Corneal Anatomy and Physiology — MCQs

All are true regarding cornea except:
Sensory innervation of the cornea is by which nerve?
Density of cells in adult corneal endothelium is
Conjunctival epithelium is a type of what?
Which among the following is the BEST irrigating fluid during ECCE?
A 20-year-old male complains of repeated changes in glasses prescription. This is most likely caused by:
In uveitis, site of keratic precipitate is:
Which of the following statements about Fuchs' corneal dystrophy is true?
What does a visual acuity test primarily assess?
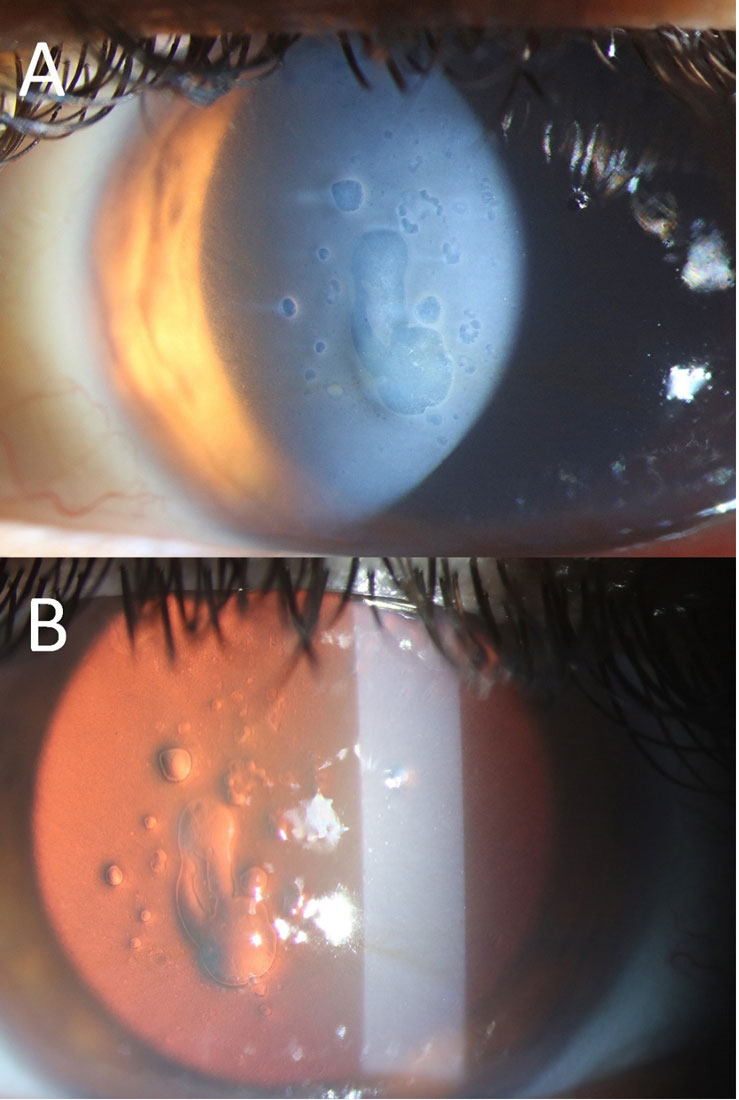
A patient, three years post-surgery, presents with the condition shown in the image and complains of decreased vision. What is the most likely diagnosis?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
