Reproductive Endocrinology — MCQs

On this page
All of the following are raised in PCOS except?
Which of the following is NOT a feature of Stein-Leventhal syndrome?
What percentage of females with polycystic ovary syndrome (PCOS) experience oligomenorrhea?
Sexual infantilism is associated with which of the following conditions?
Which of the following is NOT a typical symptom or sign of Polycystic Ovarian Disease (PCOD)?
All of the following statements about Androgen Insensitivity Syndrome are true except?
Determination of serum progesterone level to document ovulation. For the evaluation, select the most appropriate day of a normal 28-day menstrual cycle for a woman with 5-day menstrual periods.
What is the best agent for premenstrual syndrome management?
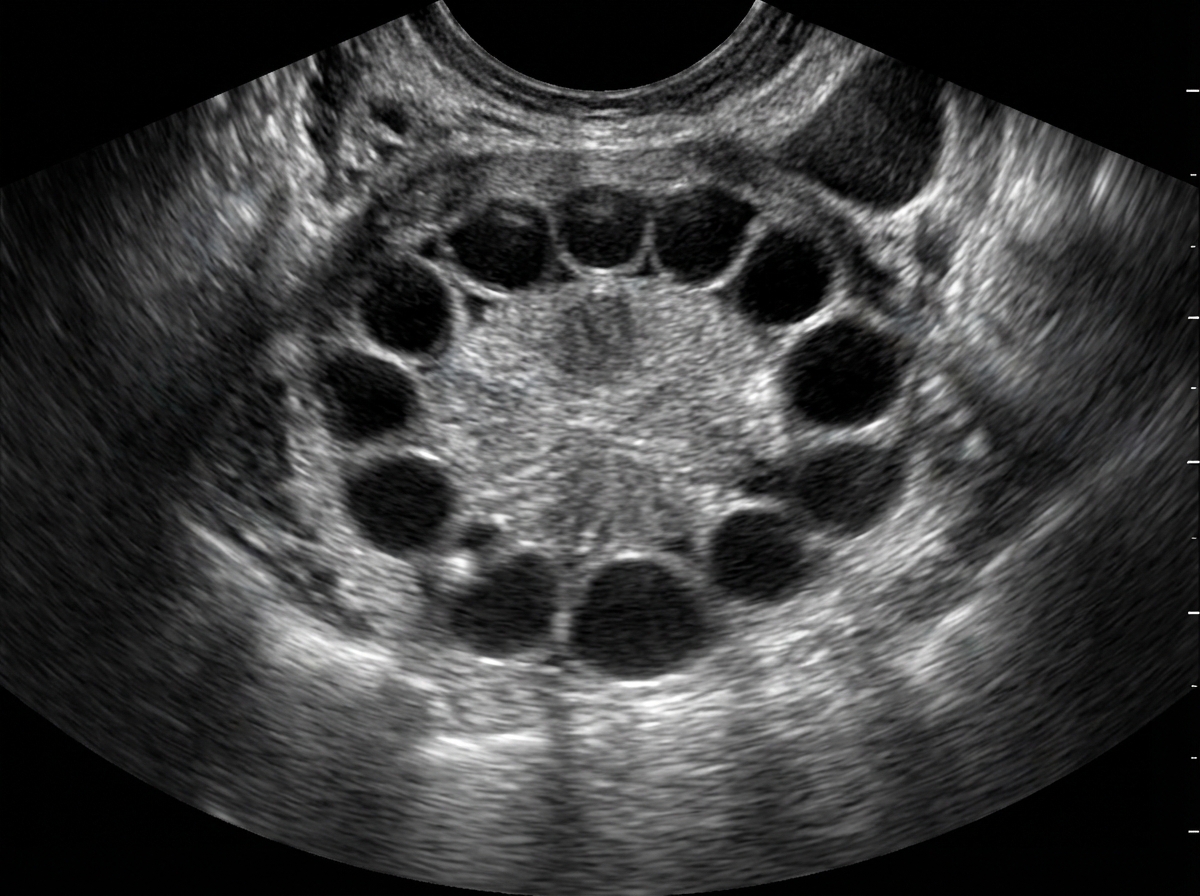
A patient presents with a history of amenorrhea and hirsutism. Ultrasound of the ovary is provided. What is the most likely diagnosis?
A 16-year-old female has not yet started having menstrual cycles. Her secondary sex characteristics appear normal, as does external examination of her genitalia. She is given an intramuscular injection of progesterone, and 5 days later she has her first period. What is the most likely mechanism responsible for the delay in menses?
Practice by Chapter
Hypothalamic-Pituitary-Ovarian Axis
Practice Questions
Disorders of Puberty
Practice Questions
Hirsutism and Virilization
Practice Questions
Primary Ovarian Insufficiency
Practice Questions
Hyperprolactinemia
Practice Questions
Hyperandrogenism
Practice Questions
Metabolic Dysfunction in PCOS
Practice Questions
Neuroendocrine Disorders and Reproduction
Practice Questions
Hormonal Evaluation and Testing
Practice Questions
Ovulation Induction
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
