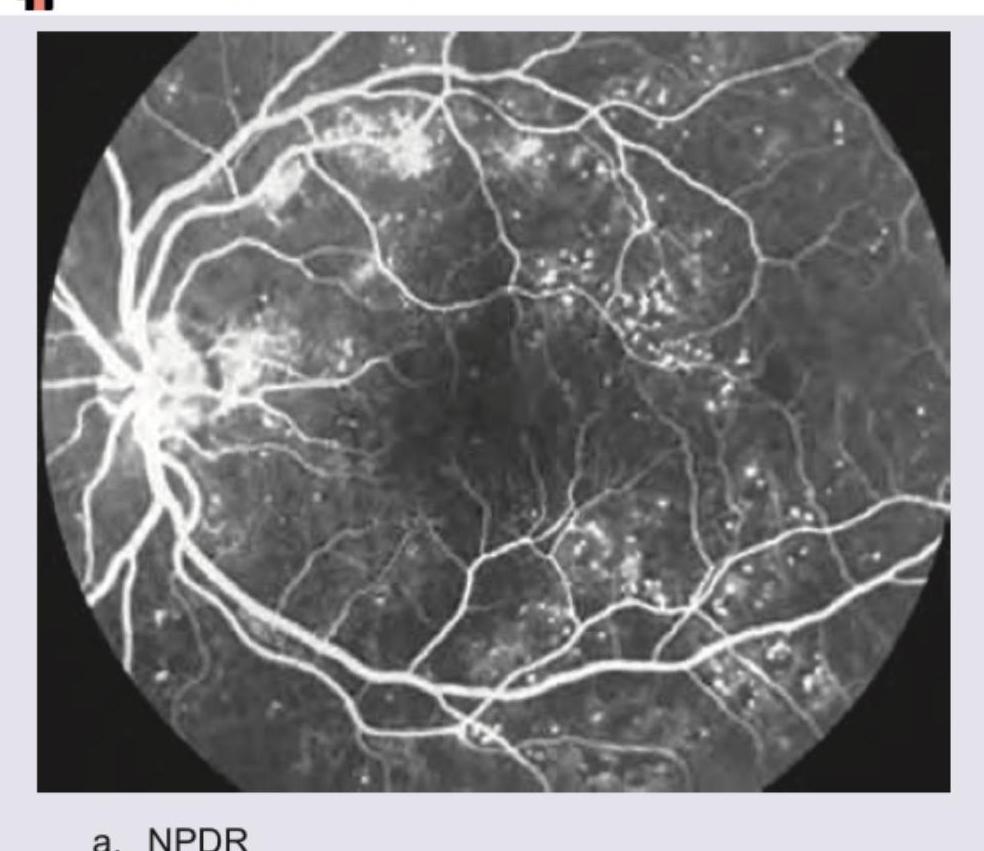
Identify the FFA picture:
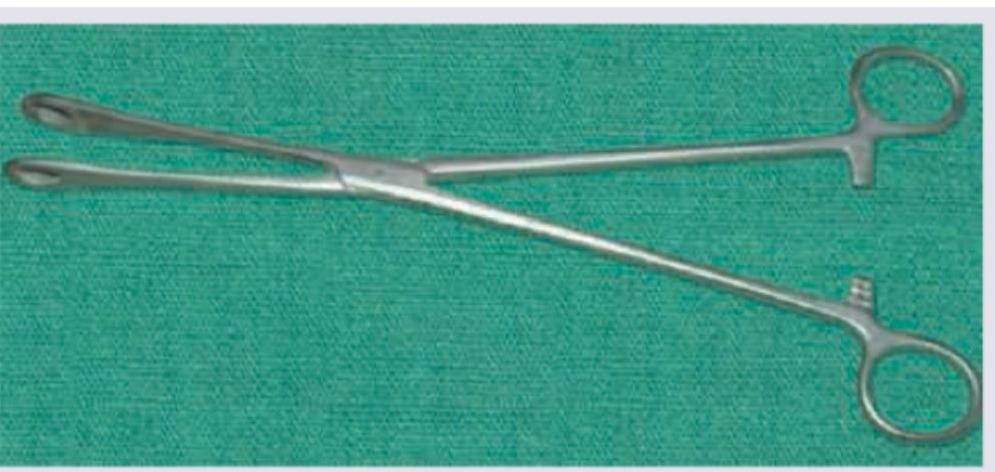
Identify the instrument:
The following fundus finding is seen in:
Consider the following causes of visual loss : 1. Obstruction of the central retinal artery 2. Vitreous and retinal haemorrhage 3. Cataract 4. Retinal detachment Which of the above causes are associated with acute visual loss in a patient?
Practice by Chapter
Retinal Anatomy and Physiology
Practice Questions
Age-Related Macular Degeneration
Practice Questions
Diabetic Retinopathy
Practice Questions
Retinal Vascular Diseases
Practice Questions
Retinal Detachment
Practice Questions
Hereditary Retinal Dystrophies
Practice Questions
Inflammatory Retinal Diseases
Practice Questions
Retinal Tumors
Practice Questions
Retinopathy of Prematurity
Practice Questions
Retinal Imaging Techniques
Practice Questions
Intravitreal Pharmacotherapy
Practice Questions
Vitreoretinal Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
