Basic Sciences as Related to Eye — MCQs

On this page
A chalazion is best described as:
What is the primary muscle responsible for the intorsion of the eye?
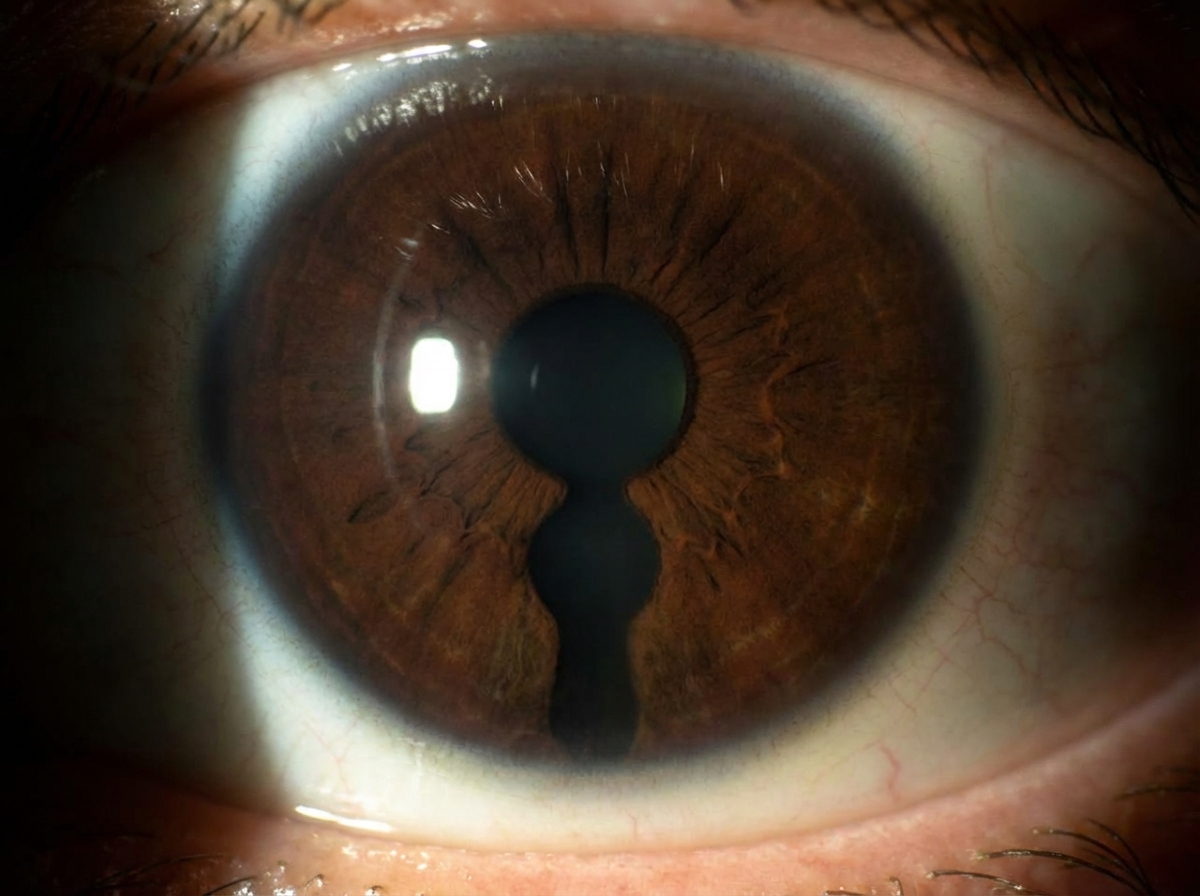
What term is used to describe the finding?
What is the normal size of an optic disc in diameter?
Lysozyme and lactoferrin are present in which layer of the tear film?
Optical coherence tomography is akin to which in vivo imaging technique?
Meibomian glands secrete which component of tears?
What is the weight of an adult eyeball?
Which muscles are responsible for the elevation of the eye?
Panuveitis involves which part(s) of the eye?
Practice by Chapter
Embryology of Eye
Practice Questions
Ocular Anatomy
Practice Questions
Ocular Physiology
Practice Questions
Ocular Biochemistry
Practice Questions
Ocular Microbiology
Practice Questions
Ocular Pharmacology
Practice Questions
Ocular Pathology
Practice Questions
Ocular Genetics
Practice Questions
Ocular Immunology
Practice Questions
Visual Neuroscience
Practice Questions
Ocular Imaging Physics
Practice Questions
Laser Physics in Ophthalmology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
