Reproductive Endocrinology — MCQs

On this page
Which of the following is the most important indication for Strassman Metroplasty for a bicornuate uterus?
Which among the following hormones acts on post ovulatory endometrium?
A 12-year-old girl presents with primary amenorrhea. She has been raised as a girl, has not developed breast tissue, and ultrasound reveals absence of the uterus. Karyotyping shows a 46 XY chromosomal pattern. What is the most likely diagnosis?
A 12-year-old female presents with Tanner stage II breast development and white, odorless vaginal discharge. This discharge is most likely due to the action of which hormone?
A 25-year-old female presents with irregular menstrual cycles, acne, and excessive hair growth. An ultrasound reveals multiple ovarian cysts. What is the most likely diagnosis?
A 27-year-old woman presents with irregular periods, acne & excessive hair growth. What is the first line management?
A female presents with hirsutism, delayed periods, obesity. USG findings are given below. What is the likely diagnosis?
A woman is diagnosed with a pituitary microadenoma and has elevated serum prolactin levels. She presents with secondary amenorrhea and infertility. What is the most likely mechanism by which hyperprolactinemia causes these symptoms?
In a woman with a regular 28-day menstrual cycle, which of the following best describes the typical hormonal profile during days 21 to 25 of the cycle?
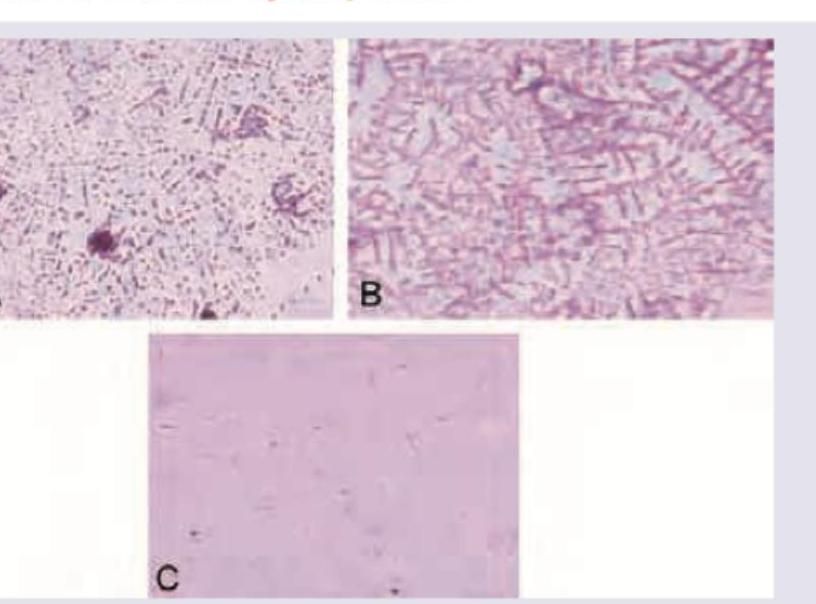
Which of the following cervical mucus smear represents the mid-cycle period?
Practice by Chapter
Hypothalamic-Pituitary-Ovarian Axis
Practice Questions
Disorders of Puberty
Practice Questions
Hirsutism and Virilization
Practice Questions
Primary Ovarian Insufficiency
Practice Questions
Hyperprolactinemia
Practice Questions
Hyperandrogenism
Practice Questions
Metabolic Dysfunction in PCOS
Practice Questions
Neuroendocrine Disorders and Reproduction
Practice Questions
Hormonal Evaluation and Testing
Practice Questions
Ovulation Induction
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
