Diseases of the Lens — MCQs

On this page
Oil drop cataract is characteristic of which condition?
Sunflower cataract is due to deposition of:
What is the treatment of choice in aphakia?
Zonular cataract is seen in?
What is the primary treatment for traumatic cataract in children?
What is the best site for a 101 implant?
Polyopia is a symptom of which of the following conditions?
Which of the following is NOT an indication for intracapsular cataract extraction?
What is your diagnosis based on the provided image?
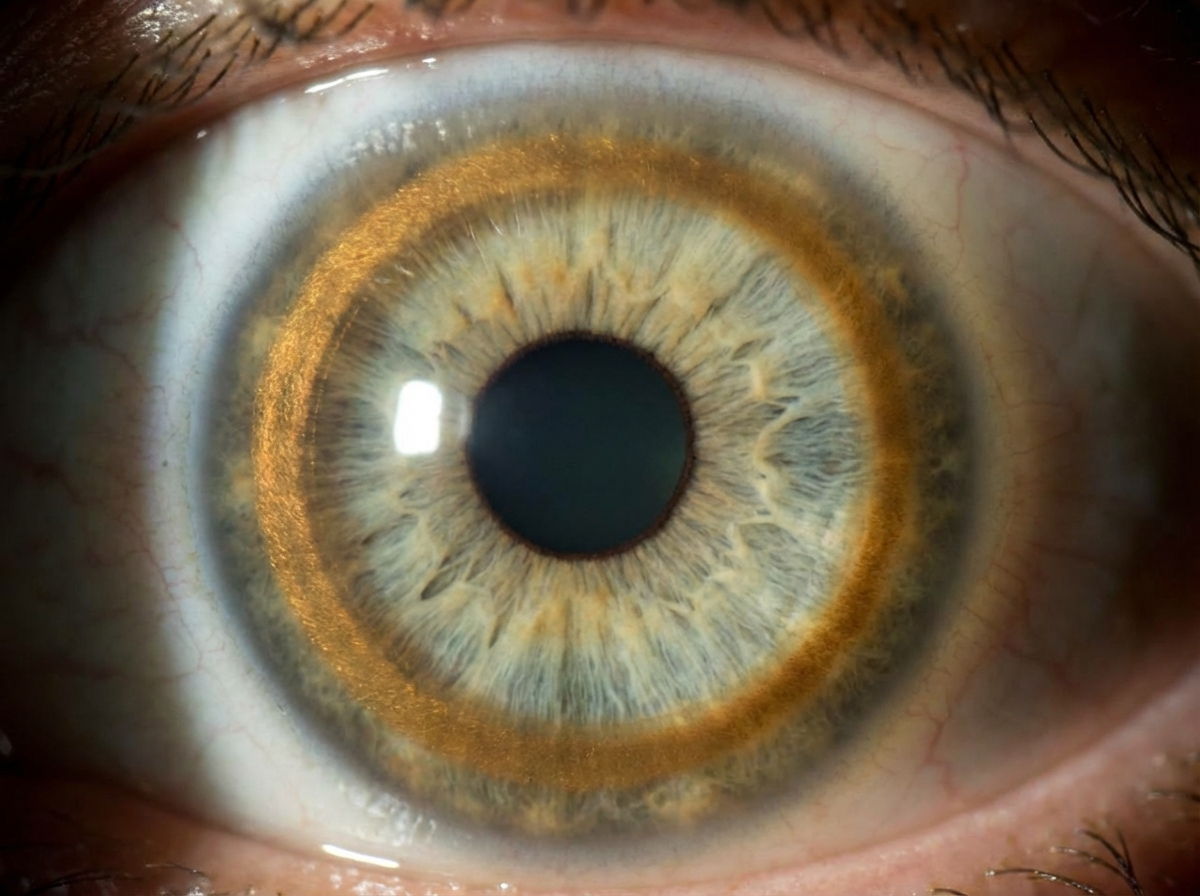
Sunflower cataract is associated with:
Practice by Chapter
Lens Anatomy and Physiology
Practice Questions
Age-Related Cataract
Practice Questions
Congenital and Developmental Cataracts
Practice Questions
Traumatic Cataract
Practice Questions
Metabolic Cataracts
Practice Questions
Drug-Induced Cataracts
Practice Questions
Cataract Surgery Techniques
Practice Questions
Intraocular Lens Implants
Practice Questions
Complications of Cataract Surgery
Practice Questions
Posterior Capsular Opacification
Practice Questions
Lens Subluxation and Dislocation
Practice Questions
Specialty IOLs
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
