Conjunctivitis: Viral — MCQs

A 25-year-old male presents with recurrent bilateral conjunctival hyperemia and a gritty sensation. Likely diagnosis?
Unilateral frontal blisters with upper lid edema and conjunctivitis is seen in?
Which condition is characterized by conjunctival injection, pharyngeal injection, polymorphic rash, and cervical lymphadenopathy?
Statement 1 - A 59-year-old patient presents with flaccid bullae. Histopathology shows a suprabasal acantholytic split. Statement 2 - The row of tombstones appearance is diagnostic of Pemphigus vulgaris.
Features of vernal conjunctivitis are:
Which of the following is a contraindication to topical steroids?
In a patient with acute anterior uveitis presenting with raised intraocular pressure, the PRIMARY treatment should be:
Not a feature of ligneous conjunctivitis:
Regarding Chlamydia infection of the eyes, true statements include the following except:
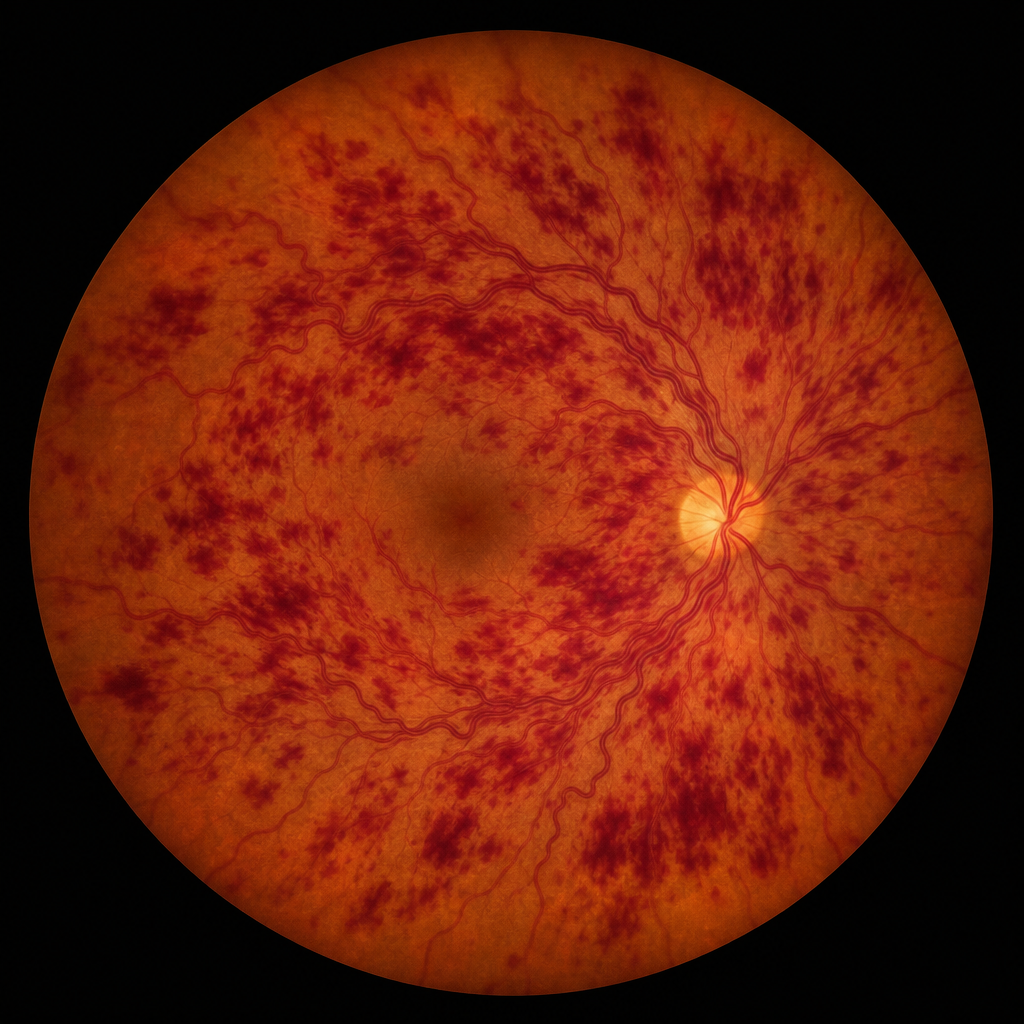
A 58-year-old hypertensive woman presents with sudden painless loss of vision in her left eye noticed on waking. Her blood pressure is 168/96 mmHg. There is no relative afferent pupillary defect. The fundus photograph of the left eye shows diffuse venous tortuosity and widespread retinal hemorrhages in all four quadrants, consistent with central retinal vein occlusion (Image 3). Which of the following investigations is most important to guide immediate management and reduce the risk of neovascular complications?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
