Basic Sciences as Related to Eye — MCQs

On this page
In bitewing radiographs, occlusal pit caries of enamel appears as a:
Chronic dacryocystitis is most commonly due to what condition?
The arrow points towards which anatomical structure?
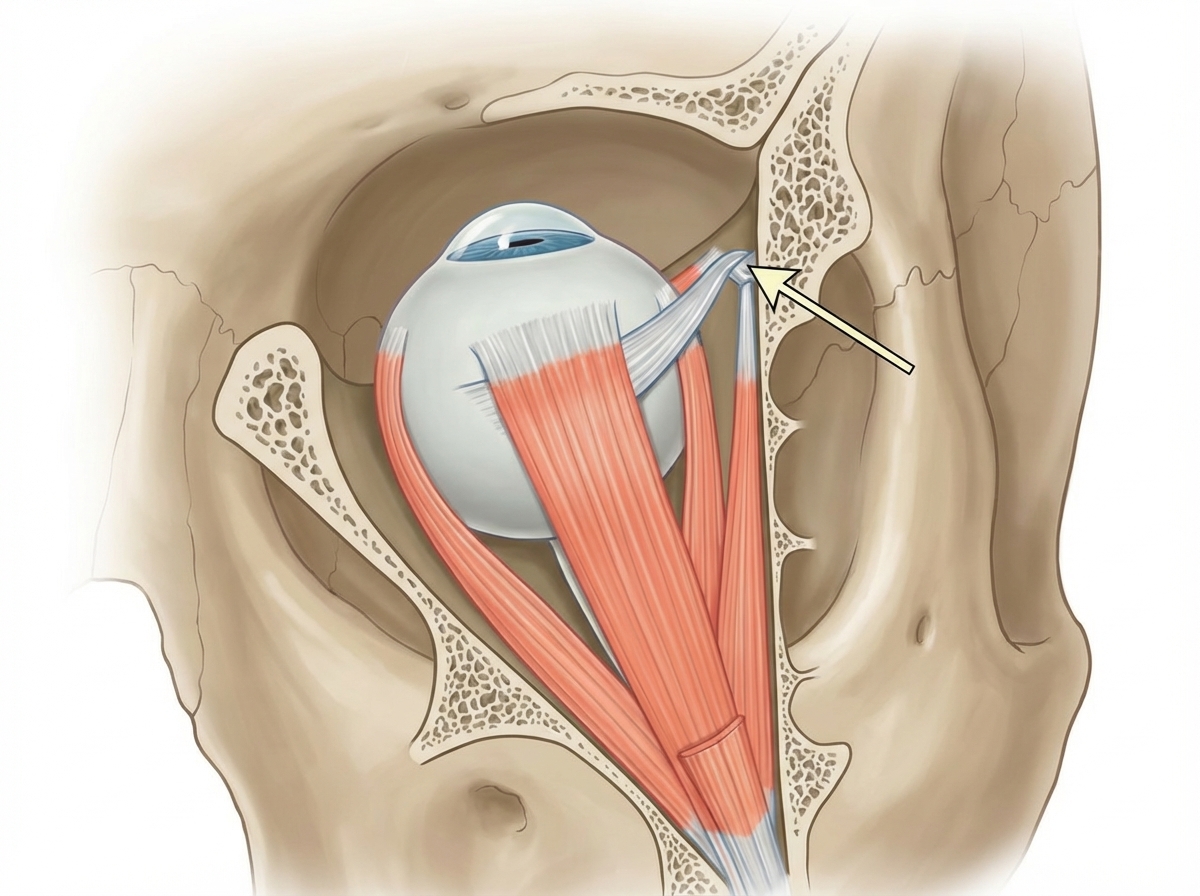
The Hasner valve is seen in which of the following structures?
Normal aqueous production rate is about:
The electroretinogram may assist in the diagnosis of all of the following, except:
The arrow marked sign is due to deposition of which substance?
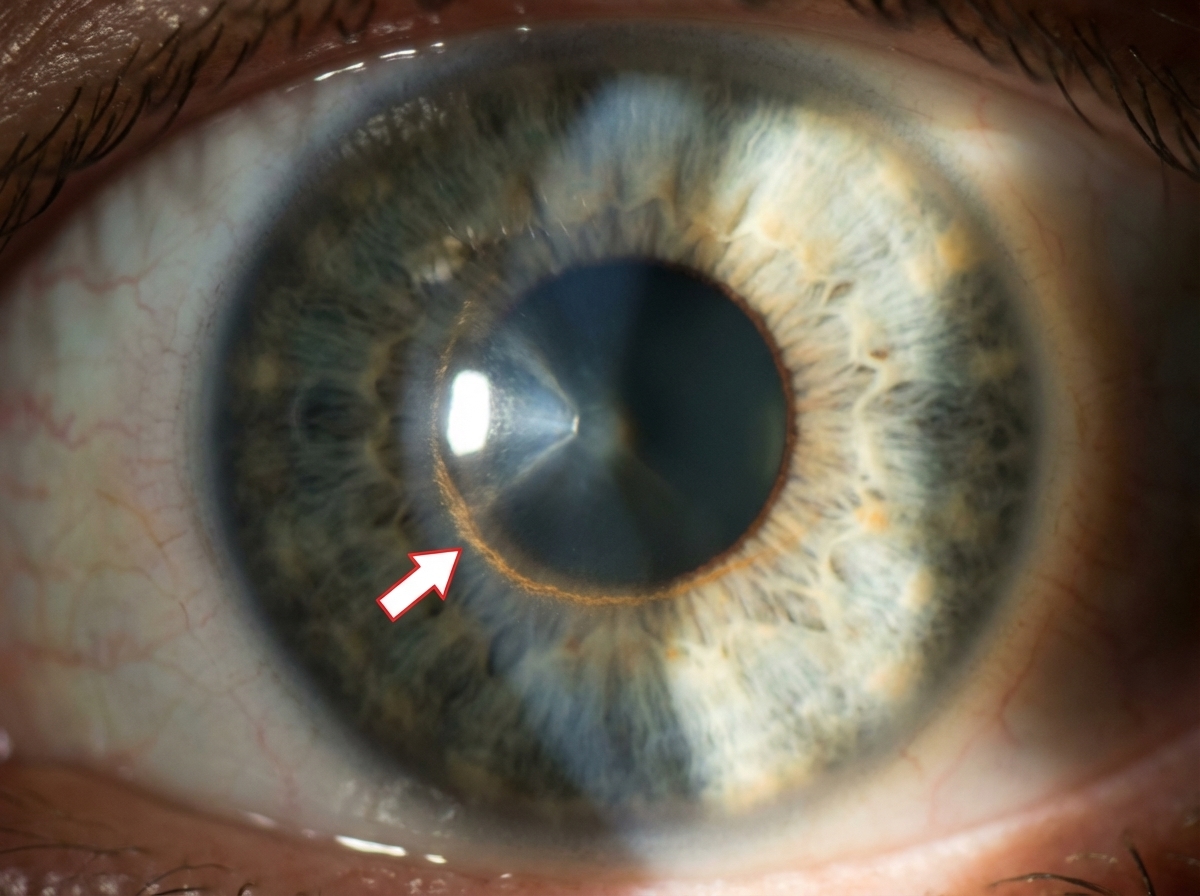
What is the most common etiological variety of uveitis?
Which instrument is used to visualize the corneal endothelium?
Hypopyon consists of:
Practice by Chapter
Embryology of Eye
Practice Questions
Ocular Anatomy
Practice Questions
Ocular Physiology
Practice Questions
Ocular Biochemistry
Practice Questions
Ocular Microbiology
Practice Questions
Ocular Pharmacology
Practice Questions
Ocular Pathology
Practice Questions
Ocular Genetics
Practice Questions
Ocular Immunology
Practice Questions
Visual Neuroscience
Practice Questions
Ocular Imaging Physics
Practice Questions
Laser Physics in Ophthalmology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
