Diseases of the Conjunctiva — MCQs

On this page
Which is the most common etiologic agent of Phlyctenular conjunctivitis?
Conjunctival xerosis is seen in all of the following except?
Which of the following is NOT a feature of Ocular Mucous Membrane Pemphigoid?
Which of the following is NOT a corneal sign of trachoma?
Blepharitis acarica is caused by which of the following?
Cicatrising trachoma is seen in which stage?
Which of the following is NOT true regarding epidemic keratoconjunctivitis?
Arlt's line is seen in which condition?
Herbert's pits are seen in which condition?
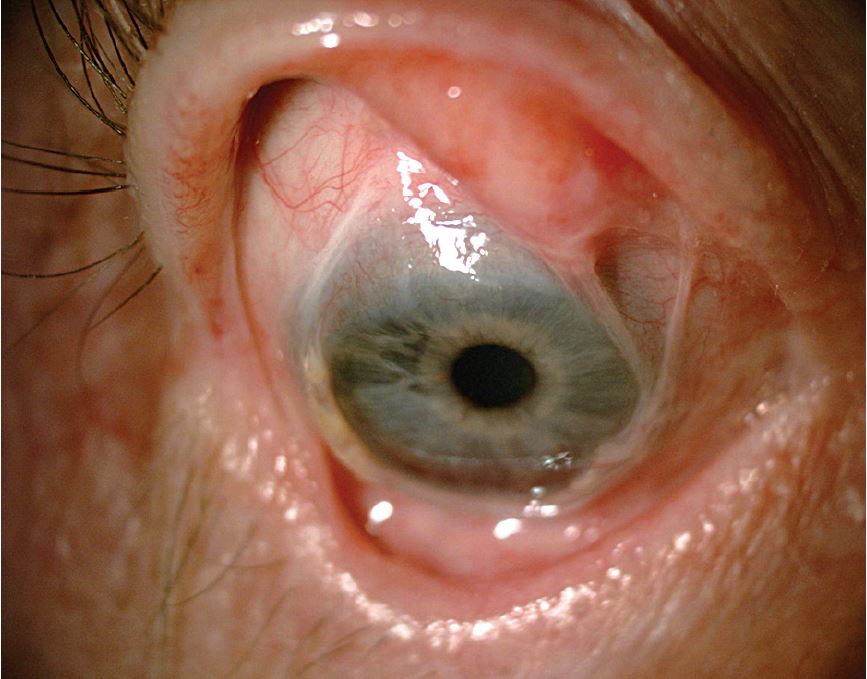
Diagnosis of the given condition is:
Practice by Chapter
Conjunctivitis: Bacterial
Practice Questions
Conjunctivitis: Viral
Practice Questions
Conjunctivitis: Allergic
Practice Questions
Conjunctivitis: Chronic
Practice Questions
Degenerations of Conjunctiva
Practice Questions
Benign Tumors of Conjunctiva
Practice Questions
Malignant Tumors of Conjunctiva
Practice Questions
Conjunctival Manifestations of Systemic Diseases
Practice Questions
Cicatricial Conjunctival Disorders
Practice Questions
Pterygium and Pinguecula
Practice Questions
Conjunctival Trauma
Practice Questions
Subconjunctival Hemorrhage
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
