Diseases of the Cornea — MCQs

On this page
Corneal scraping from a patient reveals narrow angled septate hyphae. What is the most likely etiologic agent?
All are features of rosacea keratitis except?
Which of the following is NOT an indication for the prosthesis shown in the image?
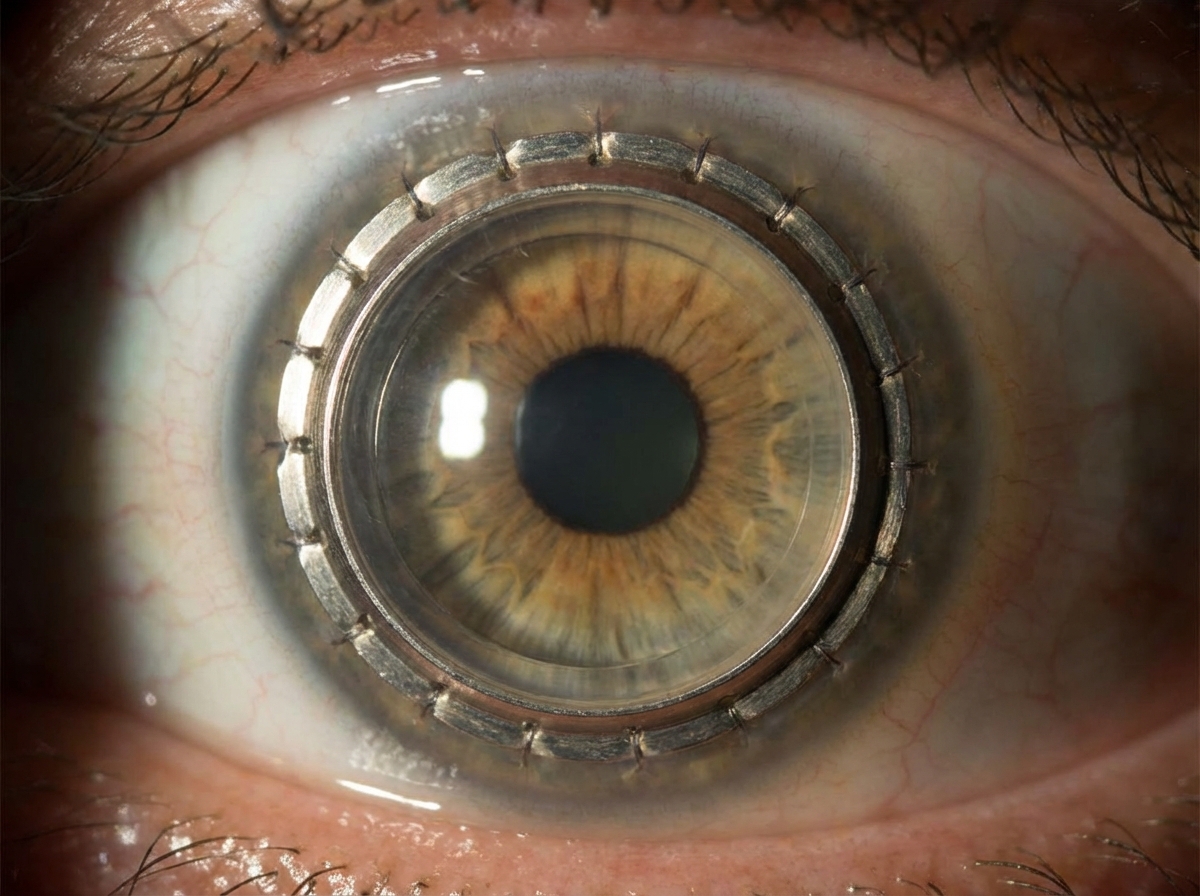
Which of the following statements regarding corneal transplantation is true?
What is the most common cause of corneal keratitis in soft contact lens users?
Enlarged corneal nerves may be seen in all of the following except?
Under hypoxic conditions, which of the following is strongly implicated as a cause of corneal edema?
Keratic precipitates are found on which layer of the cornea?
Hutchinson’s rule is related to which of the following conditions?
Keratitis can be caused by which of the following?
Practice by Chapter
Corneal Anatomy and Physiology
Practice Questions
Bacterial Keratitis
Practice Questions
Viral Keratitis
Practice Questions
Fungal Keratitis
Practice Questions
Protozoan Keratitis
Practice Questions
Corneal Degenerations
Practice Questions
Corneal Dystrophies
Practice Questions
Keratoconus and Ectatic Disorders
Practice Questions
Corneal Transplantation
Practice Questions
Corneal Topography and Imaging
Practice Questions
Dry Eye Disease
Practice Questions
Corneal Trauma
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
