Diseases of the Retina — MCQs

On this page
What is the most common etiology of recurrent vitreous hemorrhage in a young patient?
'Bull's eye' lesion in the macular region is seen in which of the following conditions?
Exudative retinal detachment occurs in which of the following conditions?
The retina is embryologically derived from which of the following germ layers?
The fundus photograph shown is characteristic of which of the following conditions?
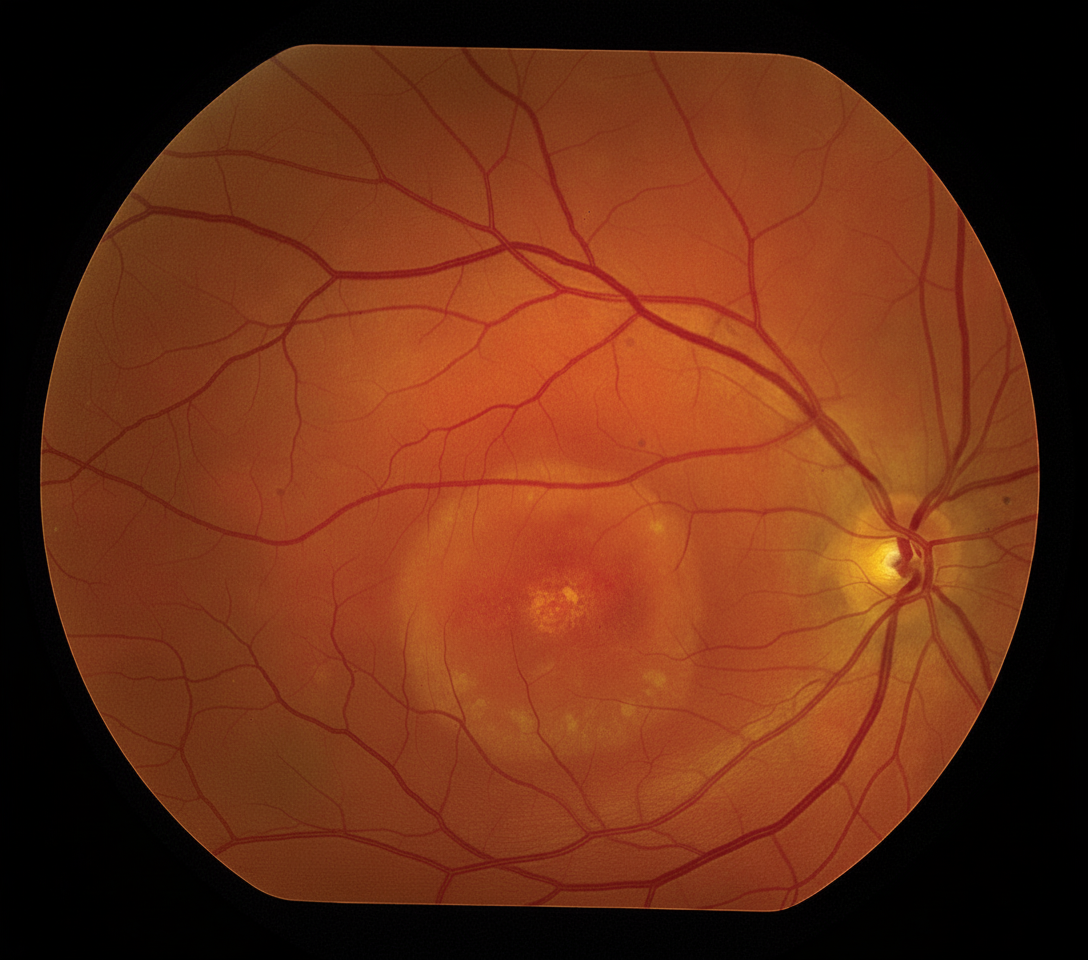
A 65-year-old man presents with metamorphopsia. On examination, he has yellow deposits subretinal near the macula in both eyes. The rest of the fundus is normal. What is the probable diagnosis?
Which gas is used for retinal tamponade?
A 7-year-old child presents with left exotropia. The right eye has 6/6 vision with a normal fundus. The left eye has only close hand movements, with subretinal yellow exudates, retinal detachment, and telangiectatic vessels. What is the diagnosis?
Macular involvement is common in which of the following infections?
Epidemic dropsy is characterised by all EXCEPT:
Practice by Chapter
Retinal Anatomy and Physiology
Practice Questions
Age-Related Macular Degeneration
Practice Questions
Diabetic Retinopathy
Practice Questions
Retinal Vascular Diseases
Practice Questions
Retinal Detachment
Practice Questions
Hereditary Retinal Dystrophies
Practice Questions
Inflammatory Retinal Diseases
Practice Questions
Retinal Tumors
Practice Questions
Retinopathy of Prematurity
Practice Questions
Retinal Imaging Techniques
Practice Questions
Intravitreal Pharmacotherapy
Practice Questions
Vitreoretinal Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
