Diseases of the Retina — MCQs

On this page
Which one of the following is a serious complication of degenerative myopia?
A cherry red spot is seen in which of the following conditions, except?
What is the diagnosis in this 31-year-old woman with gradual bilateral vision loss?
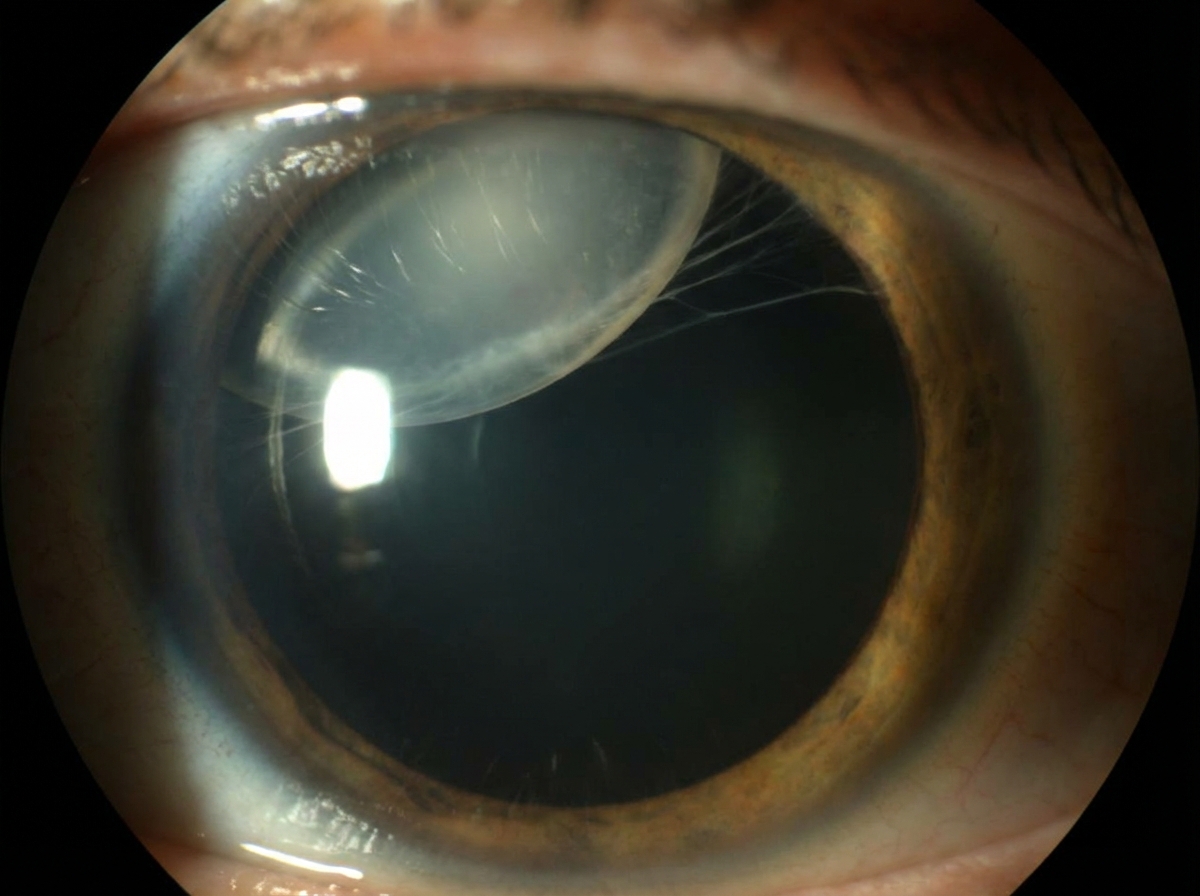
What is the largest field of vision in a normal human eye?
Angioid streaks are seen in which of the following conditions?
Argus 2 implants have been experimentally tried in which of the following conditions?
Hard exudates are seen in all the following conditions except?
Which of the following is the most common cause of vitreous hemorrhage in young individuals?
Which of the following conditions is NOT a differential diagnosis for retinoblastoma?
Syneresis refers to:
Practice by Chapter
Retinal Anatomy and Physiology
Practice Questions
Age-Related Macular Degeneration
Practice Questions
Diabetic Retinopathy
Practice Questions
Retinal Vascular Diseases
Practice Questions
Retinal Detachment
Practice Questions
Hereditary Retinal Dystrophies
Practice Questions
Inflammatory Retinal Diseases
Practice Questions
Retinal Tumors
Practice Questions
Retinopathy of Prematurity
Practice Questions
Retinal Imaging Techniques
Practice Questions
Intravitreal Pharmacotherapy
Practice Questions
Vitreoretinal Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
