Diseases of the Retina — MCQs

On this page
Retinitis pigmentosa is not associated with which of the following conditions?
Which of the following is NOT a feature of non-proliferative diabetic retinopathy?
Waxy pallor of the optic disc is seen in which disease?
What is the peak sensitivity of retinal rods and cones pigment in the most refractive eyes?
What is the diameter of the macula lutea?
Uveal effusion syndrome may be associated with all of the following, except:
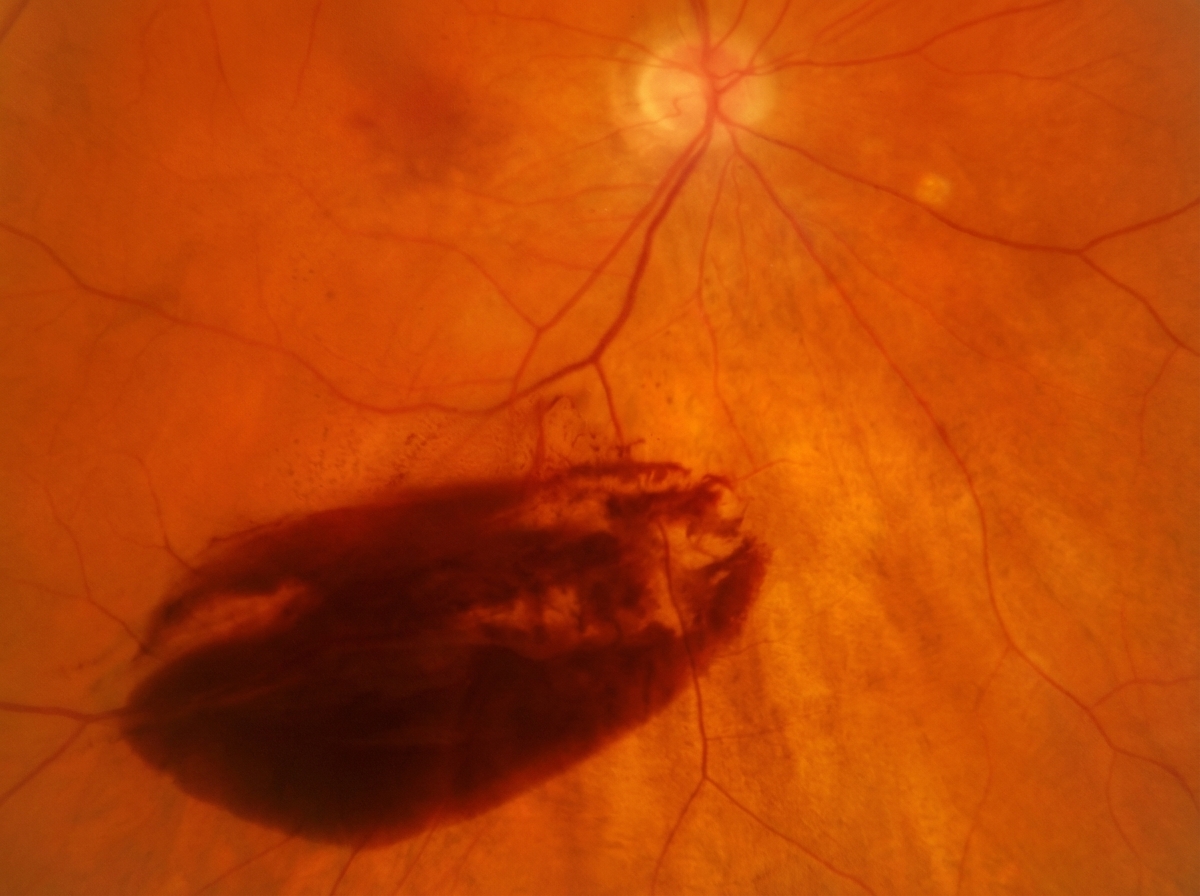
A 25-year-old male presents with painless sudden loss of vision. Ocular and systemic examinations are not contributory. What is the probable diagnosis?
Select the incorrect statement about this condition?
Microaneurysms in diabetic retinopathy are typically found in which retinal layer?
What is the most common site for a retinal break?
Practice by Chapter
Retinal Anatomy and Physiology
Practice Questions
Age-Related Macular Degeneration
Practice Questions
Diabetic Retinopathy
Practice Questions
Retinal Vascular Diseases
Practice Questions
Retinal Detachment
Practice Questions
Hereditary Retinal Dystrophies
Practice Questions
Inflammatory Retinal Diseases
Practice Questions
Retinal Tumors
Practice Questions
Retinopathy of Prematurity
Practice Questions
Retinal Imaging Techniques
Practice Questions
Intravitreal Pharmacotherapy
Practice Questions
Vitreoretinal Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
