Eye Banking and Corneal Transplantation — MCQs

All of the following conditions are immediate priorities in the WHO's "Vision -2020: The Right to sight" except:
Acute corneal hydrops is seen in:
What is the primary mechanism responsible for skin graft survival within the first 48 hours after transplantation?
Among the following organisms, which is the most common cause of postoperative endophthalmitis following corneal transplantation?
Which of the following procedures is not typically covered by the National Programme for Control of Blindness (NPCB) for reimbursement of surgery done by a non-governmental organization (NGO) eye hospital?
What is the most likely complication of the condition shown in the image below?
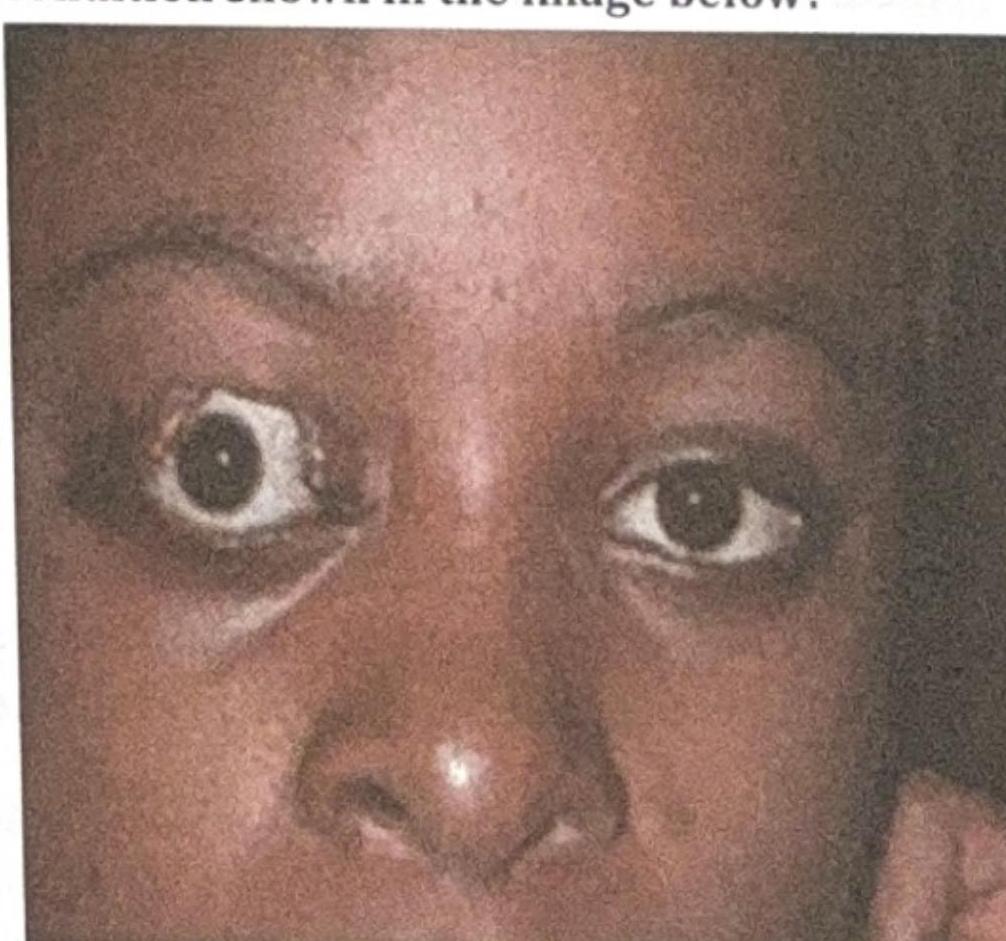
All of the following are true about Keratoconus, except:
The golden period of eye donation is
A patient complained of gradual diminution of vision. On examination, the patient had dry eyes and a rough corneal surface. What deficiency is most likely causing these manifestations?
In a patient with acute anterior uveitis presenting with raised intraocular pressure, the PRIMARY treatment should be:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
