Diseases of the Conjunctiva — MCQs

On this page
Regarding spring catarrh, all of the following are true, except:
Inclusion conjunctivitis is caused by which of the following pathogens?
Which of the following are features of vernal keratoconjunctivitis?
Which of the following are features of vernal keratoconjunctivitis?
The finding seen in the image is:
A young person with recurrent seasonal conjunctivitis presents with itchiness and eye-watering. What is the most likely cell involved in the immediate phase of this condition?
Acute hemorrhagic conjunctivitis is caused by which of the following combinations?
A 25 -year-old patient presents with localized redness in right eye as shown below. On instillation of 10% phenylephrine there is quick blanching of the vessels. What is the diagnosis?
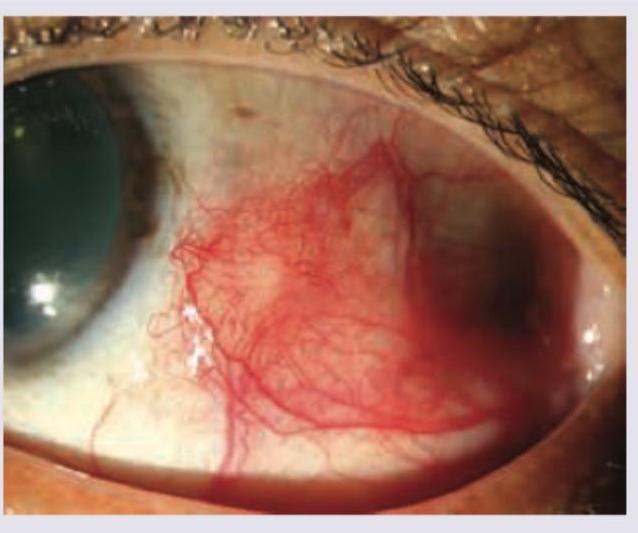
What is the diagnosis shown in the image?
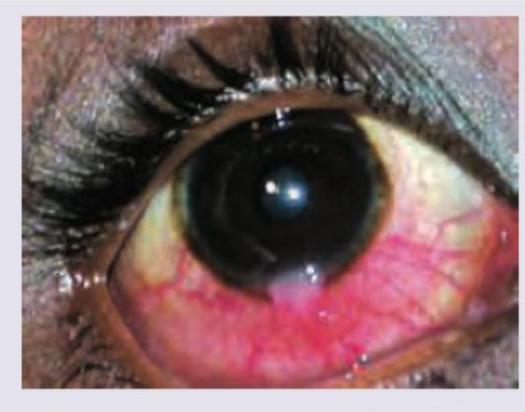
A patient presents with chronic redness and discharge from the eye. The image shows the conjunctival findings. What is the most likely diagnosis?
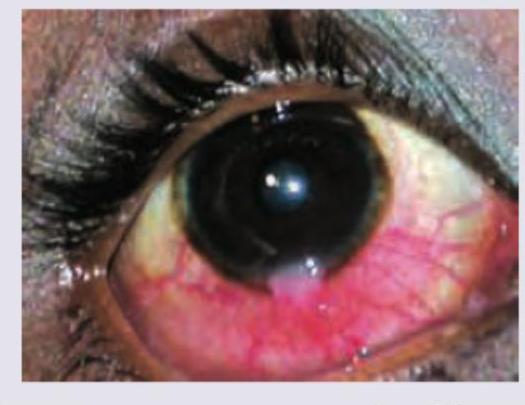
Practice by Chapter
Conjunctivitis: Bacterial
Practice Questions
Conjunctivitis: Viral
Practice Questions
Conjunctivitis: Allergic
Practice Questions
Conjunctivitis: Chronic
Practice Questions
Degenerations of Conjunctiva
Practice Questions
Benign Tumors of Conjunctiva
Practice Questions
Malignant Tumors of Conjunctiva
Practice Questions
Conjunctival Manifestations of Systemic Diseases
Practice Questions
Cicatricial Conjunctival Disorders
Practice Questions
Pterygium and Pinguecula
Practice Questions
Conjunctival Trauma
Practice Questions
Subconjunctival Hemorrhage
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
