Diseases of the Cornea — MCQs

On this page
KF ring is seen in which of the following conditions?
Corneal deposits are seen in all of these conditions except?
Which of the following is NOT true regarding the treatment of bacterial corneal ulcer?
Keratomalacia includes the following except?
Keratomalacia is a clinical manifestation associated with which of the following conditions?
In Keratoconus, all are seen except?
What is the diagnostic test for a corneal ulcer?
Marginal catarrhal corneal ulcer is caused by which of the following?
The central nebular corneal opacity is best treated with which procedure?
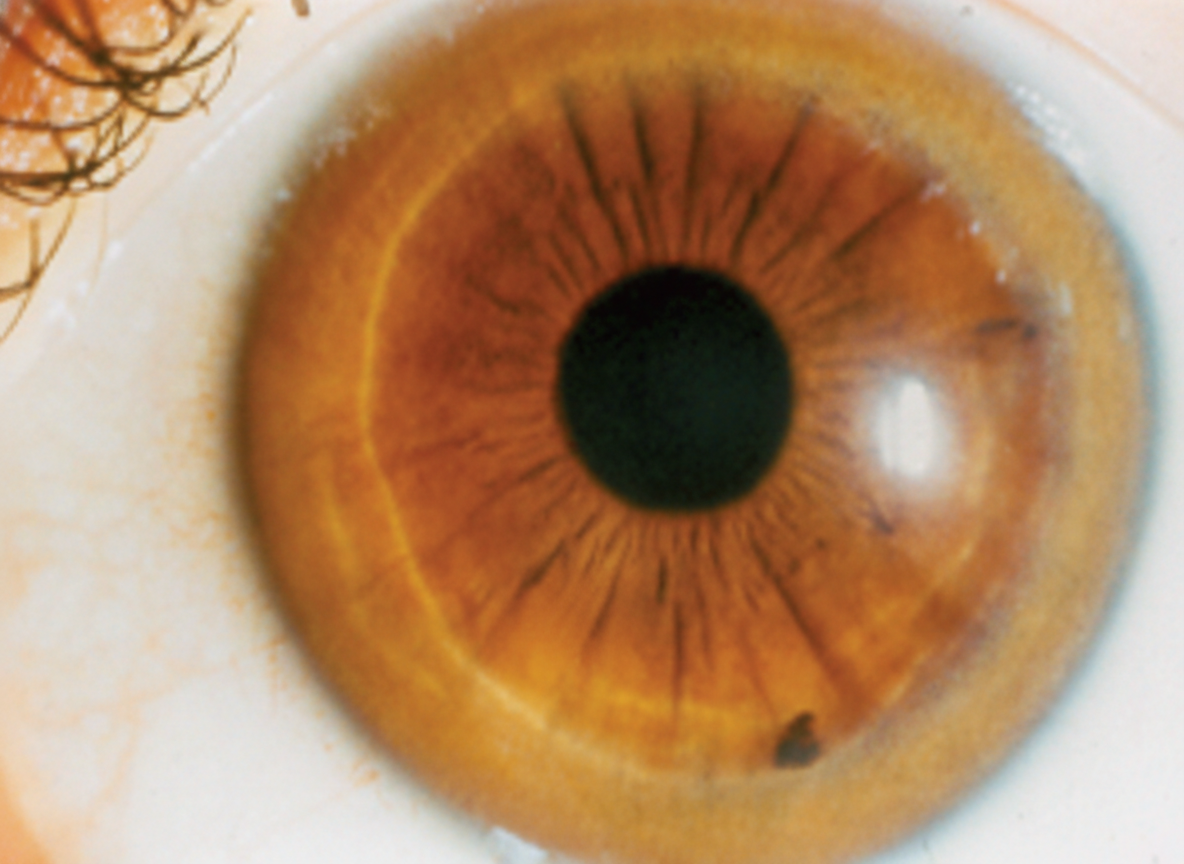
Diagnose the condition.
Practice by Chapter
Corneal Anatomy and Physiology
Practice Questions
Bacterial Keratitis
Practice Questions
Viral Keratitis
Practice Questions
Fungal Keratitis
Practice Questions
Protozoan Keratitis
Practice Questions
Corneal Degenerations
Practice Questions
Corneal Dystrophies
Practice Questions
Keratoconus and Ectatic Disorders
Practice Questions
Corneal Transplantation
Practice Questions
Corneal Topography and Imaging
Practice Questions
Dry Eye Disease
Practice Questions
Corneal Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
