Diseases of the Lens — MCQs

On this page
Identify the instrument shown.
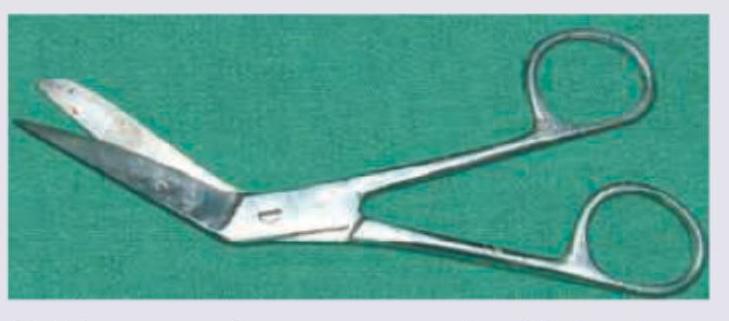
Rosette cataract is seen after:
Constantly changing refractive error is seen in:
Which laser is used in the management of posterior capsule opacification (PCO)?
Which of the following is not true about the difference between congenital cataract surgery and senile cataract surgery?
All are true except:
All of the following are causes of congenital blindness Except:
Which ocular condition is associated with "snowflake" cataracts?
A 50-year-old male presents with decreased vision and frequent changes in his glasses prescription. Examination reveals a clear cornea and increasing myopia. What is the most likely cause?
A 65-year-old male presents with difficulty reading fine print and seeing objects at a distance. Examination reveals a myopic shift in both eyes. What is the most likely cause?
Practice by Chapter
Lens Anatomy and Physiology
Practice Questions
Age-Related Cataract
Practice Questions
Congenital and Developmental Cataracts
Practice Questions
Traumatic Cataract
Practice Questions
Metabolic Cataracts
Practice Questions
Drug-Induced Cataracts
Practice Questions
Cataract Surgery Techniques
Practice Questions
Intraocular Lens Implants
Practice Questions
Complications of Cataract Surgery
Practice Questions
Posterior Capsular Opacification
Practice Questions
Lens Subluxation and Dislocation
Practice Questions
Specialty IOLs
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
